The Integration of Reactive Oxygen Species Generation and Prodrug Activation for Cancer Therapy
1School of Life Sciences, Tianjin University, Tianjin 300072, China
*Correspondence to: Sheng Wang, E-mail: shengwang@tju.edu.cn
Received: April 7 2021; Revised: May 18 2021; Accepted: June 2 2021; Published Online: July 2 2021
Cite this paper:
Xiao’en Shi, Xu Zhang, Xinlu Zhang, Haizhen Guo and Sheng Wang. The Integration of Reactive Oxygen Species Generation and Prodrug Activation for Cancer Therapy. BIO Integration 2022; 3(1): 32–40.
DOI: 10.15212/bioi-2021-0011. Available at: https://bio-integration.org/
Download citation
© 2022 The Authors. This is an open access article distributed under the terms of the Creative Commons Attribution License (https://creativecommons.org/licenses/by/4.0/). See https://bio-integration.org/copyright-and-permissions/
Abstract
The combination of chemotherapeutic drugs and reactive oxygen species (ROS) can improve cancer treatment outcome. Many ROS-generation strategies can specifically consume tumor-inherent oxygen and generate ROS, resulting in amplified ROS level and aggravated hypoxia. Therefore, the ROS generation strategy can integrate with prodrug activation strategy to realize synergetic therapy. In recent years, stimuli-responsive nanomedicines have been developed to realize the integration of ROS generation and prodrug activation. Triggered by a stimulus, nanomedicines can generate ROS at the tumor site, which can further activate the release of active drugs. In this review, we will summarize the latest progress of these nanomedicines and discuss the perspectives and challenges.
Keywords
Cancer therapy, hypoxia, nanomedicine, prodrug, reactive oxygen species.
Introduction
Chemotherapy, a cancer treatment approach based on small-molecule chemotherapeutic drugs, has been widely used in the clinic [1–3]. By systemic administration of drugs, the proliferation of tumor cells can be inhibited. However, serious side effects may also be caused by chemotherapy because chemotherapeutic drugs can cause damage to both tumor cells and normal ones [4–7]. Prodrugs, which refer to a class of bioreversible drug derivatives, have attracted much attention [8]. Currently, approximately 10% of the marketed chemotherapeutic drugs worldwide are in the form of prodrugs [9]. Prodrugs do not show high pharmacological activity until they are activated; therefore, the development of prodrugs is an efficient strategy to improve the physicochemical, biopharmaceutical, or pharmacokinetic properties of drugs, overcoming drawbacks of parent drugs [10, 11].
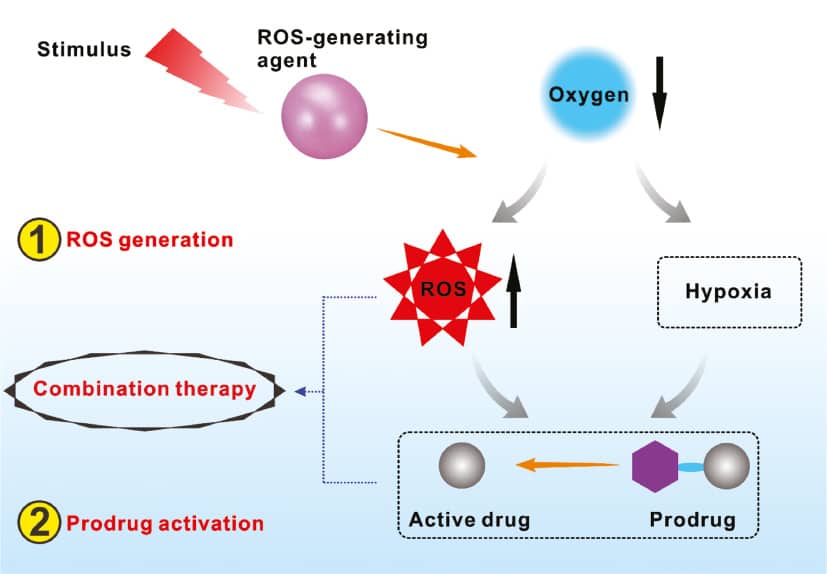
In the past several decades, a variety of prodrugs that can be activated by in vivo stimuli such as pH, glutathione (GSH), and enzymes, have been developed (Table 1) [12–18], and some of which are already in clinical trial [19]. However, acidic condition and GSH are also presented in normal cells; therefore, the selectivity of commonly used pH- and GSH-responsive prodrugs is limited because these prodrugs can be partially activated by intracellular environments of normal cells. To improve the tumor selectivity of prodrug activation, various reactive oxygen species (ROS)–activated prodrugs based on ROS-sensitive bonds, such as thioketal bond and peroxalate ester, have been developed [20–26]. By exploiting nanotechnology, the ROS-responsive prodrugs and tumor-specific ROS-generating agents such as photosensitizers can be integrated into one nanomedicine. Through passive targeting, the nanomedicine will accumulate in tumor tissue. In response to certain stimulus, the nanomedicine will first generate ROS, which will further trigger the activation of ROS-responsive prodrugs, achieving chemo/ROS combination therapy. In addition, most of the ROS generation processes will consume inherent oxygen, resulting in exacerbation of tumor hypoxic environment [27–29]. Therefore, the integration of ROS-generating agents and hypoxia-activated prodrugs is also a promising approach to realize tumor-specific combination therapy (Figure 1). The hypoxia-responsive prodrugs consist based prodrug or polyprodrug; the other is the drug whose pharmacological activity can be activated in hypoxic environment, such as tirapazamine (TPZ) and 1,4-bis([2-(dimethylamino-N-oxide)ethyl]amino)5,8-dihydroxy-anthracene-9,10-dione) [30–32].
