CT Imaging Features of Patients Infected with 2019 Novel Coronavirus
1State Key Laboratory of Molecular Vaccinology and Molecular Diagnostics & Center for Molecular Imaging and Translational Medicine, School of Public Health, Xiamen University, Xiamen 361102, China
2Department of Radiology, Xiang’an Hospital of Xiamen University, Xiamen 361102, China
3Fujian Provincial Key Laboratory of Innovative Drug Target Research, School of Pharmaceutical Science, Xiamen University, Xiamen 361102, China
*Correspondence to: Dr. Gang Liu E-mail: gangliu.cmitm@xmu.edu.cn; Prof. Shuaidong Huo E-mail: huosd@xmu.edu.cn; Prof. Jingsong Mao E-mail: maojingsong163@163.com
Received: October 27 2020; Revised: December 12 2020; Accepted: December 24 2020; Published Online: January 25 2021.
Cite this paper:
Tianhong Yao, Huirong Lin, Jingsong Mao, Shuaidong Huo and Gang Liu. CT Imaging Features of Patients Infected with 2019 Novel Coronavirus. BIO Integration 2021; 2(1): 5–11.
DOI: 10.15212/bioi-2020-0038. Available at: https://bio-integration.org/
Download citation
© 2021 The Authors. This is an open access article distributed under the terms of the Creative Commons Attribution License (https://creativecommons.org/licenses/by/4.0/). See https://bio-integration.org/copyright-and-permissions/
Abstract
Novel coronavirus pneumonia is an acute, infectious pneumonia caused by a novel coronavirus infection. Computed tomographic (CT) imaging is one of the main methods to screen and diagnose patients with this disease. Here, the importance and clinical value of chest CT examination in the diagnosis of COVID-19 is expounded, and the pulmonary CT findings of COVID-19 patients in different stages are briefly summarized, thus providing a reference document for the CT diagnosis of COVID-19 patients.
Keywords
Chest CT images, COVID-19, diagnosis stages, novel coronavirus pneumonia.
Overview of COVID-19
Coronavirus disease 2019 (COVID-19) is an acute, infectious pneumonia caused by severe acute respiratory syndrome coronavirus 2 (SARS-CoV-2) infection after full genetic testing [1, 2]. Coronaviruses are enveloped segmental positive RNA viruses belonging to the Coronaviridae family and the Nidovirales order. Coronaviruses are widespread among humans and other mammals, and can cause severe respiratory, intestinal, liver, and nervous system diseases [3]. SARS-CoV-2 belongs to the genus coronavirus, and its genetic characteristics are significantly different from severe acute respiratory syndrome coronavirus (SARS-CoV) and Middle East respiratory syndrome coronavirus (MERS-CoV) and are more similar to bat SARS-like coronaviruses (bat-SL-CoV ZC45 and bat-SL-CoV ZXC21) [4–6]. The confirmed human-to-human transmission of SARS-CoV-2 [7–10] makes it a highly infectious virus, resulting in the ongoing global pandemic. People are generally susceptible, normally with an incubation period of 1–14 days [8], but the case fatality rate is higher in the elderly and people with underlying diseases [11, 12]. Respiratory droplets and contact transmission are the main routes of infection [13]. The virus can also be spread by aerosols, especially in a relatively closed environment. Furthermore, recent research has suggested that the virus can be spread through feces and urine [14, 15]. Patients infected with SARS-CoV-2 usually have a history of epidemiological exposure, and a small number of patients show signs of throat congestion and tonsil swelling when infected. COVID-19 patients mainly present symptoms of lower respiratory tract infection, such as dry cough, fever, dyspnea, sputum production, etc. Besides, there is the possibility of accompanying symptoms of fatigue, myalgia or arthralgia, headache and chills [16–18]. In severe cases, SARS-CoV-2 can cause acute respiratory distress syndrome (ARDS) and sepsis. Asymptomatic infected people might also become the source of infection.
The importance of computed tomography imaging in the diagnosis of COVID-19
Currently, the diagnosis of COVID-19 mainly consists of a hematological examination, nucleic acid testing, and medical imaging (X-ray and computed tomography [CT] scan). A clinical blood test can be used for COVID-19 identification; indicators includes routine blood tests, liver and kidney function, and electrolyte assessments. For most patients in the early stage of COVID-19, the number of peripheral blood leukocytes will be normal or will decrease, but the number of lymphocytes will decrease [16, 19]. The liver enzymes, myoglobin, and myozyme, will increase in some patients [16]. Inflammatory response indicators, such as C-reactive protein (CRP) and erythrocyte sedimentation rate (ESR), increase in most patients, but procalcitonin levels remain normal [20, 21]. For severe patients, the D-dimer typically increases, and the number of peripheral blood lymphocytes decreases progressively [22, 23]. However, as some other diseases can also induce a similar testing result, the blood test is unlikely a reliable standalone tool to confirm COVID-19 infection [24].
Generally, the standard method of COVID-19 confirmation is real-time reverse transcription polymerase chain reaction (RT-PCR) after obtaining nucleic acid samples from the respiratory tracts of subjects [25]. Nonetheless, in the actual anti-epidemic process, there are problems such as the insufficient number of basic nucleic acid detection kits, long detection time, and the existence of false negatives [26]. Although RT-PCR has become increasingly available a year into the epidemic, it is still helpful to ascertain the radiological characteristics of the COVID-19 patients.
