Synergistic Effects of Acoustics-based Therapy and Immunotherapy in Cancer Treatment
1MOE Key Laboratory of Macromolecular Synthesis and Functionalization, Ministry of Education, Department of Polymer Science and Engineering, Zhejiang University, Hangzhou, China
2Department of Ultrasound in Medicine, Second Affiliated Hospital of Zhejiang University School of Medicine, Zhejiang University, Hangzhou, China
*Correspondence to: Pintong Huang, E-mail: huangpintong@zju.edu.cn; Weijun Tong, E-mail: tongwj@zju.edu.cn
Received: March 11 2021; Revised: March 31 2021; Accepted: April 17 2021; Published Online: May 6 2021
Cite this paper:
Yuheng Bao, Jifan Chen, Pintong Huang and Weijun Tong. Synergistic Effects of Acoustics-based Therapy and Immunotherapy in Cancer Treatment. BIO Integration 2021; 2(2): 61–70.
DOI: 10.15212/bioi-2021-0007. Available at: https://bio-integration.org/
Download citation
© 2021 The Authors. This is an open access article distributed under the terms of the Creative Commons Attribution License (https://creativecommons.org/licenses/by/4.0/). See https://bio-integration.org/copyright-and-permissions/
Abstract
Cancer is an intractable disease and has ability to escape immunological recognition. Cancer immunotherapy to enhance the autogenous immune response to cancer tissue is reported to be the most promising method for cancer treatment. After the release of damage-associated molecular patterns, dendritic cells come mature and then recruit activated T cells to induce immune response. To trigger the release of cancer associated antigens, cancer acoustics-based therapy has various prominent advantages and has been reported in various research. In this review, we classified the acoustics-based therapy into sonopyrolysis-, sonoporation-, and sonoluminescence-based therapy. Then, detailed mechanisms of these therapies are discussed to show the status of cancer immunotherapy induced by acoustics-based therapy in quo. Finally, we express some future prospects in this research field and make some predictions of its development direction.
Keywords
Acoustics-based therapy, cancer treatment, immune response activation, immunotherapy.
Introduction
Cancer is a severe threat toward human health worldwide, and its high death rate has raised great concerns. In 2015, more than 4.2 million new cases and 2.8 million new deaths were projected to take place in China by the National Central Cancer Registry of China [1]. Thus, safe and efficient cancer therapies are very important. Because it is widely accepted that innate and acquired alternations in gene expression cause cancer, the enhancement of the abilities of the host immune system seems to be a powerful and biomedical safe method. Thus, cancer immunotherapy has been proposed as a long-term anti-cancer method to train or activate the immunological systems to recognize, conquer, and eliminate cancer cells [2]. By now, the anti-cancer effect of immunotherapy has been proven in various malignant cancer models and is expected to be widely used for its clinical process [3, 4].
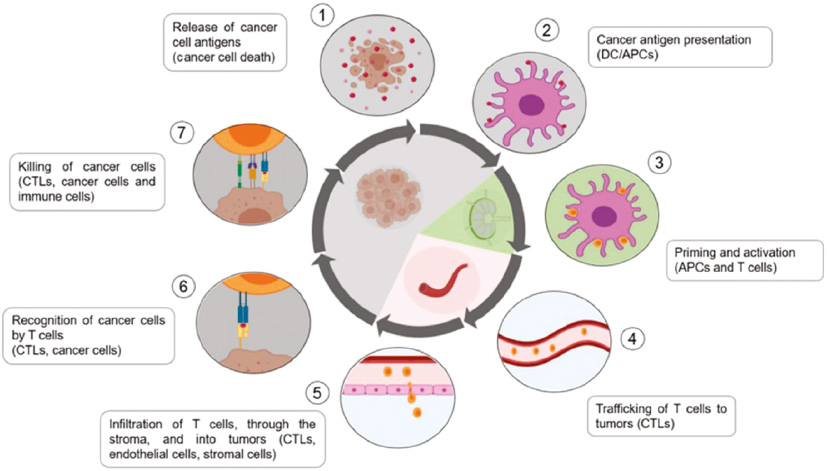
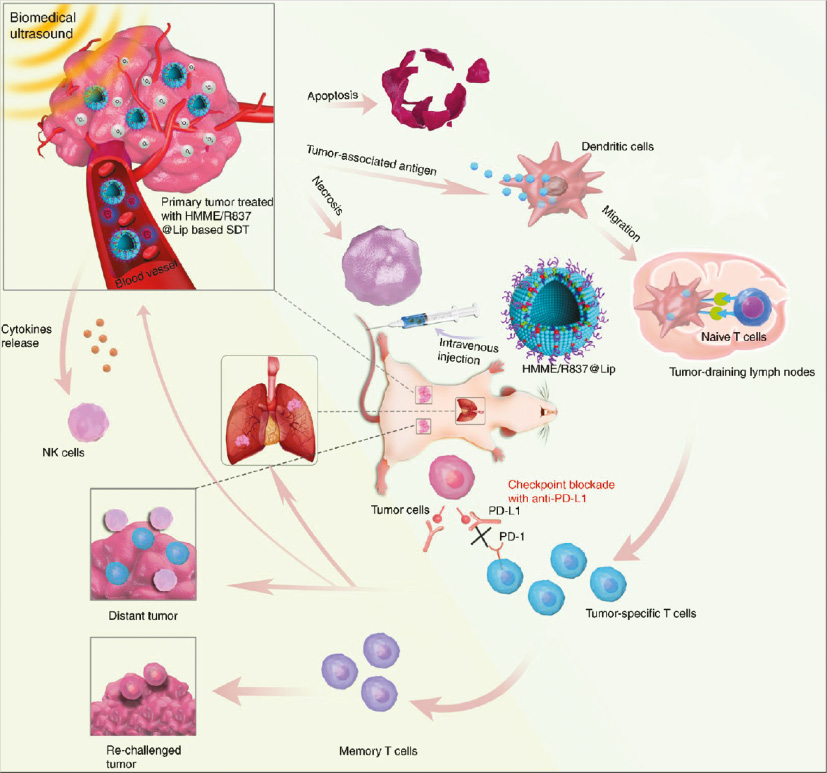
In immunotherapy, the most important step is to trigger the anti-cancer immune responses of human’s immune system [5, 6]. The detailed mechanism of cancer immunotherapy is illustrated in Figure 1. Damage-associated molecular patterns (DAMPs), signals released after the damage brought about by cancer cells, are essential in the immune activation process of cancer [7]. In this process, dendritic cells (DCs) function as antigen-presenting cells and migrate toward cancer-draining lymph nodes after recognizing DAMPs [8]. Afterward, native T cells mature with the induction of antigens presented by DCs and initiate the immune responses [9]. The excited T cells automatically cycle in the human body and then trigger immunogenic cell death (ICD) after immunological recognition toward cancer cells [10].