Table 1 Summary of Stimuli-Activatable Prodrugs in Cancer Therapy
| Stimuli | Responsive Groups | Active Drugs | References |
|---|---|---|---|
| pH | Hydrazone bond | DOX | [62–65] |
| Ketal linkage | Etoposide | [66] | |
| GSH | Disulfide bond | CPT | [12–14, 18] |
| DOX | [67] | ||
| PTX | [68, 69] | ||
| Diselenium bond | Docetaxel | [70] | |
| ROS | Thioether bond | PTX | [41] |
| Thioketal linker | DOX | [38, 39, 46] | |
| CPT | [25, 26, 37, 42, 50] | ||
| PTX | [23] | ||
| Cabazitaxel | [71] | ||
| Mitoxantrone | [33] | ||
| SS31 | [72] | ||
| Peroxalate ester linkage | CPT | [21, 49] | |
| Phenylboronic ester | DOX | [45] | |
| PTX | [73] | ||
| Enzyme | Ester bond | Mitoxantrone | [74] |
| 7-Ethyl-10-hydroxycamptothecin | [75, 76] | ||
| DOX | [77] | ||
| Hypoxia | TPZ | TPZ radical | [56–60, 78, 79] |
| AQ4N | AQ4 | [32, 80, 81] | |
| Azobenzene linker | PTX | [54] | |
| Nitro groups | IPM-Br | [55] | |
| Hydrogen sulfide | Sulfoxide linker | DOX | [82] |
| Thermo | Edman linker | DOX | [83] |
| Azo bond | DOX | [84] |
Figure 1 Schematic illustration of the integration of ROS generation and prodrug activation.
This review summarizes recent advances in the cancer therapeutic strategy combining ROS generation and prodrug activation. The representative nanomedicines and their applications in cancer therapy will be introduced. Finally, the perspectives and challenges of this therapeutic strategy will also be discussed.
ROS-triggered prodrug activation
By conjugating drug molecules with other small molecules or polymers through ROS-sensitive linkers, ROS-responsive prodrugs can be obtained [33]. In the presence of high levels of ROS, these prodrugs can be activated to release active drugs. Compared with normal tissue, cancer cells show higher level of ROS; however, the endogenous ROS is still insufficient to realize effective prodrug activation. In the past decades, various ROS generation approaches have been used to further increase the ROS level inside cancer and thus improve the responsivity of ROS-responsive prodrugs.
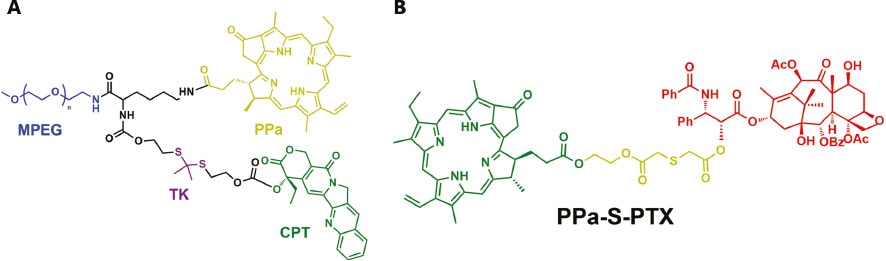
Among the ROS generation approaches, photodynamic therapy (PDT) is the most commonly used one [34–36]. Qian et al. reported a ROS-responsive nanomedicine self-assembled from amphiphilic prodrug for combined local-regional PDT and chemotherapy [37]. To prepare the amphiphilic prodrug, a photosensitizer pyropheophorbide-a (PPa) and a chemotherapeutic drug camptothecin (CPT) were conjugated to poly(ethylene glycol) (PEG) simultaneously (Figure 2A). In blood circulation, both CPT and PPa are inactive, resulting in reduced side effects to the healthy tissues. Upon laser irradiation, singlet oxygen will be first produced via PPa-mediated photodynamic process. Furthermore, the ROS will cleave the thioketal linker and thus lead to on-demand CPT release. Therefore, this nanomedicine can be used for combination of PDT and chemotherapy. Li et al. developed a ROS-activatable prodrug vesicle composed of unsaturated phospholipids, phospholipid-mimic doxorubicin (DOX) prodrug and PEG-modified PPa [38]. Under imaging-guided laser irradiation, ROS-mediated oxidation of unsaturated phospholipids and cleavage of thioketal linkers will lead to increased permeability of vesicle and DOX prodrug activation, allowing ultrafast DOX release. In another study, Wang’s group developed a polyphosphoester-DOX conjugate-based polyprodrug nanoparticle (NP), in which the photosensitizer Ce6 was encapsulated [39]. This polyprodrug NP can achieve photo-triggered dissociation and prodrug activation. In a recent study, Wang et al. reported a ROS-responsive drug delivery nanosystem [26]. A thioketal linker-containing poly-CPT prodrug was modified to iron oxide nanoparticles (IONPs). Then the polyprodrug-modified IONPs and aggregation-induced emission (AIE) photosensitizer were encapsulated into a nanomicelle formed by pH-responsive amphiphilic polymer. Under white light irradiation, the singlet oxygen produced by AIE photosensitizer will cause CPT release. Moreover, due to the pH/ROS dual responsiveness, the nanomedicine can achieve two-stage size changes for enhanced drug delivery and fast elimination.
Figure 2 (A) Chemical structure of MPEG-(TK-CPT)-PPa. (B) Chemical structure of PPa-S-PTX dimer.
The design of ROS-responsive heterotypic drug-photosensitizer dimer represents another strategy to realize ROS-triggered prodrug activation [40]. Recently, Sun and colleagues reported a nanomedicine that which is based on a ROS-responsive dimer [41]. The dimer was prepared by conjugating paclitaxel (PTX) with PPa via a ROS-cleavable single thioether linker (Figure 2B). With the help of PEG-lipid, the dimer can self-assemble into PEGylated prodrug (PSP) NPs with ultrahigh loading capacity. Once the PSP NPs arrive on the tumor sites via the passive targeting effect, the endogenous ROS will lead to partial release of PPa and PTX through cleavage of thioether bond. The disassembly of PSP NPs will address the aggregation-caused quenching (ACQ) effect of PPa. Therefore, the ROS generation efficiency in light-triggered PDT process will be significantly improved. This self-facilitated ROS generation further triggered prodrug activation, resulting in dual-synergistic multimodal cancer therapy. In a recent study, Chen’s group prepared a heterotypic dimer containing CPT and 2-(1-hexyloxyethyl)-2-devinyl pyropheophorbide-a (HPPH) [42]. The chemodrug and photosensitizer were linked by a cleavable thioketal linker. The dimer-loaded NPs showed high drug loading content without serious drug leakage. Under endogenous ROS and the ROS generated in PDT process, the HRC prodrug can be activated to achieve synergistic tumor inhibition.