Along with laboratory testing, imaging examination is another important method in the diagnosis of COVID-19, especially for patients with false-negative RT-PCR results or with limited access to RT-PCR examinations [27, 28]. Chest X-ray is a two-dimensional projection technology based on overlapping images, so its density resolution is not as good as that of a chest CT examination. For example, overlying heart or rib images might obscure the pulmonary pathology, and the rate of missed diagnosis of pulmonary lesions is relatively high [29–35]. By contrast, chest CT imaging, as a cross-sectional three-dimensional imaging technique without overlapping structure interference [36, 37], can provide a very clear display of the early, slight inflammatory changes in the lung. Irrespective, for the imaging of lung stroma or lung parenchyma, its specificity, detection rate, sensitivity, and negative or positive predictive values are all better than using X-rays. In addition, its fast-reporting speed and strong feasibility [38] also make it a vital player in COVID-19 diagnosis.
The clinical value of CT imaging in diagnosis can be summarized as follows. First, to identify the presence or absence of lesions in the lung. Second, to clarify the range, degree, and stage of the disease [39, 40], as well as to assist in clinical classification, disease progression monitoring, and post-treatment efficacy evaluation [41, 42]. Third, to predict the outcome of this disease in combination with clinical and laboratory indicators with the assistance of radiomics and deep learning [43, 44]. Finally, to distinguish COVID-19 from other lung diseases, especially other coronavirus diseases, such as SARS and MERS [45].
Different diseases might sometimes exhibit exactly the same scan features using chest CT imaging. Therefore, chest CT imaging cannot substitute for nucleic acid detection to confirm COVID-19. Nevertheless, CT imaging is a powerful supplementary means to spot suspected cases and to track close contacts, especially in epidemic areas where nucleic acid testing is not applicable, and a large number of suspected cases fail to be confirmed.
CT imaging diagnosis of COVID-19 at various stages
COVID-19 can be divided into early stage, progressive stage, severe stage, and recovery stage according to the scope and type of lesions. The CT scanning images of each period are distinct [39, 46]. However, there is no time standard for CT staging; it mainly depends on the CT reexamination comparison during the disease course of a specific patient.
Early stage
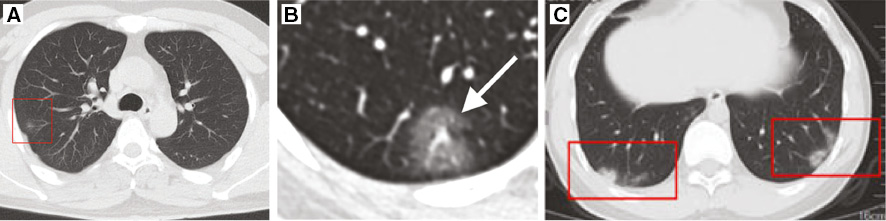
In the early stage of COVID-19, CT imaging shows unilateral or bilateral lungs with localized inflammatory infiltrates, usually with the irregular, patchy, round-like, subsegmental, or segmental ground-glass opacity (GGO) [47], associated with vascular engorgement, thickening [48], and traveling within the lesion [39]. It can also show a variety of manifestations, such as ground-glass shadow, consolidation shadow, nodule shadow, interlobular septal thickening, and interstitial change [48]. GGO is often seen in the early stage of COVID-19, and it is a kind of vascular-perfusion abnormality [49]. GGO is mostly manifested as a light cloudy shape, and the vascular texture and margins are often clearly visible [50, 51]. At this time, the pathological changes are dominated by exudate and inflammatory cell infiltration, and the alveoli are filled with exudate [52]. In terms of the distribution of lesions, they often invade cortical lung tissue at the very beginning, which can be visually summarized as the route of “rural encirclement of cities”. The peripheral subpleural involvement of intrapulmonary inflammation is more common in the early course of the disease, which might be related to pathological mechanisms that initially involve the terminal bronchioles and the pulmonary parenchyma around the respiratory bronchioles, and then the whole pulmonary lobules [53]. The morphology of the lesions in the early stage is mainly in three forms: solitary and round lesions (Figure 1A,B), single-lobed and large-sized lesions, or multi-lobed and multi-focal (Figure 1C). In a few cases, the transluminance of part of the lung parenchyma increases, and there is a mosaic-like change with the surrounding dense shadow. This might be due to an inflammatory response involving the bronchioles, which stimulates vasoconstriction and causes air retention in the distal alveoli. Special CT features seen during the early stage of COVID-19 include multiple flaxy ground glass shadows with a grid-like internal texture [54]. It is noteworthy that the thin ground glass density shadow and micronodular shadow, usually appearing in the early stage, can be easily overlooked. A small number of COVID-19 patients present negative CT findings in the early course of the disease but show positively upon reexamination [55], which indicates that chest CT imaging lacks complete sensitivity, especially in the early stage of the infection and incubation period [56]. It is more likely to have a precursor phase of viral infection, presenting symptoms before the appearance of imaging findings by CT examination. Special attention should be given to asymptomatic patients [57], who might present positive CT findings or positive viral nucleic acid test results.
Figure 1 CT images of COVID-19 patients in the early stage. (A) The image from a 36-year-old man with a 2-day history of fatigue, fever, and sore throat shows a single GGO in the left lung (red box). (Reproduced with permission [58], Copyright 2020 Radiological Society of North America.) (B) The image from a 43-year-old woman whose images show normal lung 3 days previously shows a new solitary, rounded, peripheral GGO in the right lower lobe (arrow). (Reproduced with permission [59], Copyright 2020 Radiological Society of North America.) (C) The image from a 24-year-old man with a 7-day history of mild fever, dry coughs, and weakness of unknown cause shows multiple patchy shadows in both lungs (red boxes). (Reproduced with permission [60], Copyright 2020 BioMed Central Ltd.)