Figure 1 Molecular mechanism of ICD induced by cancer immunotherapy. Step 1: Released DAMPs captured by DCs. Step 2: Presentation of DAMPs to T cells by dendritic cells. Step 3: Effector T-cell activation against specific cancer antigens. Step 4: T-cell migration to the cancer site. Step 5: Infiltration of the tumor bed. Step 6: Recognition and binding to cancer cells. Step 7: ICD of cancer cells and release of DAMPs. Reproduced with permission [10]. Copyright 2020, MDPI.
Considering a noninvasive cancer treatment to fight against the local cancer and induce the release of DAMPs, chemotherapy and radiotherapy have been widely studied in clinical cancer treatment trails [11]. Although these traditional representative therapy methods have great ability to lead to cancer death, they simultaneously have severe side effects to the human body and decrease the immunity of patients [12, 13]. To cause local cancer death and to enhance patient compliance, photics-based cancer therapies have been widely studied for their good effect and low systemic toxicity. Only the tissues in light-focus regions are affected by photics-based cancer treatments and thereafter exhibit cell apoptosis and necrosis. Acoustics-based cancer therapies are derived from photics-based cancer therapies, but they additionally have a variety of advantages. They have a greater penetration and lower radiation damage, offering a better targeted effect toward cancer in deep tissues and organs. The acoustics-based treatment is also beneficial to the infiltration of drugs and immune cells and the release of DAMPs, which gives incomparable advantages compared with other synergistic immune treatments. Moreover, acoustics-based methods have low costs, great controllability, and high biomedical safety [14]. For the aforementioned considerations, we suppose that acoustics-based cancer treatments might be the most promising method for inducing ICD for synergistic cancer immunotherapy.
Mechanisms of acoustics-based immunotherapy
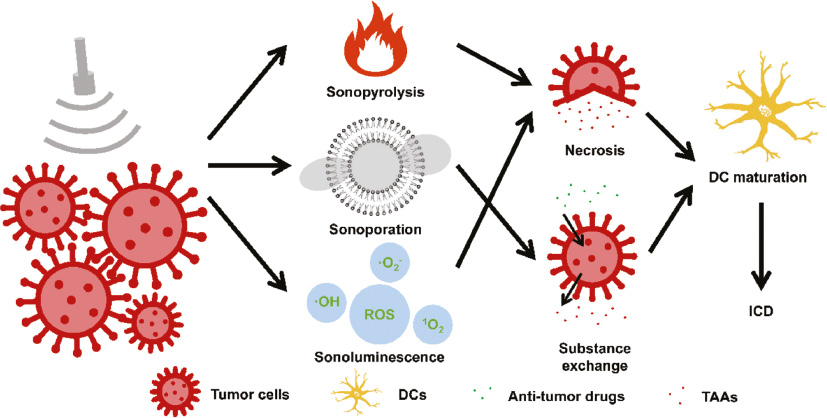
High-intensity focused ultrasound (HIFU) is a clinically used technology for local thermal ablation of cancer [15]. HIFU is a truly non-invasive therapeutic method, which is harmless to the intervening skin and tissues toward the target cancer. However, the energy level of the focused region is sufficient to cause instantaneous cell death [16]. In HIFU, ultrasound is focused on cancer sites, and the local temperature is rapidly increased to cause blockage of nutrient vessels at the targeted area and coagulative necrosis of the cancer tissue (Figure 2). This temperature-based treatment method is also called sonopyrolysis. Although thermal effect offers major impact in sonopyrolysis, the cavitation effect of HIFU gives rise to the collapse of the membrane structure at the targeted region [17]. Compared with systemic chemotherapy, local HIFU treatment has greater accuracy in positioning and lower side effects. After the destruction of the primary cancer by the thermal effect of HIFU, tissue fragments are released from the cancer region and are recognized by the immune system, causing immune activation in vivo [18]. Although some immune responses are observed in HIFU-based cancer thermal ablation therapy, recurrence or systemic metastasis after treatment is often observed [19]. This is due to the failure of the systemic anti-cancer adaptive immunity to activate in this treatment. Meanwhile, the blood supply in the cancer region is reduced after the destruction of cancer tissues and vessels structures, which greatly inhibits the infiltration of circulating immune cells into the cancer site [20].
Figure 2 Processing mechanism of acoustics-based therapy–induced cancer ICD through sonopyrolysis, sonoporation, and sonoluminescence. In all of these therapies, TAAs are released from cancer cells to mature DCs and eventually induce ICD of cancer.
Therefore, a novel strategy of activating the immune response toward cancer without completely destroying the cancer structure is required. Low-intensity focused ultrasound (LIFU) has low thermal damage, can be repeatedly operated, and can maintain the structural integrity of cancer. The ultrasonic intensity in LIFU is relatively low, which is lower than or similar to that used in diagnosis [21]. It is a new kind of noninvasive and effective method, which has a broad application prospect [22]. The thermal effect by LIFU is not significant, and the probable mechanism of LIFU-based cancer therapy is acoustic cavitation. That is, the irradiation of LIFU interacts with surrounding aqueous solutions and produces high-intensity pressure waves and shockwaves locally, accompanied by high-speed micro-jet and free radicals. These strong waves may result in DNA rupture, cell necrosis, tissue hemorrhage, and damage [23]. The cavitation effect can be further divided into two components, sonoporation effect and sonoluminescence effect, and their detailed mechanisms are presented in Figure 2.
For the sonoporation effect, the mechanical action of ultrasonic waves is utilized, and a series of biological changes are triggered at targeted cancer sites. The intense pulses of ultrasound can induce temporary pores in the cell membrane as well as enhance exchange of substance [24]. Cavitation nuclei, such as microbubbles (MBs), are combined with LIFU to increase adjustability, reduce cavitation threshold, and enhance cavitation effect [25]. The proper adjustment of cavitation parameters can spur local inflammation and enhance local blood supply; thus, further infiltration of immune cells and drugs in cancer sites can be achieved after LIFU irradiation [26]. In addition, the cavitation effect is also beneficial to the production of micro-jet flows by sonoporation, which can destroy the membrane structure of cancer cells, promoting the production and release of tumor-associated antigens (TAAs) [27]. Because of the aforementioned functions, sonoporation effect is beneficial to the exchange of substances in cancer sites.
Treatment through sonoluminescence effect is also regarded as sonodynamic therapy (SDT). This path is due to the generation of luminol light during ultrasonic irradiation at stable or inertial cavitation [28]. Sonosensitizers are activated by this photic energy to produce electrons (e+) and holes (e–), and finally, reactive oxygen species (ROS) is formed at targeted cancer sites [29]. When the oxidative stress level of cancer cells exceeds the cellular limit and disrupts the balance, cancer cells are wiped out and immunogenic signals are released from primary cancer regions [30]. Later on, acquired immunity is activated after recognition and finally contributes to the ICD of cancer. The major mechanisms of acoustic-based immunotherapy and their derived biochemical effects and applications in research are presented in Table 1.