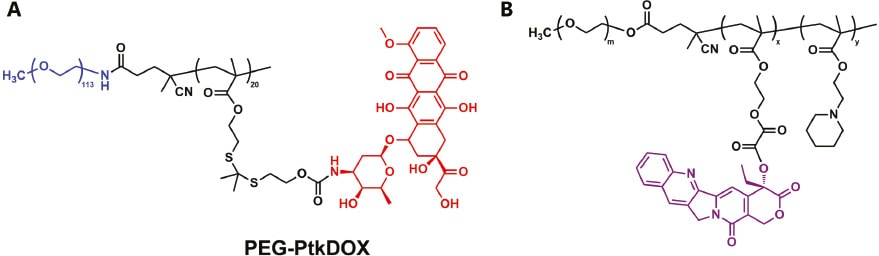
Besides PDT, ROS can also be generated by chemical methods [43, 44]. For example, β-lapachone (Lap) can generate hydrogen peroxide through the catalysis of the nicotinamide adenine dinucleotide (phosphate) (NAD(P)H): quinone oxidoreductase 1 (NQO1) enzyme. Due to NQO1 overexpression of tumor cells, Lap-based nanomedicine exhibits an extremely high selectivity. Rao and colleagues reported a nanomedicine by co-loading Lap and a ROS-responsive prodrug (BDOX) in a nanomicelle [45]. Once the nanomedicines enter NQO1-overexpressed cancer cells, they will first release Lap for improving the intracellular hydrogen peroxide level. Then the BDOX prodrug will be activated by hydrogen peroxide to release free DOX. More importantly, the sequential drug release process allows the synergy of Lap and DOX to prevent drug efflux, resulting in reversal of multidrug resistance of cancer cells. The cytotoxicities of nanomedicines against NQO1-overexpressing cancer cells (4T1, MCF-7, and MCF-7 ADR) were higher than that against normal cells (NIH/3T3). Based on the characteristic of Lap, Chen et al. developed a pH/ROS dual-responsive iron-containing nanomedicine (Figure 3A) [46]. In this nanomedicine, Lap was encapsulated into polymeric micelles that assembled from a pH-responsive polymer, a ROS-responsive DOX-based polyprodrug. In intracellular acidic environment, Lap will be first released due to pH-triggered disassembly of the nanomedicine. Through iron-catalyzed Fenton reaction, the hydrogen peroxide produced by Lap will be transformed to hydroxyl radicals, which further cleave the thioketal linker between DOX and polyprodrug to release active DOX. Therefore, chemo/chemodynamic combination therapy was achieved by the cascade of hydroxyl radical generation and DOX release. Glucose oxidase (GOD), an enzyme that can convert oxygen and glucose into hydrogen peroxide and glucose acid, is also widely used to develop multifunctional nanomedicine [47, 48]. Ge’s group has developed a series of GOD-based nanosystems for prodrug activation [49, 50]. For example, a GOD-encapsulated nanoreactor self-assembled from amphiphilic polyprodrug was prepared for oxidation/chemotherapy (Figure 3B) [49]. In acidic tumor environment, due to the permeability change of the nanoreactor membranes, glucose can diffuse into the nanoreactor and generate hydrogen peroxide under the catalysis of GOD. The high level of hydrogen peroxide will further trigger the cleavage of oxalate bonds and activate the polyprodrug, releasing active CPT. Therefore, this nanoreactor combines oxidation therapy and chemotherapy to inhibit tumor growth.
Figure 3 (A) Chemical structure of PEG-PtkDOX. (B) Chemical structure of ROS-responsive polyprodrug.
Hypoxia-triggered prodrug activation
In most solid tumors, hypoxia is a typical characteristic [51, 52]. Some ROS generation strategies, such as type II PDT and GOD-mediated catalytic process, need to further consume tumor oxygen to produce singlet oxygen or hydrogen peroxide [53]. The exacerbated hypoxia of tumor environment can also be used as a stimulus to activate hypoxia-responsive nanomedicines. Therefore, the combination of ROS-generating agents and hypoxia-activatable prodrugs is a promising approach to achieve enhanced cancer therapy.
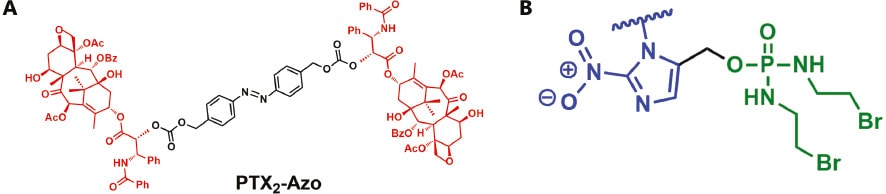
One type of hypoxia-activatable prodrug is one that contains hypoxia-sensitive linkers. Xie et al. developed a hypoxia-activated self-immolative PTX dimer (PTX2-Azo) by conjugating two PTX molecules through an azobenzene (Azo) linker (Figure 4A) [54]. The PTX2-Azo was encapsulated in the NP self-assembled from chlorin e6 (Ce6)-containing amphiphilic copolymer, obtaining Ce6/PTX2-Azo NP. Attributing to the passive targeting effect, the Ce6/PTX2-Azo NP with a size of approximately 100 nm can effectively accumulate in tumor tissue. Upon laser irradiation, the encapsulated photosensitizer Ce6 will consume inherent oxygen and generate singlet oxygen to induce cell apoptosis. Due to the PDT-aggravated hypoxia, the Azo linker of PTX2-Azo prodrug will be cleaved by reductases. Then the active PTX will be released through a cascade elimination reaction. Through the combination of PDT and prodrug activation, excellent antitumor efficacy can be achieved.
Figure 4 (A) Chemical structure of PTX2-Azo. (B) Chemical structure of hypoxia-responsive prodrug.
In another study, Pu’s group reported a nanoprodrug (denoted as SPNpd) for PDT and hypoxia-activated drug release [55]. The SPNpd was self-assembled from a drug-conjugated amphiphilic semiconducting polymer. Bromoisophosphoramide mustard intermediate (IPM-Br), a chemotherapeutic drug, was conjugated to the SPNpd by using a hypoxia-cleavable linker (Figure 4B). In this system, the light-responsive semiconducting polymer was used as a photosensitizer, which can produce ROS under 808-nm light irradiation. Meanwhile, with the consumption of oxygen, the hypoxia of tumor exacerbated. In such a hypoxic condition, the linker between IPM-Br and the polymer will be cleaved by nitroreductase-catalyzed reduction, resulting in hypoxia-activated IPM-Br release. The activity will further induce DNA crosslinking and subsequent cellular apoptosis. Therefore, the SPNpd can realize synergistic photodynamic/chemotherapy and effective inhibition of tumor growth.