Progressive stage
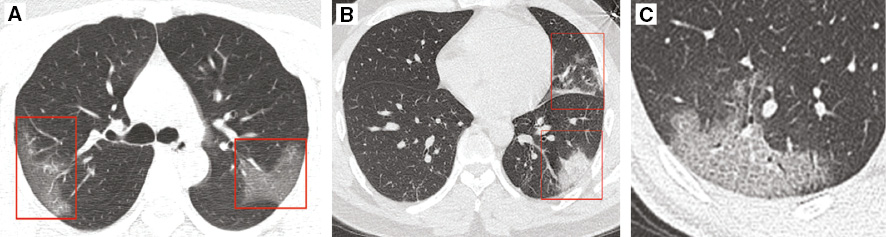
The consolidation of lung tissue is an indicator of disease progression [61, 62]. The CT characteristic findings of COVID-19 in the progressive stage are as follows: 1) the lesions extend in number and scope involving multiple pulmonary lobes (Figure 2A), and some lesions are consolidated (Figure 2B); 2) ground glass shadow coexists with consolidation shadow or striated shadow (in irregular, patchy, round-like, and anti-butterfly shape, scattered or diffused patches even fusing into large patches with increased density [39]); 3) sometimes crazy-paving signs appears [47, 51] (Figure 2C), accompanied by interlobular septal thickening and bronchopneumonia signs [39]. Additionally, there is the possibility of a reversed halo sign and pulmonary nodules with a halo sign, but this is rare [63, 64].
Figure 2 CT images of COVID-19 patients in the progressive stage. (A) The image from a 33-year-old woman shows progressive GGOs in both right upper lobe and left superior lobe (red boxes), without subpleural sparing. (Reproduced with permission [54], Copyright 2020 Radiological Society of North America.) (B) The image from a 36-year-old man shows consolidation progressed from GGOs in left lower lobe (red boxes). (Reproduced with permission [58], Copyright 2020 Radiological Society of North America.) (C) The image shows crazy-paving pattern. (Reproduced with permission [65], Copyright 2020 Radiological Society of North America.)
During the progressive stage, the pathological changes can be dramatic upon reexamination, even within a short period. As the effusion of the liquid phase inside the alveolar of the pneumonitis is caused by the virus in the early stage and for the proteins inside the fluid, the leukocytes, there are less epithelial cells, showing a relatively transparent liquid membrane. Accordingly, a lower density and an unclear boundary are presented. The original ground glass shadows or solid shadows can be fused or partially absorbed during this time, and the lesion scope and morphology often change after fusion, which is not completely distributed along with the bronchial vascular bundle. However, as the disease progresses, when combined with the bacterial infection, ever more exudate content is generated. As a result, the density of the alveolar gradually increases, and the density difference between alveolar of pneumonitis and blood vessels becomes smaller, displaying a large consolidation.
Severe stage
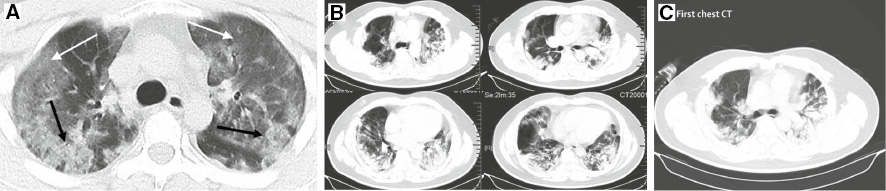
During the course of the disease, the lesions gradually spread to occupy two-thirds or even the whole of the lung, which can be accompanied by pleural reaction and interlobar pleural thickening. The lesions on CT imaging present as diffuse lesions of double lungs [66], GGO combined with consolidation and paving stone signs, are often accompanied by a fiber cable shadow (Figure 3A). A “white lung” would present when the diffuse lesions are further developed [51, 62]. During this time, a consolidation shadow is the main feature, accompanied by a ground glass shadow (Figure 3B). This might also be accompanied by pleural adhesion. Also, pleural effusion is more common in severe and critical COVID-19 patients. Pulmonary bronchogram (Figure 3C), lung parenchyma extensive exudation, lung structure distortion, subsegmental atelectasis, and other possible manifestations might also be seen [67]. More importantly, the pleural parallel sign can be viewed as the most valuable characteristic [68].
Figure 3 CT images of COVID-19 patients in the severe stage. (A) The image from a 29-year-old man requiring admission to an intensive care unit shows diffuse bilateral confluent and patchy GGOs (white arrows) and consolidative pulmonary opacities (black arrows). (Reproduced with permission [59], Copyright 2020 Radiological Society of North America.) (B) Images from a 40-year-old man show bilateral multiple lobular and subsegmental areas of consolidation on day 15 after symptom onset. (Reproduced with permission [70], Copyright 2020 Elsevier Ltd.) (C) The image shows mass high-density shadows in both lungs, accompanied with bright bronchogram, namely bronchoinflation sign. (Reproduced with permission [71], Copyright 2020 Elsevier Ltd.)
During the severe stage of COVID-19, the lesions of patients progress rapidly, and can increase by more than 50% within 48 h. This results in the rapid deterioration of patients’ conditions, aggravation of breathing difficulties, and high mortality. After analyzing 1023 deaths among COVID-19 patients up to February 11, 2020, in China, Wu et al. [69] concluded that the case fatality rate for critical cases is 49%, and that for cases with the underlying disease this rate is even higher. Among those who died, 10.5% had cardiovascular disease, 7.3% had diabetes, 6.3% had chronic respiratory disease, 6.0% had hypertension, and 5.6% had cancer.