Table 1 Major Mechanisms of Acoustic-based Immunotherapy and Their Derived Biochemical Effects and Applications in Research
| Ultrasound type | Major mechanisms | Derived effects | References |
|---|---|---|---|
| High-intensity focused ultrasound | Sonopyrolysis | Thermal ablation | [33–35] |
| Regulation of cancer microenvironment | [36] | ||
| Temperature-sensitive release | [37] | ||
| Low-intensity focused ultrasound | Sonoporation | Protein and factors delivery | [41, 42] |
| DNA/RNA delivery | [43–45] | ||
| Chemotherapy drug delivery | [46–48] | ||
| Sonoluminescence | Cancer-targeted reactive oxygen species production | [51–55] |
Sonopyrolysis-induced immunotherapy
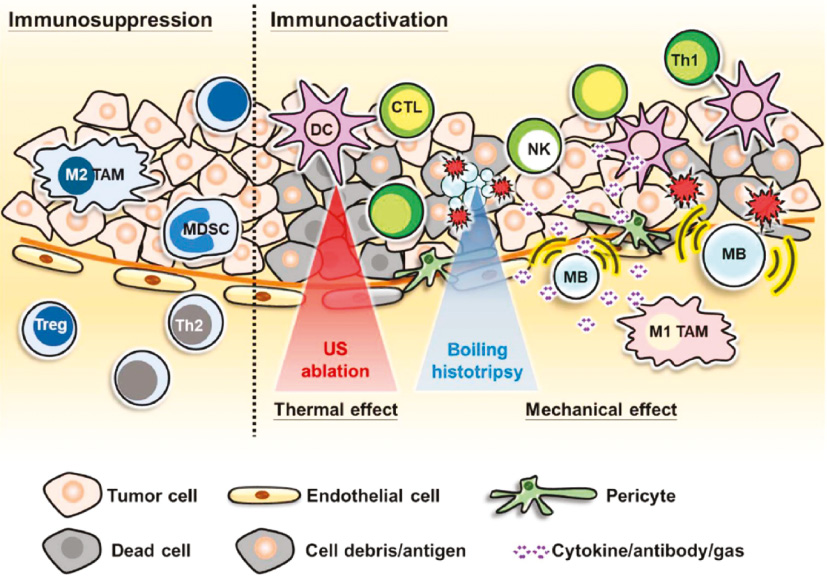
Based on previous studies of various cancer ablation methods (laser irradiation, radiofrequency, microwaves, etc.), we have summarized the basic regulation of local temperature increase–induced cell death. That is, when temperature is >56°C, coagulative cell necrosis immediately takes place at targeted cancer sites [18]. In cancer treatment of HIFU ablation, the temperature of focused center can immediately reach approximately 100°C, which can induce in vivo protein denaturation, cell shrinkage, membrane rupture, and finally, coagulative necrosis of cancer cells [31]. At the same time, the surrounding cancer blood vessels also exhibit structural and functional changes or even immediate destruction after thermal ablation, leading to lack of nutrition and oxygen in the cancer region. This effect also contributes to cancer necrosis and further immune response [32]. The detailed mechanism is illustrated in Figure 3.
Figure 3 Schematic illustration of the thermal and mechanical effects of high-intensity focused ultrasound to promote the activation and infiltration of immune cells for anti-cancer immunotherapy. Reproduced with permission [22]. Copyright 2020, Elsevier BV.
Xia et al. studied the anti-cancer cellular immunity induction of H22 hepatic cancer-bearing mice after HIFU irradiation [33]. A total of 105 mice were randomly divided into three groups and were treated with HIFU or with sham HIFU or were not treated. After 14 days, mice were sacrificed, and a significant function variation (p<0.001) of T lymphocytes was determined by measuring interferon γ (IFN-γ) and tumor necrosis factor α (TNF-α) secretion. Furthermore, the frequency of the major histocompatibility complex class I tetramer/CD8-positive cells and the survival rates of HIFU group were significantly higher (p<0.01) than other two groups, thus demonstrating that HIFU ablation can trigger immune responses in cancer-bearing mice by activating cancer-specific T lymphocytes. A similar model was set up by Ran’s group [34], and they reported that the CD3+ and CD4+ levels and CD4+/CD8+ ratio in peripheral blood significantly (p<0.05) increased in HIFU-treated group. To further prove the mechanism of HIFU-triggered immune response, Deng et al. used cancer debris derived from the H22 cancer model after HIFU ablation as activating signals [35]. Bone marrow–derived DCs were loaded with debris and were used to immunize mature mice to trigger the acquired immunity. The treated mice were rechallenged by H22 cancer. Similar to the HIFU-treated group, the number of mature DCs and splenic lymphocytes in the cancer debris–treated group significantly increased (p<0.01). The secretion of interleukin 12 (IL-12) and interferon γ was also higher in these two groups than in the control group, implying that DCs were activated by cancer debris and therefore initiated the acquired anti-cancer immune response in the H22 cancer re-challenge.
Sethuraman et al. used novel calreticulin-based nanoparticles (CRT-NPs) in combination with HIFU to upregulate CRT expression in solid cancer and improve anti-cancer effects after cancer ablation [36]. Their results showed that functional CD4+ and CD8+ cytotoxic T cells specific to melanoma TRP-2 and M1 phenotype macrophage cells expanded in the re-challenge assay, and the growth of B16 melanoma was suppressed by over 85% with controls and over 50% with CRT-NPs or HIFU-alone groups. Kheirolomoom et al. studied the activatable delivery of temperature-sensitive liposomes after HIFU irradiation [37]. In this work, liposomes could rapidly release free doxorubicin (DOX) and type I interferons in the vasculature of cancer lesions after ultrasound induction. The release of drugs in liposomes initiates cancer necrosis and viral-like immune response, and cancer eradication was observed in both treated and distant tumors of mice.
Although thermal effect is the major mechanism in HIFU-based cancer therapy, non-thermal mechanical destruction of the cancer region can also trigger immunomodulated effect [38]. This method mainly appears to work with acoustic cavitation. At high acoustic pressure, the positive (compression) peak of the sinusoidal wave travels faster than the negative (rarefraction) peak of the wave due to the non-linear acoustic wave propagation, resulting in shockwaves when the penetration of tissue by ultrasound occurs [39]. During HIFU treatment, boiling MBs are induced by thermal effects, and the cavitation effect takes place when the negative pressure is high enough to overcome the surface tension of the gas nuclei in the cancer tissue. More examples are presented in the next section.