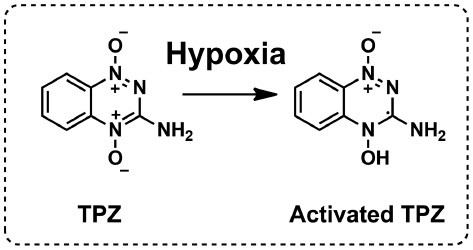
Another type of hypoxia-activatable prodrug mainly contains quinone-based prodrugs and N-oxide prodrugs that show little toxicity in normoxic condition and high toxicity in hypoxic condition. Among the prodrugs, TPZ is a widely studied one. In hypoxic condition, TPZ can be converted into toxic radicals through bioreduction (Figure 5) [56]. Therefore, the development of hybrid nanosystems that combine TPZ and photosensitizer represents a promising way to realize combination therapy. Porphyrinic metal-organic framework (MOF), which self-assembled from metal ion and porphyrin photosensitizer through coordination interactions, has attracted much attention. Porphyrinic MOF can be used not only as a nanophotosensitizer for PDT, but also as a nanocarrier for delivering other therapeutic agents. Li et al. reported a TPZ-loaded core−shell upconversion nanoparticle in porphyrinic MOFs (TPZ/UCSs) for combination therapy [57]. Under near-infrared (NIR) light irradiation, the upconversion nanoparticle core will convert the NIR light to visible light to activate photosensitizer in MOF shell, generating 1O2 efficiently. Furthermore, PDT-aggravated tumor hypoxia will activate the pharmacological activity of encapsulated TPZ, enabling combinational photodynamic/chemotherapy. This study provides a promising nanoplatform in fighting tumor through the integration of NIR-triggered ROS generation and hypoxia-triggered prodrug activation.
Figure 5 Chemical structures of TPZ and activated TPZ.
The hypoxia-responsive prodrugs have also been combined with GOD to develop nanomedicine [58, 59]. Wu et al. constructed a hybrid nanoreactor (denoted as HGTFT) composed of human serum albumin (HSA), GOD, TPZ, Fe3+ and tannic acid (TA) for cascade chemo-chemodynamic therapy [60]. In cancer cells, GOD will first consume glucose and oxygen for starvation therapy, resulting in the production of hydrogen peroxide and aggravated hypoxia. Through TA-accelerated Fenton reaction, the hydrogen peroxide will react with iron ions to produce highly toxic hydroxyl radicals for chemodynamic therapy. Meanwhile, the hypoxic environment will activate TPZ to generate BTZ• for chemotherapy. The in vitro and in vivo results demonstrated excellent biosafety and enhanced anticancer activity of the HGTFT nanoreactor. Therefore, this nanoreactor has great potential for clinical applications.
Cascade of prodrug release and activation
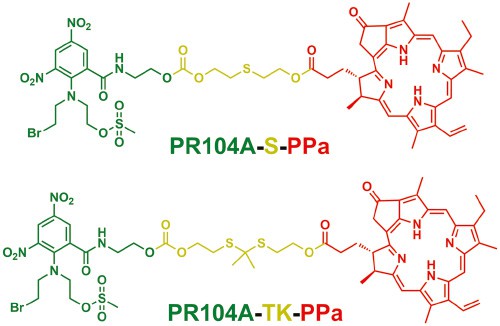
As we discussed above, the PDT process will lead to two consequences, high ROS level and aggravated hypoxia, both of which can be used for drug release and prodrug activation. In order to make full use of these two consequences, Sun and colleagues developed a nanomedicine that combines ROS-triggered prodrug release and hypoxia-triggered prodrug activation [61]. As shown in Figure 6, two types of heterodimeric dimers that based on hypoxia-responsive prodrug PR104A and photosensitizer PPa were synthesized. The PR104A and PPa were conjugated via a ROS-sensitive thioether or thioketal linkage. Then the heterodimeric dimers self-assembled to form prodrug-NPs with a dense intermolecular-packing structure. Under laser irradiation, the thioether or thioketal linkages between PPa and PR104A will be cleaved because electrons can be transferred from PPa to the sulfur atoms via photoinduced electron transfer. Therefore, the PR104A prodrug will be released, causing disassembly of prodrug-NPs. As the ACQ effect was relieved, the PPa will efficiently consume oxygen and produce singlet oxygen to further promote the PR104A release. Meanwhile, the hypoxic condition caused by oxygen consumption will facilitate the activation of hypoxia-sensitive PR104A to realize DNA damage.
Figure 6 Chemical structures of PR104A-S-PPa and PR104A-TK-PPa.
Conclusion and outlook
Compared with normal tissue, tumor tissue has unique structural and metabolic characteristics, such as weak acidic microenvironment, hypoxia condition, high ROS level, and overexpression of specific enzymes. Based on these special characteristics, prodrugs that can be activated in tumor site exhibit great potential in antitumor therapy. With the developments of stimuli-sensitive moieties, various prodrug and polyprodrug systems have been designed and applied in cancer treatments. However, the selectivity of generally used pH- and GSH-activated prodrugs is still limited. Many ROS generation strategies, such as PDT, can specifically consume tumor inherent oxygen and generate ROS, resulting in amplified ROS level and aggravated hypoxia. In recent years, nanomedicines that integrate ROS generation strategies with ROS- or hypoxia-responsive prodrugs have been developed. Upon accumulation in tumor tissue, the nanomedicines will first generate ROS in tumor site, which can not only cause cell death directly, but also activate prodrugs to improve therapeutic efficiency. Therefore, these nanomedicines show great potential to realize combination therapy with improved selectivity.
In this review, we summarized recent advances of the integration strategy. Although significant progress has been made in the design and application of ROS-responsive and hypoxia-responsive prodrugs, there are still some obstacles and challenges. For example, the efficiency of the first stage (ROS generation) will significantly affect the effectiveness of second stage (prodrug activation). Particularly, this strategy is difficult to apply to the treatment of hypoxic tumors. Furthermore, in some systems, the prodrug activation process needs to consume ROS, resulting in unsatisfactory combination treatment outcome. Therefore, for the future research, more efforts should be put toward to address these issues. In addition, ROS generation can also be triggered by engineered bacteria, which provided an opportunity for interdisciplinary integration.
Conflict of interest
The authors declare no conflict of interest.