Recovery stage
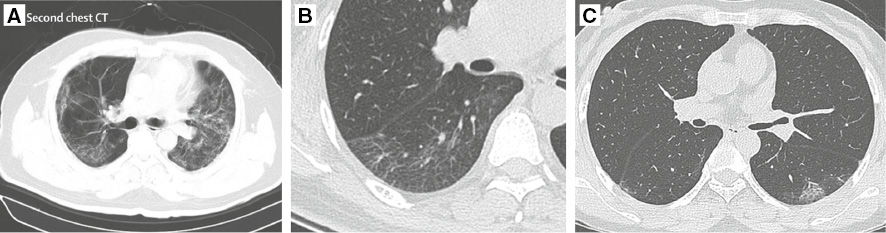
During the convalescent stage, the range of lesions and the density in the lungs of COVID-19 patients decrease [55], and the consolidation shadow gradually changes to ground glass density shadow (Figure 4A). Ultimately, the lesions will appear as small fiber stripe shadows [72] (Figure 4B) or completely disappear (Figure 4C), and the pleural effusion will be fully absorbed [7].
Figure 4 CT images of COVID-19 patients in the recovery stage. (A) The image shows GGOs gradually changed from mass consolidation shadow, though the lesion is still relatively large. (Reproduced with permission [71], Copyright 2020 Elsevier Ltd.) (B) The image from a 47-year-old woman shows minimal residual GGOs and parenchymal bands, with linear opacities being observed. (Reproduced with permission [65], Copyright 2020 Radiological Society of North America.) (C) The image from a 46-year-old woman shows GGOs are mostly resolved. (Reproduced with permission [74], Copyright 2020 Radiological Society of North America.)
The start time of lesion absorption varies from person to person, and there is no obvious specificity. In most cases, the symptoms begin to ease at ∼1 week after the onset of pneumonia, while the CT images begin to normalize later. The return to the negativity of the CT imaging and nucleic acid detection results might be unsynchronized, and can occur in either order [60]. Intrapulmonary lesions might be completely absorbed, but might also be organized, in which situation the time of recovery for severe cases is delayed. Some cases can change from normal type or from the state of remission of symptoms (nucleic acid test to negative) to severe disease (nucleic acid test to positive) in about 10 days [73].
In addition to the characteristic CT findings of each stage of COVID-19 introduced separately above, the relationship between the frequency of CT abnormity and infection time course has been studied by Bernheim et al. [75]. These authors found that with disease development, CT manifestations become more diverse, including more consolidation and the aggravation of bilateral lobe involvement. The process of lesion development of COVID-19 can be compared to <uni-201C>a piece of candy melting<uni-201D>: as the disease progresses, the initial consolidation area begins to absorb, the density decreases, and gradually becomes a ground glass density shadow, just like a piece of candy melting.
Not all patients are lucky enough to go through these four stages, ending with recovery. Because of autoimmunity and active treatment, most patients get better quickly, and the scope and density of the lesions are reduced before developing into severe disease, followed by gradual recovery. Meanwhile, some patients experience early, progressive, and severe stages, gradually improve, and eventually recover or enter a chronic phase. However, the therapeutic effect of a small number of patients is worse. Combined with other pathogens infection, the lesions extend rapidly, which eventually causes death.
The specification of CT imaging in the diagnosis of COVID-19
Specific attention should be paid to the operation specifications of CT in practical applications. First, all CT equipment should be equipped with the necessary protection, including a lead rubber gonadal protective apron, a lead rubber neck sleeve, a lead rubber hat and so on. Second, the accompany examiners should not stay in the machine room in non-specialized circumstances, and they should wear lead protective clothing during the CT test. Third, the legitimacy judgment of X-ray examination for women of child-bearing age, pregnant women, and infants should be strictly strengthened [76]. Generally, it is critical to do the best job protecting the gonads and other organs in the examination of infants and adolescents. Pregnant women should not accept a CT examination of the lower abdomen if not in urgent necessary. Beyond that, CT examination for COVID-19 patients should be applied to people who have had contact history, display symptoms or can show pathogenic evidence, rather than the whole population including numerous asymptomatic subjects without contact history [56].
Moreover, virus transmission during the CT procedure also poses a threat to the people being examined and the imaging technician [56]. Hence, during the application of CT imaging for COVID-19 identification, a series of adjustments have to be implemented. For example, staggering the use of dedicated CT scanners in fever clinics to avoid cross-infection, strictly disinfecting rooms before and after each examination, arranging examinations time ahead of schedule to minimize contact among people in the waiting areas, as well as strengthening radiographers perception of the associated risk [77].
Conclusions
In summary, there are various methods in terms of the diagnosis of COVID-19, CT imaging is a powerful supplementary means, especially in spotting suspected cases and tracking close contacts in a timely fashion.
Chest CT imaging of COVID-19 patients mainly shows ground-glass, density shadows, and cotton-mass and reticular nodules, distributed across both lungs. The subpleural distribution of the lower lungs is dominant, which is more prominent than that of the middle and upper lobes. In the early stage of the disease, there are single or multiple patchy, subsegmental, or segmental ground glass shadows, and interstitial changes, mainly involving the external lung and interstitial lung, which can also be accompanied by interlobular septa thickening. In most cases, air bronchiole can be seen; then, it develops into multiple ground glass shadows and infiltration shadows. Frequently, ground glass shadows, consolidation shadows and strip shadows can coexist at this stage. In some severe cases, diffuse lesions of both lungs can be found, and lung consolidation might be accompanied by a pleural reaction.
Although chest CT imaging has many advantages and plays an important role in COVID-19 diagnosis, it should not be employed excessively and should be used with special caution because of the potential harm from the associated radiation. In addition, as the CT manifestations of some other diseases are similar to that of COVID-19, a comprehensive diagnosis should be used to confirm the result, thereby reducing the risk of misdiagnosis. Combining the patient’s epidemiological history, clinical symptoms, and laboratory examinations, and correctly recognizing the chest CT imaging manifestations can help to accurately diagnose SARS-CoV-2 infection.