Sonoporation-induced immunotherapy
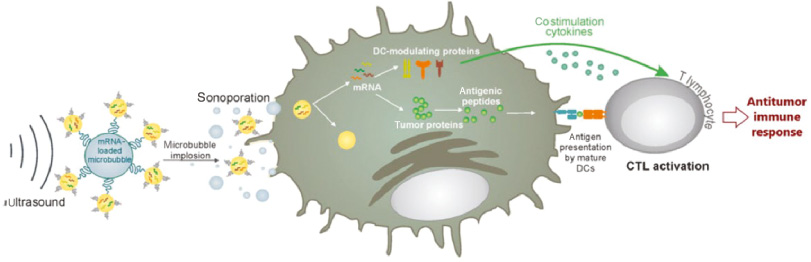
As sonopyrolysis cancer therapy inevitably causes injury or damage toward surrounding tissues, LIFU, which is mainly based on the mechanical effect of acoustic waves, seems to be feasible alternative to HIFU. Unlike thermal-induced MBs in cancer ablation, LIFU-based cavitation relies on the gas MBs injected into vessels [40]. Under LIFU treatments, MBs non-linearly oscillate and expand more than twice the initial size and then rupture, causing high acoustic pressure (several thousand atmospheres) in a local cancer area [27]. This mechanism contributes to the temporary loosening of the dense cancer stroma, which is beneficial for drug delivery and immune cell infiltration of the cancer cells. Additionally, severe sonoporation enables the formation of pores on the cell membranes of cancer, and DAMPs may be easily released and monitored by the immune system, resulting in more drastic immune response. The mechanism of sonoporation-induced immunotherapy is shown in Figure 4.
Figure 4 Schematic illustration of MB implosion upon ultrasound exposure to sonoporate the dendritic cell (DCs). Antigens and modulating proteins are produced by the DC and lead to antigen presentation and T-cell activation. Reproduced with permission [43]. Copyright 2014, Elsevier BV.
Chen et al. explored the enhancement of IL-12 delivery across the blood–brain barrier and the subsequent immunity promotion after induction of LIFU [41]. Combined with MBs, focused ultrasound could temporarily and locally open the blood–brain barrier. Evaluation of the immunological response to IL-12 delivery showed that, compared with IL-12 alone, local IL-12 deposition in brain cancer was 2.87-fold higher and patients had 42.9% survival improvement. In another research, perfluoropropane gas-entrapping liposomes were used by Suzuki et al. to deliver ovalbumin (OVA), a model cancer antigen, to DCs [42]. Their results indicated that exogenous antigens can also be recognized after delivery into the cytosol of DCs, and complete rejection of endogenous E.G7-OVA cancer was exhibited in cancer-bearing mice. Dewitte’s group studied the improved mRNA delivery to DCs and immunoregulation effect by TriMix MBs [43]. Cancer antigen mRNA was loaded in MBs to form in vivo DC vaccines, and transfection of DCs was triggered by focused ultrasound. Antigen-specific T cells were induced by sonoporation, and specific lysis of antigen-expressing cells occurs. Then, 30% of experimental animals displayed complete cancer regression, and long-term antigen-specific immunological memory was observed. The LIFU-induced sonoporation effect can also facilitate the transfection of DNA to cancer and stromal cells [44, 45], thus enhancing the secretion of cancer-related antigens for immunotherapy. In both works, transfection inhibited cancer growth in vivo, and cytotoxic immune cells were recruited to remove primary and distant cancers.
Anti-programmed cell death protein 1 (PD-1)/programmed death-ligand 1 (PD-L1) antibodies are typical checkpoint inhibitors that can block the binding of PD-1-inhibited molecules to their receptor on cytotoxic T cells. The procedure of cancer immunotherapy activated by ultrasound combined with PD-1 inhibitors is shown in Figure 5. Zheng et al. studied the effect of ultrasound irradiation in DOX- and anti-PD-1–based combined chemo-immunotherapy in the model of B-cell lymphoma mice [46]. The results confirmed that ultrasound irradiation is beneficial for the targeted accumulation and controllable release of DOX in cancer site, and a significant inhibitory effect was observed on cancer irradiated with ultrasound and inhibited with PD-1 checkpoint. Li’s group used anti-PD-L1 monoclonal antibody–conjugated lipid MBs as cancer-targeted carriers to deliver docetaxel, a chemotherapeutic drug for non-small cell lung cancer [47]. Combined with ultrasonic irradiation, docetaxel-loaded MBs showed a higher cellular uptake and increased rate of cellular apoptosis. In addition, enhanced G2-M arrest rate in cancers were observed, which was positively correlated with PD-L1 expression in cancer cells, indicating the synergistic chemo-immunotherapy. Bulner’s group set up a colorectal cancer cell line CT26 model and proposed the possibility of synergistic effect of chemotherapy-based MBs and PD-1–based immunotherapy [48]. In this study, enhanced cancer growth inhibition and increased animal survival relative to monotherapy method was proven.
Figure 5 Schematic illustration of MBs with ultrasound irradiation to provide the possibility of combining with programmed cell death protein 1 inhibitor and increasing the anti-cancer activity in B-cell lymphoma. RDM: rituximab-conjugated and doxorubicin-loaded MB. Reproduced with permission [46]. Copyright 2018, Future Medicine Ltd.
Sonoluminescence-induced immunotherapy
Sonoluminescence effect is often used in SDT, which is a local treatment method derived from photodynamic therapy (PDT) [49]. In PDT, photosensitizers are exposed to a specific wavelength of light and activated from a ground state to an excited state. When they return to the ground state, the released energy generates ROS, such as free radicals and singlet oxygen, to trigger local cellular apoptosis and necrosis. A similar mechanism is exhibited in SDT, and sonosensitizers are used as mediums to utilize the ultrasound energy for ROS generation at cancer sites [50]. Compared with PDT, SDT has the capability to conquer the deeper in situ cancer and cause fewer side effects such as thermal toxicity [31]. The details of the anti-cancer immune responses induced by noninvasive SDT and synergistic immunotherapy are shown in Figure 6.
Figure 6 Schematic illustration of anti-cancer immune responses induced by noninvasive SDT with immune-adjuvant–contained nanosonosensitizers and checkpoint blockade for cancer immunotherapy. Reproduced with permission [53]. Copyright 2019, Springer Nature Limited.