Acknowledgements
This work was supported by the National Natural Science Foundation of China (32000991), the Young Elite Scientists Sponsorship Program by Tianjin (TJSQNTJ-2020-02), and Tianjin Research Innovation Project for Postgraduate Students (2020YJSB130).
References
- Yoo J-W, Irvine DJ, Discher DE, Mitragotri S. Bio-inspired, bioengineered and biomimetic drug delivery carriers. Nat Rev Drug Discovery 2011;10:521-35. [PMID: 21720407 DOI: 10.1038/nrd3499]
- Jain RK, Stylianopoulos T. Delivering nanomedicine to solid tumors. Nat Rev Clin Oncol 2010;7:653-64. [PMID: 20838415 DOI: 10.1038/nrclinonc.2010.139]
- Zhang X, Wang S, Cheng G, Yu P, Chang J, et al . Cascade drug-release strategy for enhanced anticancer therapy. Matter 2021;4:26-53. [PMID: 33718863 DOI: 10.1016/j.matt.2020.10.002]
- Cheng Z, Al Zaki A, Hui JZ, Muzykantov VR, Tsourkas A. Multifunctional nanoparticles: cost versus benefit of adding targeting and imaging capabilities. Science 2012;338:903-10. [PMID: 23161990 DOI: 10.1126/science.1226338]
- Peer D, Karp JM, Hong S, Farokhzad OC, Margalit R, et al . Nanocarriers as an emerging platform for cancer therapy. Nat Nanotechnol 2007;2:751-60. [PMID: 18654426 DOI: 10.1038/nnano.2007.387]
- Thakor AS, Gambhir SS. Nanooncology: the future of cancer diagnosis and therapy. Ca-Cancer J Clin 2013;63:395-418. [PMID: 24114523 DOI: 10.3322/caac.21199]
- Wang S, Huang P, Chen X. Hierarchical targeting strategy for enhanced tumor tissue accumulation/retention and cellular internalization. Adv Mater 2016;28:7340-64. [PMID: 27255214 DOI: 10.1002/adma.201601498]
- Rautio J, Kumpulainen H, Heimbach T, Oliyai R, Oh D, et al. Prodrugs: design and clinical applications. Nat Rev Drug Discovery 2008;7:255-70. [PMID: 18219308 DOI: 10.1038/nrd2468]
- Rautio J, Meanwell NA, Di L, Hageman MJ. The expanding role of prodrugs in contemporary drug design and development. Nat Rev Drug Discovery 2018;17:559-87. [PMID: 29700501 DOI: 10.1038/nrd.2018.46]
- Stella VJ, Nti-Addae KW. Prodrug strategies to overcome poor water solubility. Adv Drug Delivery Rev 2007;59:677-94. [PMID: 17628203 DOI: 10.1016/j.addr.2007.05.013]
- Pradere U, Garnier-Amblard EC, Coats SJ, Amblard F, Schinazi RF. Synthesis of nucleoside phosphate and phosphonate prodrugs. Chem Rev 2014;114:9154-218. [PMID: 25144792 DOI: 10.1021/cr5002035]
- Wang S, Yu G, Wang Z, Jacobson O, Tian R, et al. Hierarchical tumor microenvironment-responsive nanomedicine for programmed delivery of chemotherapeutics. Adv Mater 2018;30:1803926. [PMID: 30168612 DOI: 10.1002/adma.201803926]
- Zhang F, Zhu G, Jacobson O, Liu Y, Chen K, et al. Transformative nanomedicine of an amphiphilic camptothecin prodrug for long circulation and high tumor uptake in cancer therapy. ACS Nano 2017;11:8838-48. [PMID: 28858467 DOI: 10.1021/acsnano.7b03003]
- Zhang F, Ni Q, Jacobson O, Cheng S, Liao A, et al. Polymeric nanoparticles with a glutathione-sensitive heterodimeric multifunctional prodrug for in vivo drug monitoring and synergistic cancer therapy. Angew Chem Int Ed 2018;57:7066-70. [PMID: 29624828 DOI: 10.1002/anie.201801984]
- Yu G, Zhang M, Saha ML, Mao Z, Chen J, et al. Antitumor activity of a unique polymer that incorporates a fluorescent self-assembled metallacycle. J Am Chem Soc 2017;139:15940-9. [PMID: 29019660 DOI: 10.1021/jacs.7b09224]
- Hu X, Zhai S, Liu G, Xing D, Liang H, et al . Concurrent drug unplugging and permeabilization of polyprodrug-gated crosslinked vesicles for cancer combination chemotherapy. Adv Mater 2018;30:1706307. [PMID: 29635863 DOI: 10.1002/adma.201706307]
- Guo X, Wang L, Duval K, Fan J, Zhou S, et al . Dimeric drug polymeric micelles with acid-active tumor targeting and FRET-traceable drug release. Adv Mater 2018;30:1705436. [PMID: 29210480 DOI: 10.1002/adma.201705436]
- Wang S, Zhang F, Yu G, Wang Z, Jacobson O, et al. Zwitterionic-to-cationic charge conversion polyprodrug nanomedicine for enhanced drug delivery. Theranostics 2020;10:6629-37. [PMID: 32550894 DOI: 10.7150/thno.47849]
- Xie A, Hanif S, Ouyang J, Tang ZM, Kong N, et al. Stimuli -responsive prodrug-based cancer nanomedicine. EBioMedicine 2020;56:102821. [PMID: 32505922 DOI: 10.1016/j.ebiom.2020.102821]
- Yuan Y, Liu J, Liu B. Conjugated-polyelectrolyte-based polyprodrug: targeted and image-guided photodynamic and chemotherapy with on-demand drug release upon irradiation with a single light source. Angew Chem Int Ed 2014;53:7163-8. [PMID: 24861823 DOI: 10.1002/anie.201402189]
- Wang S, Wang Z, Yu G, Zhou Z, Jacobson O, et al. Tumor-specific drug release and reactive oxygen species generation for cancer chemo/chemodynamic combination therapy. Adv Sci 2019;6:1801986. [PMID: 30886808 DOI: 10.1002/advs.201801986]