Conflict of interest
The authors declare no competing financial interest.
Acknowledgments
The authors acknowledge the support by the Novel Coronavirus Prevention Emergency Scientific Research Project, Xiamen University (20720200036 and 20720200019).
References
- Lu RJ, Zhao X, Li J, Niu PH, Yang B, et al. Genomic characterisation and epidemiology of 2019 novel coronavirus: implications for virus origins and receptor binding. Lancet 2020;395:565-74. [PMID: 32007145 DOI: 10.1016/s0140-6736(20)30251-8]
- Xu XT, Chen P, Wang JF, Feng JN, Zhou H, et al. Evolution of the novel coronavirus from the ongoing Wuhan outbreak and modeling of its spike protein for risk of human transmission. Sci China Life Sci 2020;63:457-60. [PMID: 32009228 DOI: 10.1007/s11427-020-1637-5]
- Mubarak A, Alturaiki W, Hemida MG. Middle East respiratory syndrome coronavirus (MERS-CoV): infection, immunological response, and vaccine development. J Immunol Res 2019;2019:6491738. [PMID: 31089478 DOI: 10.1155/2019/6491738]
- Zhou P, Yang XL, Wang XG, Hu B, Zhang L, et al. A pneumonia outbreak associated with a new coronavirus of probable bat origin. Nature 2020;579:270-3. [PMID:32015507 DOI: 10.1038/s41586-020-2012-7]
- Chu DKW, Pan Y, Cheng SMS, Hui KPY, Krishnan P, et al. Molecular diagnosis of a novel coronavirus (2019-nCoV) causing an outbreak of pneumonia. Clin Chem 2020;66:549-55. [PMID: 32031583 DOI: 10.1093/clinchem/hvaa029]
- Chen Y, Liu QY, Guo DY. Emerging coronaviruses: genome structure, replication, and pathogenesis. J Med Virol 2020;92:418-23. [PMID: 31967327 DOI: 10.1002/jmv.25681]
- Ziyaeifard M, Ziyaeifard P. Cardiac anesthesia and COVID-19 outbreak: what should we know? J Res Med Sci 2020;25:89. [PMID: 33273934 DOI: 10.4103/jrms.JRMS_336_20]
- Li Q, Guan XH, Wu P, Wang XY, Zhou L, et al. Early transmission dynamics in Wuhan, China, of novel coronavirus-infected pneumonia. N Engl J Med 2020;382:1199-207. [PMID: 31995857 DOI: 10.1056/NEJMoa2001316]
- Wu P, Hao XX, Lau EHY, Wong JY, Leung KSM, et al. Real-time tentative assessment of the epidemiological characteristics of novel coronavirus infections in Wuhan, China, as at 22 January 2020. Euro Surveill 2020;25. [PMID:31992388 DOI: 10.2807/1560-7917.ES.2020.25.3.2000044]
- Chan JF, Yuan S, Kok KH, To KK, Chu H, et al. A familial cluster of pneumonia associated with the 2019 novel coronavirus indicating person-to-person transmission: a study of a family cluster. Lancet 2020;395:514-23. [PMID: 31986261 DOI: 10.1016/s0140-6736(20)30154-9]
- Wang WE, Tang JM, Wei FQ. Updated understanding of the outbreak of 2019 novel coronavirus (2019-nCoV) in Wuhan, China. J Med Virol 2020;92:441-7. [PMID: 31994742 DOI: 10.1002/jmv.25689]
- Guo LX, Wei D, Zhang XX, Wu YR, Li QY, et al. Clinical Features predicting mortality risk in patients with viral pneumonia: the MuLBSTA score. Front Microbiol 2019;10:2752. [PMID: 31849894 DOI: 10.3389/fmicb.2019.02752]
- Munster VJ, Koopmans M, van Doremalen N, van Riel D, de Wit E. A novel coronavirus emerging in China – key questions for impact assessment. N Engl J Med 2020;382:692-4. [PMID: 31978293 DOI: 10.1056/NEJMp2000929]
- Kim YI, Kim SG, Kim SM, Kim EH, Park SJ, et al. Infection and rapid transmission of SARS-CoV-2 in ferrets. Cell Host Microbe 2020;27:704-9.e2. [PMID: 32259477 DOI: 10.1016/j.chom.2020.03.023]
- Chen YF, Chen LJ, Deng QL, Zhang GQ, Wu KS, et al. The presence of SARS-CoV-2 RNA in feces of COVID-19 patients. J Med Virol 2020;92:833-40. [PMID: 32243607 DOI: 10.1002/jmv.25825]
- Guan WJ, Ni ZY, Hu Y, Liang WH, Ou CQ, et al. Clinical characteristics of coronavirus disease 2019 in China. N Engl J Med 2020;382:1708-20. [PMID: 32109013 DOI: 10.1056/NEJMoa2002032]
- Liu H, Gao JY, Wang YY, Jie J, Luo JJ, et al. Epidemiological and clinical characteristics of 2019 novel coronavirus disease (COVID-19) in Jilin, China: a descriptive study. Medicine (Baltimore) 2020;99:e23407. [PMID: 33217886 DOI: 10.1097/md.0000000000023407]
- Zhang LT, Kong X, Li XJ, Zhu JZ, Liu SP, et al. CT imaging features of 34 patients infected with COVID-19. Clin Imaging 2020;68:226-31. [PMID: 32425337 DOI: 10.1016/j.clinimag.2020.05.016]
- Wang DW, Hu B, Hu C, Zhu FF, Liu X, et al. Clinical characteristics of 138 hospitalized patients with 2019 novel coronavirus-infected pneumonia in Wuhan, China. JAMA 2020;323:1061-9. [PMID: 32031570 DOI: 10.1001/jama.2020.1585]