Zhang et al. used the human liver cancer cell line Hep3b to set up an in vivo mice cancer model and studied the HiPorfin-induced SDT effect and its subsequent immunological memory triggering [51]. A significant difference (p<0.001) in cellular ROS level and apoptotic rate was observed between the experimental and control groups, and the cancer volume in cancer-bearing mice in the experimental group was relatively controlled. Later, through immunohistochemical analysis of cancer tissue and cancer re-challenging assay, the cured mice were completely resistant to the re-challenge and showed high expression levels of CD4, CD8, and CD68, and low expression levels of CD163, CD25, and FoxP3, suggesting the activation of T cells during SDT. Xie’s group used phase-shifted nanoparticles loaded with perfluoropentane, indocyanine green, and oxaliplatin to augment the anti-cancer immunological effects by synergistic chemotherapy, PDT, and SDT [52]. Under the induction of near-infrared light and ultrasound, the anti-cancer effects were determined in cellular and in vivo studies. In addition, a significantly enhanced expression of DAMPs was observed in cancer model mice, thus indicating a long-term immune response effect.
Based on this mechanism, a mass of multifunctional sensitizers has been developed for sonoluminescence-induced immunotherapy in various research. Yue’s group co-loaded sonosensitizer hematoporphyrin monomethyl ether and immune adjuvants TLR7 agonist R837 in liposomes to elicit an immune response [53]. Combined with PD-L1 injection, this platform showed long-term immunological memory through PD-1/PD-L1 blockage, elimination effect of the initial and distant cancers, and protection against cancer re-challenge. Um et al. synthesized chlorin e6–based amphiphilic sonosensitizers and loaded PFP to form ultrasonic responsive nanobubbles [54]. After exposure to ultrasound, the generation of ROS induced cancer necroptosis. Simultaneously, perfluoropentane nanobubbles showed sonoporation effect and active DAMPs were easier to release due to the disintegration of cell membrane, thus improving anti-cancer immune response by the maturation of DCs and activation of CD8+ cytotoxic T cells. Zhao et al. reported a biomimetic decoy to enhance ICD-mediated immunotherapy by synergistic chemo-sonodynamic therapy [55]. Hybrid red blood cell and platelet membrane were used to enhance the in vivo biosafety, circulation time, and cancer-targeted ability of nanoplatforms. Although loaded chlorin e6 was able to produce ROS under ultrasonic irradiation, the carried tirapazamine could function at hypoxic cancer microenvironment and achieve augmented cancer necrosis and DAMP release effect.
Conclusion and prospects
Immunotherapy, a method to enhance autogenous acquired immunity, offers great opportunity for the eradication of cancers. One critical step is to capture the DAMPs of cancer tissue by DCs and induce its maturation process. Acoustics-based cancer therapies use ultrasound irradiation to trigger cancer cell apoptosis or necrosis to induce the release of DAMPs, thus inducing the presentation of TAAs to DCs. Compared with other therapies, acoustic-based therapy has unique advantages of low costs, great controllability, high biomedical safety, deeper penetration, lower irradiation damage, better infiltration of drugs, immune cells, and augmented release of DAMPs. Therefore, it is a very promising method for synergistic cancer immunotherapy.
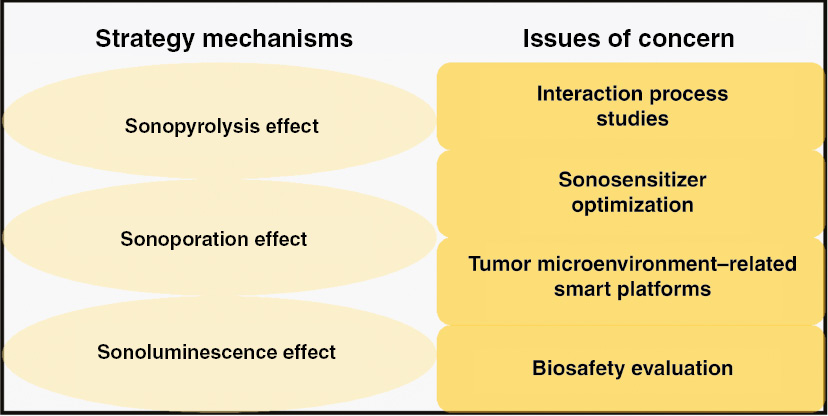
In this review, we provided three major mechanisms of acoustics-based therapy: sonopyrolysis effect, sonoporation effect, and sonoluminescence effect. Cutting-edge research on synergistic cancer treatment of immunotherapy with these three therapeutic methods has been collected and discussed. Among these strategies, sonopyrolysis-induced immunotherapy utilizes thermal effect of focused ultrasound to kill cancer cells, which has relatively great side effects to common cells. In contrast, because of the transient function time and limited impact region of microjet and ROS, immunotherapy induced by sonoporation and sonoluminescence effect has greater biosafety. In addition, the overall structure of the cancer region is retained, which is beneficial to the permeation of immunological cells and immunity activation, reducing recurrence or systemic metastasis after treatment. In comparison, sonoporation-induced immunotherapy is often associated with chemotherapy to produce DAMPs, whereas sonoluminescence can eliminate cancer cells and induce immunotherapy. Furthermore, several concerns should be considered before clinical trials, as summarized in Figure 7 and discussed as follows.
Figure 7 Schematic illustration of the different mechanisms of acoustics-based immunotherapy strategy and diverse issues for future research in order to determine the feasibility and effectiveness of this strategy.
Interaction process studies
The cancer therapy ability of acoustics-based therapy has been widely verified both in vitro and in vivo, but the therapeutic effect is mostly based on researchers’ repeated trials, which is unforeseeable and cumbersome. It is necessary for researchers to look for detailed mechanisms. Up to now, despite many hypotheses that have been put forward, such thermal effect and cavitation effect, further understanding in physicochemical process remains to be studied [56]. Furthermore, the mechanism of triggering of cancer immunotherapy by acoustics-based therapy is not proven. Research is mainly focused on the detection of DCs’ final maturation, which lacks the monitoring of the release of DAMPs. In our viewpoint, to determine the augmenting antigen–presenting effect toward DCs, the DAMPs level before and after cancer acoustics-based therapy have to be evaluated. This is a complex field involving macroscopically mechanical interactions and microscopically molecular interactions, which requires interdisciplinary knowledge, such as physical acoustics, analog simulation, material science, and biomedical science.
Sonosensitizer optimization
For SDT, organic and inorganic sonosensitizers have already been utilized for cancer ROS level augmentation, but several crucial problems of sonosensitizers remain to be solved. First, most sonosensitizers are hydrophobic, which are insoluble in aqueous solutions or buffers, leading to the low biocompatibility, fast elimination, and short circulation time in vivo. Nanocarrier loading or surface modification may be two major resolutions. Nanocarriers, especially mesoporous and hollow carriers, can be used to load sonosensitizers based on hydrophobic interaction [29]. Therein, porphyrin-based metal–organic and covalent–organic frameworks are two promising nanostructures to avoid self-quenching [57]. For surface modification, hydrophobic sensitizers can be functionalized with hydrophilic chains to form amphiphilic porphyrin molecules [58]. Supramolecular self-assembly interaction takes place in aqueous solution, and porphyrin-based vesicles or micelles are then obtained for cancer-targeted sonosensitizer delivery [59].