- Li J, Ke W, Wang L, Huang M, Yin W, et al. Self-sufficing H2O2-responsive nanocarriers through tumor-specific H2O2 production for synergistic oxidation-chemotherapy. J Control Release 2016;225:64-74. [PMID: 26806789 DOI: 10.1016/j.jconrel.2016.01.029]
- Pei Q, Hu X, Zheng X, Liu S, Li Y, et al. Light-activatable red blood cell membrane-camouflaged dimeric prodrug nanoparticles for synergistic photodynamic/chemotherapy. ACS Nano 2018;12:1630-41. [PMID: 29346736 DOI: 10.1021/acsnano.7b08219]
- Yue C, Yang Y, Zhang C, Alfranca G, Cheng S, et al. Ros-responsive mitochondria-targeting blended nanoparticles: chemo- and photodynamic synergistic therapy for lung cancer with on-demand drug release upon irradiation with a single light source. Theranostics 2016;6:2352-66. [PMID: 27877240 DOI: 10.7150/thno.15433]
- Zhang W, Hu X, Shen Q, Xing D. Mitochondria-specific drug release and reactive oxygen species burst induced by polyprodrug nanoreactors can enhance chemotherapy. Nat Commun 2019;10:1704. [PMID: 30979885 DOI: 10.1038/s41467-019-09566-3]
- Cheng G, Zong W, Guo H, Li F, Zhang X, et al. Programmed size-changeable nanotheranostic agents for enhanced imaging guided chemo/photodynamic combination therapy and fast elimination. Adv Mater 2021;33:2100398. [PMID: 33876500 DOI: 10.1002/adma.202100398]
- Liu JN, Bu WB, Shi JL. Chemical design and synthesis of functionalized probes for imaging and treating tumor hypoxia. Chem Rev 2017;117:6160-224. [PMID: 28426202 DOI: 10.1021/acs.chemrev.6b00525]
- Wang S, Tian R, Zhang X, Cheng G, Yu P, et al. Beyond photo: Xdynamic therapies in fighting cancer. Adv Mater 2021;33:2007488. [PMID: 33987898 DOI: 10.1002/adma.202007488]
- Wang S, Yu G, Yang W, Wang Z, Jacobson O, et al. Photodynamic-chemodynamic cascade reactions for efficient drug delivery and enhanced combination therapy. Adv Sci 2021;8:2002927. [PMID: 34026433 DOI: 10.1002/advs.202002927]
- Lin QN, Bao CY, Yang YL, Liang QN, Zhang DS, et al. Highly discriminating photorelease of anticancer drugs based on hypoxia activatable phototrigger conjugated chitosan nanoparticles. Adv Mater 2013;25:1981-6. [PMID: 23401259 DOI: 10.1002/adma.201204455]
- Sharma A, Arambula JF, Koo S, Kumar R, Singh H, et al. Hypoxia-targeted drug delivery. Chem Soc Rev 2019;48:771-813. [PMID: 30575832 DOI: 10.1039/c8cs00304a]
- He ZM, Dai YL, Li XL, Guo D, Liu YJ, et al. Hybrid nanomedicine fabricated from photosensitizer-terminated metal-organic framework nanoparticles for photodynamic therapy and hypoxia-activated cascade chemotherapy. Small 2019;15:1804131. [PMID: 30565431 DOI: 10.1002/smll.201804131]
- Xu X, Saw PE, Tao W, Li Y, Ji X, et al. Ros-responsive polyprodrug nanoparticles for triggered drug delivery and effective cancer therapy. Adv Mater 2017;29:1700141. [PMID: 28681981 DOI: 10.1002/adma.201700141]
- Lucky SS, Soo KC, Zhang Y. Nanoparticles in photodynamic therapy. Chem Rev 2015;115:1990-2042. [DOI: https://doi.org/10.1021/cr5004198??]
- Yu G, Cen T-Y, He Z, Wang S-P, Wang Z, et al. Porphyrin nanocage-embedded single molecular nanoparticles for cancer nanotheranostics. Angew Chem Int Ed 2019;58:8799-803. [PMID: 31034679 DOI: 10.1002/anie.201903277]
- Cheng L, Wang C, Feng L, Yang K, Liu Z. Functional nanomaterials for phototherapies of cancer. Chem Rev 2014;114:10869-939. [PMID: 25260098 DOI: 10.1021/cr400532z]
- Chu BY, Qu Y, He XL, Hao Y, Yang CL, et al. ROS-responsive camptothecin prodrug nanoparticles for on-demand drug release and combination of chemotherapy and photodynamic therapy. Adv Funct Mater 2020;30:2005918. [DOI: https://doi.org/10.1002/adfm.202005918??]
- Zhou F, Feng B, Wang T, Wang D, Cui Z, et al. Theranostic prodrug vesicles for reactive oxygen species-triggered ultrafast drug release and local-regional therapy of metastatic triple-negative breast cancer. Adv Funct Mater 2017;27:1703674. [DOI: https://doi.org/10.1002/adfm.201703674??]
- Pei P, Sun C, Tao W, Li J, Yang X, et al . ROS-sensitive thioketal-linked polyphosphoester-doxorubicin conjugate for precise phototriggered locoregional chemotherapy. Biomaterials 2019;188:74-82. [PMID: 30336287 DOI: 10.1016/j.biomaterials.2018.10.010]
- Liu LH, Qiu WX, Li B, Zhang C, Sun LF, et al. A red light activatable multifunctional prodrug for image-guided photodynamic therapy and cascaded chemotherapy. Adv Funct Mater 2016;26:6257-69. [DOI: https://doi.org/10.1002/adfm.201602541??]
- Luo C, Sun BJ, Wang C, Zhang XB, Chen Y, et al. Self-facilitated ros-responsive nanoassembly of heterotypic dimer for synergistic chemo-photodynamic therapy. J Control Release 2019;302:79-89. [PMID: 30946853 DOI: 10.1016/j.jconrel.2019.04.001]
- Jiang M, Mu J, Jacobson O, Wang Z, He L, et al. Reactive oxygen species activatable heterodimeric prodrug as tumor-selective nanotheranostics. ACS Nano 2020;14:16875-86. [DOI: https://doi.org/10.1021/acsnano.0c05722??]