- Shi SB, Qin M, Cai YL, Liu T, Shen B, et al. Characteristics and clinical significance of myocardial injury in patients with severe coronavirus disease 2019. Eur Heart J 2020;41:2070-9. [PMID: 32391877 DOI: 10.1093/eurheartj/ehaa408]
- Zhang B, Zhang J, Chen H, Chen LY, Chen QY, et al. Novel coronavirus disease 2019 (COVID-19): relationship between chest CT scores and laboratory parameters. Eur J Nucl Med Mol Imaging 2020;47:2083-9. [PMID: 32399620 DOI: 10.1007/s00259-020-04854-3]
- Lin LY, Zhong CM, Rao SS, Lin HG, Huang RF, et al. Clinical characteristics of 78 cases of patients infected with coronavirus disease 2019 in Wuhan, China. Exp Ther Med 2021;21:7. [PMID: 33235616 DOI: 10.3892/etm.2020.9439]
- Liang WH, Liang HR, Ou LM, Chen BF, Chen A, et al. Development and validation of a clinical risk score to predict the occurrence of critical illness in hospitalized patients with COVID-19. JAMA Intern Med 2020;180:1081-9. [PMID: 32396163 DOI: 10.1001/jamainternmed.2020.2033]
- Grasselli G, Zangrillo A, Zanella A, Antonelli M, Cabrini L, et al. Baseline characteristics and outcomes of 1591 patients infected with SARS-CoV-2 admitted to ICUs of the Lombardy region, Italy. JAMA 2020;323:1574-81. [PMID: 32250385 DOI: 10.1001/jama.2020.5394]
- Corman VM, Landt O, Kaiser M, Molenkamp R, Meijer A, et al. Detection of 2019 novel coronavirus (2019-nCoV) by real-time RT-PCR. Euro Surveill 2020;25. [PMID: 31992387 DOI: 10.2807/1560-7917.Es.2020.25.3.2000045]
- Lu CY, Bai HL, Yuan Y, Lu Q. The value of CT imaging for COVID-19 pneumonia: report of a false-negative nucleic acid test case. J Thorac Dis 2020;12:2827-9. [PMID: 32642192 DOI: 10.21037/jtd.2020.03.62]
- Xie XZ, Zhong Z, Zhao W, Zheng C, Wang F, et al. Chest CT for Typical 2019-nCoV pneumonia: relationship to negative RT-PCR testing. Radiology 2020;296:200343. [PMID: 32049601 DOI: 10.1148/radiol.2020200343]
- Kottlors J, Große Hokamp N, Fervers P, Bremm J, Fichter F, et al. Early extrapulmonary prognostic features in chest computed tomography in COVID-19 pneumonia: bone mineral density is a relevant predictor for the clinical outcome – a multicenter feasibility study. Bone 2020;144:115790. [PMID: 33301962 DOI: 10.1016/j.bone.2020.115790]
- Hayden GE, Wrenn KW. Chest radiograph vs. computed tomography scan in the evaluation for pneumonia. J Emerg Med 2009;36:266-70. [PMID: 18571356 DOI: 10.1016/j.jemermed.2007.11.042]
- Figueroa-Casas JB, Brunner N, Dwivedi AK, Ayyappan AP. Accuracy of the chest radiograph to identify bilateral pulmonary infiltrates consistent with the diagnosis of acute respiratory distress syndrome using computed tomography as reference standard. J Crit Care 2013;28:352-7. [PMID: 23566733 DOI: 10.1016/j.jcrc.2012.12.002]
- Esayag Y, Nikitin I, Bar-Ziv J, Cytter R, Hadas-Halpern I, et al. Diagnostic value of chest radiographs in bedridden patients suspected of having pneumonia. Am J Med 2010;123:88.e81-5. [PMID: 20102999 DOI: 10.1016/j.amjmed.2009.09.012]
- Basi SK, Marrie TJ, Huang JQ, Majumdar SR. Patients admitted to hospital with suspected pneumonia and normal chest radiographs: epidemiology, microbiology, and outcomes. Am J Med 2004;117:305-11. [PMID: 15336579 DOI: 10.1016/j.amjmed.2004.03.029]
- Börjesson J, Latifi A, Friman O, Beckman MO, Oldner A, et al. Accuracy of low-dose chest CT in intensive care patients. Emerg Radiol 2011;18:17-21. [PMID: 20694568 DOI: 10.1007/s10140-010-0895-6]
- Mueller-Lenke N, Rudez J, Staub D, Laule-Kilian K, Klima T, et al. Use of chest radiography in the emergency diagnosis of acute congestive heart failure. Heart 2006;92:695-6. [PMID: 16159971 DOI: 10.1136/hrt.2005.074583]
- Ebner L, Bütikofer Y, Ott D, Huber A, Landau J, et al. Lung nodule detection by microdose CT versus chest radiography (standard and dual-energy subtracted). Am J Roentgenol 2015;204:727-35. [PMID: 25794062 DOI: 10.2214/ajr.14.12921]
- Bhandary A, Prabhu GA, Rajinikanth V, Krishnan PT, Satapathy SC, et al. Deep-learning framework to detect lung abnormality – a study with chest X-ray and lung CT scan images. Pattern Recogn Lett 2020;129:271-8. [DOI: 10.1016/j.patrec.2019.11.013]
- Jin YH, Cai L, Cheng ZS, Cheng H, Deng T, et al. A rapid advice guideline for the diagnosis and treatment of 2019 novel coronavirus (2019-nCoV) infected pneumonia (standard version). Mil Med Res 2020;7:4. [PMID: 32029004 DOI: 10.1186/s40779-020-0233-6]