Tumor microenvironment–related smart platforms
Smart nanoplatforms have been raised as a topic for cancer-targeted therapy. These designs are mainly focused on local application of nanomaterials and enhanced therapy effect only in cancer sites while staying out of operation during body circulation, leading to augmented delivery efficiency and lower injection dose of sensitizers. Low pH [60], hypoxia [61], high ROS [62], and glutathione level [63] are typical characteristics of the tumor microenvironment (TME), which are promising in the design of TME-responsive systems. These smart platforms give rise to acoustics-based therapy and activate immune response after delivery to targeted cancer sites. Nanoplatforms are also used to regulate or remodel TME, that is, the physicochemical property and immune property of TME are adjusted. The relief of cancer hypoxia and local glutathione depletion are beneficial to augmented local ROS production, thus promoting the release of cancer DAMPs. Meanwhile, the immune TME can be remodeled by immune cells infiltration enhancement, checkpoint inhibition, macrophage phenotype regulation, and cytokine levels adjustment. As ultrasound-mediated bubble sonoporation is an efficient method for the infiltration of macrophages and DCs, the activation of cancer DAMPs recognition and immune response can be thus improved to achieve better cancer therapy efficacy.
Biosafety evaluation
Biocompatibility is a crucial property of biomaterials; thus, in vivo biosafety evaluation is necessary for clinical trials of synergistic therapy strategies. However, recent researchers only evaluated in vivo toxicity for less than 30 days, thus lacking long-term monitoring. If possible, the biosafety evaluation time should be prolonged. Moreover, aside from mice, more high-class animal models, such as rabbits and monkeys, should be established in some advanced studies.
Conflicts of interests
The authors declare that they have no competing interests.
Acknowledgement
This work was supported by the National Key R&D Program of China (no. 2018YFC0115900), National Nature Science Foundation of China (grant nos. 82030048, 51973187, 81901871, and 81527803), Zhejiang Science and Technology Project (no. 2019C03077), and Natural Science Foundation of Zhejiang Province (LQ19H180004, LQ20H180009, and LQ21H180007).
References
- Chen W, Zheng R, Baade DP, Zhang S, Zeng H, et al. Cancer statistics in China, 2015. CA Cancer J Clin 2016;66:115-32. [PMID: 26808342 DOI: 10.3322/caac.21338]
- Duan X, Chan C, Lin W. Nanoparticle-mediated immunogenic cell death enables and potentiates cancer immunotherapy. Angew Chem Int Ed 2019;58:670-80. [PMID: 30016571 DOI: 10.1002/anie.201804882]
- Pardoll DM. The blockade of immune checkpoints in cancer immunotherapy. Nat Rev Cancer 2012;12:252-64. [PMID: 22437870 DOI: 10.1038/nrc3239]
- Musetti S, Huang L. Nanoparticle-mediated remodeling of the tumor microenvironment to enhance immunotherapy. ACS Nano 2018;12:11740-55. [PMID: 30508378 DOI: 10.1021/acsnano.8b05893]
- Liu J, Xu M, Yuan Z. Immunoscore guided cold tumors to acquire “temperature” through integrating physicochemical and biological methods. BIO Integration 2020;1:6-14. [DOI: 10.15212/bioi-2020-0002].
- Sprooten J, De Wijngaert P, Vanmeerbeek I, Martin S, Vangheluwe P, et al. Necroptosis in immuno-oncology and cancer immunotherapy. Cells 2020;9:1823. [PMID: 32752206 DOI: 10.3390/cells9081823]
- Kroemer G, Galluzzi L, Kepp O, Zitvogel L. Immunogenic cell death in cancer therapy. Annu Rev Immunol 2013;31:51-72. [PMID: 23157435 DOI: 10.1146/annurev-immunol-032712-100008]
- Turnbull E, MacPherson G. Immunobiology of dendritic cells in the rat. Immunol Rev 2001;184:58-68. [PMID: 12086321 DOI: 10.1034/j.1600-065x.2001.1840106.x]
- Montico B, Nigro A, Casolaro V, Dal Col J. Immunogenic apoptosis as a novel tool for anticancer vaccine development. Int J Mol Sci 2018;19:594. [PMID: 29462947 DOI: 10.3390/ijms19020594]
- Acebes-Fernández V, Landeira-Viñuela A, Juanes-Velasco P, Hernández AP, Otazo-Perez A, et al. Nanomedicine and onco-immunotherapy: from the bench to bedside to biomarkers. Nanomaterials 2020;10:1274. [PMID: 32610601 DOI: 10.3390/nano10071274]
- Li X. The inducers of immunogenic cell death for tumor immunotherapy. Tumori 2018;104:1-8. [PMID: 28967094 DOI: 10.5301/tj.5000675]
- Luo Q, Zhang L, Luo C, Jiang M. Emerging strategies in cancer therapy combining chemotherapy with immunotherapy. Cancer Lett 2019;454:191-203. [PMID: 30998963 DOI: 10.1016/j.canlet.2019.04.017]
- Zitvogel L, Apetoh L, Ghiringhelli F, André F, Tesniere A, et al. The anticancer immune response: indispensable for therapeutic success? J Clin Invest 2008;118:1991-2001. [PMID: 18523649 DOI: 10.1172/JCI35180]
- Huang P. An integrated approach to ultrasound imaging in medicine and biology. BIO Integration 2020;1:105-9. [DOI: 10.15212/bioi-2020-0036].