- Lin L-S, Huang T, Song J, Ou X-Y, Wang Z, et al. Synthesis of copper peroxide nanodots for H2O2 self-supplying chemodynamic therapy. J Am Chem Soc 2019;141:9937-45. [PMID: 31199131 DOI: 10.1021/jacs.9b03457]
- Lin L, Wang S, Deng H, Yang W, Rao L, et al. Endogenous labile iron pool-mediated free radical generation for cancer chemodynamic therapy. J Am Chem Soc 2020;142:15320-30. [PMID: 32820914 DOI: 10.1021/jacs.0c05604]
- Ye M, Han Y, Tang J, Piao Y, Liu X, et al. A tumor-specific cascade amplification drug release nanoparticle for overcoming multidrug resistance in cancers. Adv Mater 2017;29:1702342. [PMID: 28833669 DOI: 10.1002/adma.201702342]
- Wang S, Yu G, Wang Z, Jacobson O, Lin LS, et al. Enhanced antitumor efficacy by a cascade of reactive oxygen species generation and drug release. Angew Chem Int Ed 2019;58:14758-63. [PMID: 31429173 DOI: 10.1002/anie.201908997]
- Feng L, Xie R, Wang C, Gai S, He F, et al. Magnetic targeting, tumor microenvironment-responsive intelligent nanocatalysts for enhanced tumor ablation. ACS Nano 2018;12:11000-12. [PMID: 30339353 DOI: 10.1021/acsnano.8b05042]
- Fan W, Lu N, Huang P, Liu Y, Yang Z, et al. Glucose-responsive sequential generation of hydrogen peroxide and nitric oxide for synergistic cancer starving-like/gas therapy. Angew Chem Int Ed 2017;56:1229-33. [PMID: 27936311 DOI: 10.1002/anie.201610682]
- Li J, Li Y, Wang Y, Ke W, Chen W, et al. Polymer prodrug-based nanoreactors activated by tumor acidity for orchestrated oxidation/chemotherapy. Nano Lett 2017;17:6983-90. [PMID: 28977746 DOI: 10.1021/acs.nanolett.7b03531]
- Ke W, Li J, Mohammed F, Wang Y, Tou K, et al. Therapeutic polymersome nanoreactors with tumor-specific activable cascade reactions for cooperative cancer therapy. ACS Nano 2019;13:2357-69. [PMID: 30699292 DOI: 10.1021/acsnano.8b09082]
- Zhu H, Li Q, Shi B, Ge F, Liu Y, et al. Dual-emissive platinum(II) metallacage with a sensitive oxygen response for imaging of hypoxia and imaging-guided chemotherapy. Angew Chem Int Ed 2020;59:20208-14. [PMID: 32710650 DOI: 10.1002/anie.202009442]
- He Z, Huang X, Wang C, Li X, Liu Y, et al. A catalase-like metal-organic framework nanohybrid for O2-evolving synergistic chemoradiotherapy. Angew Chem Int Ed 2019;58:8752-6. [PMID: 31046176 DOI: 10.1002/anie.201902612]
- Yu P, Li X, Cheng G, Zhang X, Wu D, et al. Hydrogen peroxide-generating nanomedicine for enhanced chemodynamic therapy. Chin Chem Lett 2021. [DOI: 10.1016/j.cclet.2021.02.015]
- Zhou SY, Hu XL, Xia R, Liu S, Pei Q, et al. A paclitaxel prodrug activatable by irradiation in a hypoxic microenvironment. Angew Chem Int Ed 2020;59:23198-205. [PMID: 32852145 DOI: 10.1002/anie.202008732]
- Cui D, Huang J, Zhen X, Li J, Jiang Y, et al. A semiconducting polymer nano-prodrug for hypoxia-activated photodynamic cancer therapy. Angew Chem Int Ed 2019;58:5920-4. [DOI: 10.1002/anie.201814730]
- Qian C, Feng P, Yu J, Chen Y, Hu Q, et al. Anaerobe-inspired anticancer nanovesicles. Angew Chem Int Ed 2017;56:2588-93. [PMID: 28140504 DOI: 10.1002/anie.201611783]
- Shao YL, Liu B, Di ZH, Zhang G, Sun LD, et al. Engineering of upconverted metal-organic frameworks for near-infrared light-triggered combinational photodynamic/chemo-/immunotherapy against hypoxic tumors. J Am Chem Soc 2020;142:3939-46. [PMID: 31968933 DOI: 10.1021/jacs.9b12788]
- Zhang L, Wang ZZ, Zhang Y, Cao FF, Dong K, et al. Erythrocyte membrane cloaked metal-organic framework nanoparticle as biomimetic nanoreactor for starvation-activated colon cancer therapy. ACS Nano 2018;12:10201-11. [PMID: 30265804 DOI: 10.1021/acsnano.8b05200]
- Zhang MK, Li CX, Wang SB, Liu T, Song XL, et al. Tumor starvation induced spatiotemporal control over chemotherapy for synergistic therapy. Small 2018;14:1803602. [PMID: 30370690 DOI: 10.1002/smll.201803602]
- Guo YX, Jia HR, Zhang XD, Zhang XP, Sun Q, et al. A glucose/oxygen-exhausting nanoreactor for starvation- and hypoxia-activated sustainable and cascade chemo-chemodynamic therapy. Small 2020;16:2000897. [PMID: 32537936 DOI: 10.1002/smll.202000897]
- Zhao DY, Tao WH, Li SH, Li LX, Sun YX, et al. Light-triggered dual-modality drug release of self-assembled prodrug-nanoparticles for synergistic photodynamic and hypoxia-activated therapy. Nanoscale Horiz 2020;5:886-94. [PMID: 32219262 DOI: 10.1039/d0nh00034e]
- Bai S, Yang LL, Wang YJ, Zhang T, Fu LQ, et al. Prodrug-based versatile nanomedicine for enhancing cancer immunotherapy by increasing immunogenic cell death. Small 2020;16:2000214. [PMID: 32309900 DOI: 10.1002/smll.202000214]
- Luo L, Xu FS, Peng HL, Luo YH, Tian XH, et al. Stimuli-responsive polymeric prodrug-based nanomedicine delivering nifuroxazide and doxorubicin against primary breast cancer and pulmonary metastasis. J Control Release 2020;318:124-35. [PMID: 31838206 DOI: 10.1016/j.jconrel.2019.12.017]
- Dong YM, Du PC, Pei ML, Liu P. Design, postpolymerization conjugation and self-assembly of a di-block copolymer-based prodrug for tumor intracellular acid-triggered dox release. J Mater Chem B 2019;7:5640-7. [DOI: 10.1039/C9TB01511F]