- Franquet T. Imaging of pulmonary viral pneumonia. Radiology 2011;260:18-39. [PMID: 21697307 DOI: 10.1148/radiol.11092149]
- Dai H, Zhang X, Xia J, Zhang T, Shang YL, et al. High-resolution chest CT features and clinical characteristics of patients infected with COVID-19 in Jiangsu, China. Int J Infect Dis 2020;95:106-12. [PMID: 32272262 DOI: 10.1016/j.ijid.2020.04.003]
- Zhang B, Zhang J, Chen H, Yang K, Zhang SX. Unmatched clinical presentation and chest CT manifestation in a patient with severe coronavirus disease 2019 (COVID-19). Quant Imaging Med Surg 2020;10:871-3. [PMID: 32355651 DOI: 10.21037/qims.2020.03.12]
- Ye Z, Zhang Y, Wang Y, Huang ZX, Song B. Chest CT manifestations of new coronavirus disease 2019 (COVID-19): a pictorial review. Eur Radiol 2020;30:1-9. [PMID: 32193638 DOI: 10.1007/s00330-020-06801-0]
- Rodriguez-Morales AJ, Cardona-Ospina JA, Gutiérrez-Ocampo E, Villamizar-Peña R, Holguin-Rivera Y, et al. Clinical, laboratory and imaging features of COVID-19: a systematic review and meta-analysis. Travel Med Infect Dis 2020;34:101623. [PMID: 32179124 DOI: 10.1016/j.tmaid.2020.101623]
- Saw PE, Jiang SP. The significance of interdisciplinary integration in academic research and application. BIO Integration 2020;1:2-5. [DOI: 10.15212/bioi-2020-0005]
- Yao MK, Saw PE, Jiang SP. Coronavirus pneumonia and pulmonary thromboembolism. BIO Integration 2021;1:178-84. [DOI: 10.15212/bioi-2020-0030]
- Chen Y, Jiang GF, Li Y, Tang YT, Xu YF, et al. A survey on artificial intelligence in chest imaging of COVID-19. BIO Integration 2021;1:137-46. [DOI: 10.15212/bioi-2020-0015]
- Pan YY, Guan HX, Zhou SC, Wang YJ, Li Qian, et al. Initial CT findings and temporal changes in patients with the novel coronavirus pneumonia (2019-nCoV): a study of 63 patients in Wuhan, China. Eur Radiol 2020;30:3306-9. [PMID: 32055945 DOI: 10.1007/s00330-020-06731-x]
- Torkian P, Ramezani N, Kiani P, Bax MR, Akhlaghpoor S. Common CT findings of novel coronavirus disease 2019 (COVID-19): a case series. Cureus 2020;12:e7434. [PMID: 32351814 DOI: 10.7759/cureus.7434]
- Han R, Huang L, Jiang H, Dong J, Peng HF, et al. Early clinical and CT manifestations of coronavirus disease 2019 (COVID-19) pneumonia. Am J Roentgenol 2020;20:1-6. [PMID: 32181672 DOI: 10.2214/ajr.20.22961]
- Lang M, Som A, Mendoza DP, Flores EJ, Reid N, et al. Hypoxaemia related to COVID-19: vascular and perfusion abnormalities on dual-energy CT. Lancet Infect Dis 2020;20:1365-6. [PMID: 32359410 DOI: 10.1016/S1473-3099(20)30367-4]
- Liu HH, Liu F, Li JN, Zhang TT, Wang DB, et al. Clinical and CT imaging features of the COVID-19 pneumonia: focus on pregnant women and children. J Infect 2020;80:e7-e13. [PMID: 32171865 DOI: 10.1016/j.jinf.2020.03.007]
- Chen HX, Ai L, Lu H, Li HJ. Clinical and imaging features of COVID-19. Radiol Infect Dis 2020;7:43-50. [PMID: 32346593 DOI: 10.1016/j.jrid.2020.04.003]
- Zeng Z, Xu L, Xie XY, Yan HL, Xie BJ, et al. Pulmonary pathology of early-phase COVID-19 pneumonia in a patient with a benign lung lesion. Histopathology 2020;77:823-31. [PMID: 32374419 DOI: 10.1111/his.14138]
- Li RQ, Tian JG, Yang F, Lv L, Yu J, et al. Clinical characteristics of 225 patients with COVID-19 in a tertiary hospital near Wuhan, China. J Clin Virol 2020;127:104363. [PMID: 32298988 DOI: 10.1016/j.jcv.2020.104363]
- Lei JQ, Li JF, Li X, Qi XL. CT Imaging of the 2019 novel coronavirus (2019-nCoV) pneumonia. Radiology 2020;295:18. [PMID: 32003646 DOI: 10.1148/radiol.2020200236]
- Ling ZK, Xu X, Gan QX, Zhang LG, Luo LP, et al. Asymptomatic SARS-CoV-2 infected patients with persistent negative CT findings. Eur J Radiol 2020;126:108956. [PMID: 32199142 DOI: 10.1148/radiol.2020200236]
- Liu WH, Wang XW, Cai ZQ, Wang X, Huang XL, et al. Chest CT as a screening tool for COVID-19 in unrelated patients and asymptomatic subjects without contact history is unjustified. Quant Imaging Med Surg 2020;10:876-7. [PMID: 32355653 DOI: 10.21037/qims.2020.04.02]
- Mok C, Seet YM, Tan S-M. Breast cancer multidisciplinary management during COVID-19 pandemic: experiences and strategies used by a Singapore breast surgical unit. BIO Integration 2020;1:95-100. [DOI: 10.15212/bioi-2020-0012]