- Kotewall N, Lang BHH. High-intensity focused ultrasound ablation as a treatment for benign thyroid diseases: the present and future. Ultrasonography 2019;38:135-42. [PMID: 30690961 DOI: 10.14366/usg.18040]
- Kennedy JE. High-intensity focused ultrasound in the treatment of solid tumours. Nat Rev Cancer 2005;5:321-7. [PMID: 15776004 DOI: 10.1038/nrc1591]
- Cohen-Inbar O, Xu Z, Sheehan JP. Focused ultrasound-aided immunomodulation in glioblastoma multiforme: a therapeutic concept. J Ther Ultrasound 2016;4:2. [PMID: 26807257 DOI: 10.1186/s40349-016-0046-y]
- Wu F. High intensity focused ultrasound ablation and antitumor immune response. J Acoust Soc Am 2013;134:1695-701. [PMID: 23927210 DOI: 10.1121/1.4812893]
- Wu F, Wang ZB, Chen WZ, Zou JZ, Bai J, et al. Extracorporeal focused ultrasound surgery for treatment of human solid carcinomas: early Chinese clinical experience. Ultrasound Med Biol 2004;30:245-60. [PMID: 14998677 DOI: 10.1016/j.ultrasmedbio.2003.10.010]
- van den Bijgaart RJE, Eikelenboom DC, Hoogenboom M, Fütterer JJ, den Brok MH, et al. Thermal and mechanical high-intensity focused ultrasound: perspectives on tumor ablation, immune effects and combination strategies. Cancer Immunol Immunother 2016;66:247-58. [PMID: 27585790 DOI: 10.1007/s00262-016-1891-9]
- Baek H, Pahk KJ, Kim H. A review of low-intensity focused ultrasound for neuromodulation. Biomed Eng Lett 2017;7:135-42. [PMID: 30603160 DOI: 10.1007/s13534-016-0007-y]
- Ho YJ, Li JP, Fan CH, Liu HL, Yeh CK. Ultrasound in tumor immunotherapy: current status and future developments. J Control Release 2020;323:12-23. [PMID: 32302759 DOI: 10.1016/j.jconrel.2020.04.023]
- Unga J, Hashida M. Ultrasound induced cancer immunotherapy. Adv Drug Deliv Rev 2014;72:144-53. [PMID: 24680708 DOI: 10.1016/j.addr.2014.03.004]
- Lentacker I, De Cock I, Deckers R, De Smedt SC, Moonen CT. Understanding ultrasound induced sonoporation: definitions and underlying mechanisms. Adv Drug Deliv Rev 2014;72:49-64. [PMID: 24270006 DOI: 10.1016/j.addr.2013.11.008]
- Omata D, Unga J, Suzuki R, Maruyama K. Lipid-based microbubbles and ultrasound for therapeutic application. Adv Drug Deliv Rev 2020;154-5:236-44. [PMID: 32659255 DOI: 10.1016/j.addr.2020.07.005]
- Xu W, Zhang X, Hu X, Zhiyi C, Huang P. Translational prospects of ultrasound-mediated tumor immunotherapy: preclinical advances and safety considerations. Cancer Lett 2019;460:86-95. [PMID: 31254552 DOI: 10.1016/j.canlet.2019.06.017]
- Tu J, Zhang H, Yu J, Liufu C, Chen Z. Ultrasound-mediated microbubble destruction: a new method in cancer immunotherapy. Oncol Targets Ther 2018;11:5763-75. [PMID: 30254469 DOI: 10.2147/OTT.S171019]
- Qian X, Zheng Y, Chen Y. Micro/nanoparticle-augmented sonodynamic therapy (SDT): breaking the depth shallow of photoactivation. Adv Mater 2016;28:8097-129. [PMID: 27384408 DOI: 10.1002/adma.201602012]
- Xu M, Zhou L, Zheng L, Zhou Q, Liu K, et al. Sonodynamic therapy-derived multimodal synergistic cancer therapy. Cancer Lett 2021;497:229-42. [PMID: 33122099 DOI: 10.1016/j.canlet.2020.10.037]
- Ma X, Pan H, Yi J. Combination sonodynamic therapy with immunoadjuvant may be a promising new modality for cancer treatment. Med Hypotheses 2009;72:418-20. [PMID: 19128891 DOI: 10.1016/j.mehy.2008.10.024]
- Wu F, Zhou L, Chen WR. Host antitumour immune responses to HIFU ablation. Int J Hyperthermia 2009;23:165-71. [PMID: 17578340 DOI: 10.1080/02656730701206638]
- Pahk KJ, Shin CH, Bae IY, Yang Y, Kim SH, et al. Boiling histotripsy-induced partial mechanical ablation modulates tumour microenvironment by promoting immunogenic cell death of cancers. Sci Rep 2019;9:9050. [PMID: 31227775 DOI: 10.1038/s41598-019-45542-z]
- Xia JZ, Xie FL, Ran LF, Xie XP, Fan YM, et al. High- intensity focused ultrasound tumor ablation activates autologous tumor-specific cytotoxic T lymphocytes. Ultrasound Med Biol 2012;38:1363-71. [PMID: 22633269 DOI: 10.1016/j.ultrasmedbio.2012.03.009]
- Ran LF, Xie XP, Xia JZ, Xie FL, Fan YM, et al. Specific antitumour immunity of HIFU-activated cytotoxic T lymphocytes after adoptive transfusion in tumour-bearing mice. Int J Hyperthermia 2015;32:204-10. [PMID: 26708472 DOI: 10.3109/02656736.2015.1112438]
- Deng J, Zhang Y, Feng J, Wu F. Dendritic cells loaded with ultrasound-ablated tumour induce in vivo specific antitumour immune responses. Ultrasound Med Biol 2010;36:441-8. [PMID: 20172447 DOI: 10.1016/j.ultrasmedbio.2009.12.004]
- Sethuraman SN, Singh MP, Patil G, Li S, Fiering S, et al. Novel calreticulin-nanoparticle in combination with focused ultrasound induces immunogenic cell death in melanoma to enhance antitumor immunity. Theranostics 2020;10:3397-412. [PMID: 32206098 DOI: 10.7150/thno.42243]
- Kheirolomoom A, Silvestrini MT, Ingham ES, Mahakian LM, Tam SM, et al. Combining activatable nanodelivery with immunotherapy in a murine breast cancer model. J Control Release 2019;303:42-54. [PMID: 30978432 DOI: 10.1016/j.jconrel.2019.04.008]
- Mauri G, Nicosia L, Xu Z, Pietrom SD, Monfardini L, et al. Focused ultrasound—tumour ablation and its potential to enhance immunological therapy to cancer. Br J Radiol 2018;91:20170641. [PMID: 29168922 DOI: 10.1259/bjr.20170641]
- Goertz DE. An overview of the influence of therapeutic ultrasound exposures on the vasculature: high intensity ultrasound and microbubble-mediated bioeffects. Int J Hyperthermia 2015;31:134-44. [PMID: 25716770 DOI: 10.3109/02656736.2015.1009179]
- Escoffre JM, Deckers R, Bos C, Moonen C. Bubble-assisted ultrasound: application in immunotherapy and vaccination. Adv Exp Med Biol 2016;880:243-61. [PMID: 26486342 DOI: 10.1007/978-3-319-22536-4_14]