- Yao MN, Ma XT, Zhang X, Shi LQ, Liu TY, et al. Lectin-mediated pH-sensitive doxorubicin prodrug for pre-targeted chemotherapy of colorectal cancer with enhanced efficacy and reduced side effects. Theranostics 2019;9:747-60. [PMID: 30809306 DOI: 10.7150/thno.29989]
- Yu N, Liu T, Zhang X, Gong NQ, Ji TJ, et al. Dually enzyme- and acid-triggered self-immolative ketal glycoside nanoparticles for effective cancer prodrug monotherapy. Nano Lett 2020;20:5465-72. [PMID: 32573235 DOI: 10.1021/acs.nanolett.0c01973]
- Yang Y, Sun B, Zuo S, Li X, Zhou S, et al. Trisulfide bond-mediated doxorubicin dimeric prodrug nanoassemblies with high drug loading, high self-assembly stability, and high tumor selectivity. Sci Adv 2020;6:eabc1725. [PMID: 33148644 DOI: 10.1126/sciadv.abc1725]
- Guo YY, Zhang J, Ding F, Pan GF, Li J, et al. Stressing the role of DNA as a drug carrier: synthesis of DNA-drug conjugates through grafting chemotherapeutics onto phosphorothioate oligonucleotides. Adv Mater 2019;31:1807533. [PMID: 30847970 DOI: 10.1002/adma.201807533]
- Yi XQ, Hu JJ, Dai J, Lou XD, Zhao ZJ, et al. Self-guiding polymeric prodrug micelles with two aggregation-induced emission photosensitizers for enhanced chemo-photodynamic therapy. ACS Nano 2021;15:3026-37. [PMID: 33449627 DOI: 10.1021/acsnano.0c09407]
- Zuo SY, Sun BJ, Yang YX, Zhou S, Zhang Y, et al. Probing the superiority of diselenium bond on docetaxel dimeric prodrug nanoassemblies: small roles taking big responsibilities. Small 2020;16:e2005039. [PMID: 33078579 DOI: 10.1002/smll.202005039]
- Huang LL, Wan JQ, Wu HH, Chen XN, Bian Q, et al. Quantitative self-assembly of photoactivatable small molecular prodrug cocktails for safe and potent cancer chemo-photodynamic therapy. Nano Today 2021;36:101030. [DOI: 10.1016/j.nantod.2020.101030]
- Liu D, Shu GF, Jin FY, Qi J, Xu XL, et al. ROS-responsive chitosan-SS31 prodrug for AKI therapy via rapid distribution in the kidney and long-term retention in the renal tubule. Sci Adv 2020;6:eabb7422. [PMID: 33036968 DOI: 10.1126/sciadv.abb7422]
- Dong C, Zhou Q, Xiang J, Liu F, Zhou Z, et al. Self-assembly of oxidation-responsive polyethylene glycol-paclitaxel prodrug for cancer chemotherapy. J Control Release 2020;321:529-39. [PMID: 32109513 DOI: 10.1016/j.jconrel.2020.02.038]
- Saw PE, Yao HR, Lin CH, Tao W, Farokhzad OC, et al. Stimuli-responsive polymer-prodrug hybrid nanoplatform for multistage siRNA delivery and combination cancer therapy. Nano Lett 2019;19:5967-74. [PMID: 31381852 DOI: 10.1021/acs.nanolett.9b01660]
- Wang YC, Xie HY, Ying KK, Xie BB, Chen XN, et al. Tuning the efficacy of esterase-activatable prodrug nanoparticles for the treatment of colorectal malignancies. Biomaterials 2021;270:120705. [PMID: 33581609 DOI: 10.1016/j.biomaterials.2021.120705]
- Liu Q, Xie ZJ, Qiu M, Shim I, Yang YL, et al. Prodrug-loaded zirconium carbide nanosheets as a novel biophotonic nanoplatform for effective treatment of cancer. Adv Sci 2020;7:2001191. [DOI: 10.1002/advs.202001191]
- Chung SW, Choi JU, Cho YS, Kim HR, Won TH, et al. Self-triggered apoptosis enzyme prodrug therapy (STAEPT): enhancing targeted therapies via recurrent bystander killing effect by exploiting caspase-cleavable linker. Adv Sci 2018;5:1800368. [PMID: 30027061 DOI: 10.1002/advs.201800368]
- Guo DB, Xu ST, Wang N, Jiang HY, Huang Y, et al. Prodrug-embedded angiogenic vessel-targeting nanoparticle: a positive feedback amplifier in hypoxia-induced chemo-photo therapy. Biomaterials 2017;144:188-98. [PMID: 28837960 DOI: 10.1016/j.biomaterials.2017.08.032]
- Ma YC, Zhao YY, Bejjanki NK, Tang XF, Jiang W, et al. Nanoclustered cascaded enzymes for targeted tumor starvation and deoxygenation-activated chemotherapy without systemic toxicity. ACS Nano 2019;13:8890-902. [PMID: 31291092 DOI: 10.1021/acsnano.9b02466]
- Yang Y, Lu Y, Abbaraju PL, Azimi I, Lei C, et al. Stepwise degradable nanocarriers enabled cascade delivery for synergistic cancer therapy. Adv Funct Mater 2018;28:1800706. [DOI: 10.1002/adfm.201800706]
- Feng L, Cheng L, Dong Z, Tao D, Barnhart TE, et al. Theranostic liposomes with hypoxia activated prodrug to effectively destruct hypoxic tumors post-photodynamic therapy. ACS Nano 2017;11:927-37. [PMID: 28027442 DOI: 10.1021/acsnano.6b07525]
- Xu G, Guo W, Gu X, Wang Z, Wang R, et al. Hydrogen sulfide-specific and NIR-light-controllable synergistic activation of fluorescent theranostic prodrugs for imaging-guided chemo-photothermal cancer therapy. CCS Chem 2020;2:527-38. [DOI: 10.31635/ccschem.020.201900072]
- Tang L, Yang Z, Zhou Z, Ma Y, Kiesewetter DO, et al. A logic-gated modular nanovesicle enables programmable drug release for on-demand chemotherapy. Theranostics 2019;9:1358-68. [PMID: 30867836 DOI: 10.7150/thno.32106]
- Yang J, Zhai S, Qin H, Yan H, Xing D, et al . NIR-controlled morphology transformation and pulsatile drug delivery based on multifunctional phototheranostic nanoparticles for photoacoustic imaging-guided photothermal-chemotherapy. Biomaterials 2018;176:1-12. [PMID: 29842986 DOI: 10.1016/j.biomaterials.2018.05.033]