- Huang PK, Liu TZ, Huang LS, Liu HL, Lei M, et al. Use of chest CT in combination with negative RT-PCR assay for the 2019 novel coronavirus but high clinical suspicion. Radiology 2020;295:22-3. [PMID: 32049600 DOI: 10.1148/radiol.2020200330]
- Chung M, Bernheim A, Mei XY, Zhang N, Huang MQ, et al. CT Imaging features of 2019 novel coronavirus (2019-nCoV). Radiology 2020;295:202-7. [PMID: 32017661 DOI: 10.1148/radiol.2020200230]
- Gao J, Liu JQ, Wen HJ, Liu H, Hu WD, et al. The unsynchronized changes of CT image and nucleic acid detection in COVID-19: reports the two cases from Gansu, China. Respir Res 2020;21:96. [PMID: 32321530 DOI: 10.1186/s12931-020-01363-7]
- Song FX, Shi NN, Shan F, Zhang ZY, Shen J, et al. Emerging 2019 novel coronavirus (2019-nCoV) pneumonia. Radiology 2020;295:210-7. [PMID: 32027573 DOI: 10.1148/radiol.2020200274]
- Inchingolo R, Smargiassi A, Moro F, Buonsenso D, Salvi S, et al. The diagnosis of pneumonia in a pregnant woman with coronavirus disease 2019 using maternal lung ultrasound. Am J Obstet Gynecol 2020;223:9-11. [PMID: 32360111 DOI: 10.1016/j.ajog.2020.04.020]
- Farias LPG, Strabelli DG, Sawamura MVY. COVID-19 pneumonia and the reversed halo sign. J Bras Pneumol 2020;46:e20200131. [PMID: 32321009 DOI: 10.36416/1806-3756/e20200131]
- Li Y, Xia LM. Coronavirus Disease 2019 (COVID-19): role of chest CT in diagnosis and management. Am J Roentgenol 2020;214:1280-6. [PMID: 32130038 DOI: 10.2214/ajr.20.22954]
- Pan F, Ye TH, Sun P, Gui S, Liang B, et al. Time course of lung changes at chest CT during recovery from coronavirus disease 2019 (COVID-19). Radiology 2020;295:715-21. [PMID: 32053470 DOI: 10.1148/radiol.2020200370]
- Zhong Z, Hu Y, Yu QZ, Li YX, Li P, et al. Multistage CT features of coronavirus disease 2019. J Centr South Univ Med Sci 2020;45:250-6. [PMID: 32386015 DOI: 10.11817/j.issn.1672-7347.2020.200144]
- Li MZ, Lei PG, Zeng BL, Li ZL, Yu P, et al. Coronavirus disease (COVID-19): spectrum of CT findings and temporal progression of the disease. Acad Radiol. 2020;27:603-8. [PMID: 32204987 DOI: 10.1016/j.acra.2020.03.003]
- Wu J, Feng LC, Xian XY, Qiang J, Zhang J, et al. Novel coronavirus pneumonia (COVID-19) CT distribution and sign features. Chin J Tuberc Respir Dis 2020;43:321-26. [PMID: 32125131 DOI: 10.3760/cma.j.cn112147-20200217-00106]
- Wu ZY, McGoogan JM. Characteristics of and important lessons from the coronavirus disease 2019 (COVID-19) outbreak in China: summary of a report of 72 314 cases from the Chinese Center for Disease Control and Prevention. JAMA 2020;323:1239-42. [PMID: 32091533 DOI: 10.1001/jama.2020.2648]
- Huang CL, Wang YM, Li XW, Ren LL, Zhao JP, et al. Clinical features of patients infected with 2019 novel coronavirus in Wuhan, China. Lancet 2020;395:497-506. [PMID: 31986264 DOI: 10.1016/s0140-6736(20)30183-5]
- Chen NS, Zhou M, Dong X, Qu JM, Gong FY, et al. Epidemiological and clinical characteristics of 99 cases of 2019 novel coronavirus pneumonia in Wuhan, China: a descriptive study. Lancet 2020;395:507-13. [PMID: 32007143 DOI: 10.1016/s0140-6736(20)30211-7]
- Xu YH, Dong JH, An WM, Lv XY, Yin XP, et al. Clinical and computed tomographic imaging features of novel coronavirus pneumonia caused by SARS-CoV-2. J Infect 2020;80:394-400. [PMID: 32109443 DOI: 10.1016/j.jinf.2020.02.017]
- Zhou SC, Zhu TT, Wang YJ, Xia LM. Imaging features and evolution on CT in 100 COVID-19 pneumonia patients in Wuhan, China. Eur Radiol 2020;30. [PMID: 32367418 DOI: 10.1007/s00330-020-06879-6]
- Duan YN, Qin J. Pre- and posttreatment chest CT findings: 2019 novel coronavirus (2019-nCoV) pneumonia. Radiology 2020;295:21. [PMID: 32049602 DOI: 10.1148/radiol.2020200323]
- Bernheim A, Mei XY, Huang MQ, Yang Y, Fayad ZA, et al. Chest CT findings in coronavirus disease-19 (COVID-19): relationship to duration of infection. Radiology 2020;119:200463. [PMID: 32077789 DOI: 10.1148/radiol.2020200463]
- Duan YN, Zhu YQ, Tang LL, Qin J. CT features of novel coronavirus pneumonia (COVID-19) in children. Eur Radiol 2020;30:1-7. [PMID: 32291501 DOI: 10.1007/s00330-020-06860-3]
- Qu JM, Yang WJ, Yang YZ, Qin L, Yan FH. Infection Control for CT equipment and radiographers’ personal protection during the coronavirus disease (COVID-19) outbreak in China. Am J Roentgenol 2020;215:1-5. [PMID: 32352309 DOI: 10.2214/ajr.20.23112]