- Chen PY, Hsieh HY, Huang CY, Lin CY, Wei KC, et al. Focused ultrasound-induced blood–brain barrier opening to enhance interleukin-12 delivery for brain tumor immunotherapy: a preclinical feasibility study. J Transl Med 2015;13:93. [PMID: 25784614 DOI: 10.1186/s12967-015-0451-y]
- Suzuki R, Oda Y, Utoguchi N, Namai E, Taira Y, et al. A novel strategy utilizing ultrasound for antigen delivery in dendritic cell-based cancer immunotherapy. J Control Release 2009;133:198-205. [PMID: 19000727 DOI: 10.1016/j.jconrel.2008.10.015]
- Dewitte H, Van Lint S, Heirman C, Thielemans K, De Smedt SC, et al. The potential of antigen and TriMix sonoporation using mRNA-loaded microbubbles for ultrasound-triggered cancer immunotherapy. J Control Release 2014;194:28-36. [PMID: 25151979 DOI: 10.1016/j.jconrel.2014.08.011]
- Yoshida M, Kawakami S, Kono Y, Un K, Higuchi Y, et al. Enhancement of the anti-tumor effect of DNA vaccination using an ultrasound-responsive mannose-modified gene carrier in combination with doxorubicin-encapsulated PEGylated liposomes. Int J Pharm 2014;475:401-7. [PMID: 25218184 DOI: 10.1016/j.ijpharm.2014.09.005]
- Ilovitsh T, Feng Y, Foiret J, Kheirolomoom A, Zhang H, et al. Low-frequency ultrasound-mediated cytokine transfection enhances T cell recruitment at local and distant tumor sites. Proc Natl Acad Sci USA 2020;117:12674-85. [PMID: 32430322 DOI: 10.1073/pnas.1914906117]
- Zheng S, Song D, Jin X, Zhang H, Aldarouish M, et al. Targeted microbubbles with ultrasound irradiation and PD-1 inhibitor to increase antitumor activity in B-cell lymphoma. Nanomedicine 2018;13:297-311. [PMID: 29338562 DOI: 10.2217/nnm-2017-0296]
- Li T, Hu Z, Wang C, Yang J, Zeng C, et al. PD-L1-targeted microbubbles loaded with docetaxel produce a synergistic effect for the treatment of lung cancer under ultrasound irradiation. Biomater Sci 2020;8:1418-30. [PMID: 31942578 DOI: 10.1039/c9bm01575b]
- Bulner S, Prodeus A, Gariepy J, Hynynen K, Goertz DE. Enhancing checkpoint inhibitor therapy with ultrasound stimulated microbubbles. Ultrasound Med Biol 2019;45:500-12. [PMID: 30447880 DOI: 10.1016/j.ultrasmedbio.2018.10.002]
- Pu K, Li J, Luo Y. Electromagnetic nanomedicines for combinational cancer immunotherapy. Angew Chem Int Ed 2020. [PMID: 32671893 DOI: 10.1002/anie.202008386]
- Qian J, Gao Q. Sonodynamic therapy mediated by emodin induces the oxidation of microtubules to facilitate the sonodynamic effect. Ultrasound Med Biol 2018;44:853-60. [PMID: 29398130 DOI: 10.1016/j.ultrasmedbio.2017.12.016]
- Zhang Q, Bao C, Cai X, Jin L, Sun L, et al. Sonodynamic therapy-assisted immunotherapy: a novel modality for cancer treatment. Cancer Sci 2018;109:1330-45. [PMID: 29575297 DOI: 10.1111/cas.13578]
- Xie W, Zhu S, Yang B, Chen C, Chen S, et al. The destruction of laser-induced phase-transition nanoparticles triggered by low-intensity ultrasound: an innovative modality to enhance the immunological treatment of ovarian cancer cells. Int J Nanomedicine 2019;14:9377-93. [PMID: 31819438 DOI: 10.2147/IJN.S208404]
- Yue W, Chen L, Yu L, Zhou B, Yin H, et al. Checkpoint blockade and nanosonosensitizer-augmented noninvasive sonodynamic therapy combination reduces tumour growth and metastases in mice. Nat Commun 2019;10:2025. [PMID: 31048681 DOI: 10.1038/s41467-019-09760-3]
- Um W, Ko H, You DG, Lim S, Kwak G, et al. Necroptosis-inducible polymeric nanobubbles for enhanced cancer sonoimmunotherapy. Adv Mater 2020;32:1907953. [PMID: 32125731 DOI: 10.1002/adma.201907953]
- Zhao H, Zhao B, Li L, Ding K, Xiao H, et al. Biomimetic decoy inhibits tumor growth and lung metastasis by reversing the drawbacks of sonodynamic therapy. Adv Healthcare Mater 2019;9:1901335. [PMID: 31762228 DOI: 10.1002/adhm.201901335]
- Yang Y, Tu J, Yang D, Raymond JL, Roy RA, et al. Photo- and sono-dynamic therapy: a review of mechanisms and considerations for pharmacological agents used in therapy incorporating light and sound. Curr Pharm Des 2019;25:401-12. [PMID: 30674248 DOI: 10.2174/1381612825666190123114107]
- Li T, Li J, Pang Q, Ma L, Tong W, et al. Construction of microreactors for cascade reaction and their potential applications as antibacterial agents. ACS Appl Mater Interfaces 2019;11:6789-95. [PMID: 30702277 DOI: 10.1021/acsami.8b20069]
- Luciano M, Brückner C Modifications of porphyrins and hydroporphyrins for their solubilization in aqueous media. Molecules 2017;22:980. [PMID: 28608838 DOI: 10.3390/molecules22060980]
- Hou W, Xia F, Alves CS, Qian X, Yang Y, et al. MMP2-targeting and redox-responsive PEGylated chlorin e6 nanoparticles for cancer near-infrared imaging and photodynamic therapy. ACS Appl Mater Interfaces 2016;8:1447-57. [PMID: 26638778 DOI: 10.1021/acsami.5b10772]
- An J, Hu YG, Cheng K, Li C, Hou XL, et al. ROS-augmented and tumor-microenvironment responsive biodegradable nanoplatform for enhancing chemo-sonodynamic therapy. Biomaterials 2020;234:119761. [PMID: 31954230 DOI: 10.1016/j.biomaterials.2020.119761]
- Zhang K, Meng X, Yang Z, Dong H, Zhang X. Enhanced cancer therapy by hypoxia-responsive copper metal-organic frameworks nanosystem. Biomaterials 2020;258:120278. [PMID: 32781328 DOI: 10.1016/j.biomaterials.2020.120278]
- Shi J, Chen Z, Wang B, Wang L, Lu T, et al. Reactive oxygen species-manipulated drug release from a smart envelope-type mesoporous titanium nanovehicle for tumor sonodynamic-chemotherapy. ACS Appl Mater Interfaces 2015;7:28554-65. [PMID: 26587885 DOI: 10.1021/acsami.5b09937]
- Lin X, Liu S, Zhang X, Zhu R, Chen S, et al. An ultrasound activated vesicle of Janus Au-MnO nanoparticles for promoted tumor penetration and sono-chemodynamic therapy of orthotopic liver cancer. Angew Chem Int Ed 2019;59:1682-8. [PMID: 31710768 DOI: 10.1002/anie.201912768]