Modifying an Implant: A Mini-review of Dental Implant Biomaterials
1School of Life Sciences, Faculty of Science, University of Technology Sydney, Ultimo, NSW, Australia
*Correspondence to: Martin P. Stewart, E-mail: martin.stewart@uts.edu.au
Received: September 7 2020; Revised: December 7 2020; Accepted: January 4 2021; Published Online: March 19 2021
Cite this paper:
Oliver K. Semisch-Dieter, Andy H. Choi, Besim Ben-Nissan and Martin P. Stewart. Modifying an Implant: A Mini-review of Dental Implant Biomaterials. BIO Integration 2021; 2(1): 12–21.
DOI: 10.15212/bioi-2020-0034. Available at: https://bio-integration.org/
Download citation
© 2021 The Authors. This is an open access article distributed under the terms of the Creative Commons Attribution License (https://creativecommons.org/licenses/by/4.0/). See https://bio-integration.org/copyright-and-permissions/
Abstract
Dental implants have been used as far back as 2000BC, and since then have developed into highly sophisticated solutions for tooth replacement. It is becoming increasingly important for the materials used in dental implants to exhibit and maintain favorable long-term mechanical, biological and more recently, aesthetic properties. This review aims to assess the biomaterials used in modern dental implants, introducing their properties, and concentrating on modifications to improve these biomaterials. Focus is drawn to the prominent biomaterials, titanium (Ti) and zirconia due to their prevalence in implant dentistry. Additionally, novel coatings and materials with potential use as viable improvements or alternatives are reviewed. An effective dental biomaterial should osseointegrate, maintain structural integrity, resist corrosion and infection, and not cause systemic toxicity or cytotoxicity. Current materials such as bioactive glass offer protection against biofilm formation, and when combined with a titanium–zirconium (TiZr) alloy, provide a reliable combination of properties to represent a competitive alternative. Further long-term clinical studies are needed to inform the development of next-generation materials.
Keywords
Biocompatibility, biomaterials, dental implant, titanium, zirconia.
Significance Statement
Biomaterials have become essential for modern implants. A suitable implant biomaterial integrates into the body to perform a key function, whilst minimizing negative immune response. Focusing on dentistry, the use of dental implants for tooth replacement requires a balance between bodily response, mechanical structure and performance, and aesthetics. This mini-review addresses the use of biomaterials in dental implants with significant comparisons drawn between Ti and zirconia. Attention is drawn to optimizing surface modification processes and the additional use of coatings. Alternatives and novel developments are addressed, providing potential implications of combining biomaterials to form novel composites that combine and synergize the benefits of each material.
Introduction
Biomaterials are crucial for modern medical applications, and in the last several decades, these materials have been refined and improved for applications seen in dentistry, orthopedics, drug delivery, and cardiology. Candidate materials include polymers, metals (and their alloys), ceramics, composites (e.g. carbon fiber), and glass. For clinical use, the material must not cause any adverse or damaging effects to the patient [1]. This concept is known as biocompatibility and was described by Williams as, “the ability of a biomaterial to perform its desired function with respect to a medical therapy, without eliciting any undesirable local or systemic effects in the recipient or beneficiary of that therapy, but generating the most appropriate beneficial cellular or tissue response to that specific situation, and optimizing the clinically relevant performance of that therapy” [2].
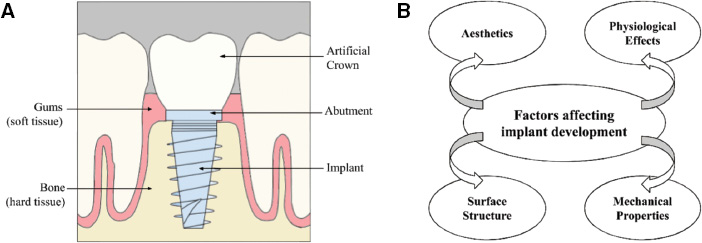
The application of biomaterials as a dental implant is shown in Figure 1A; an endosseous fixture is used to replace the root and support a dental prosthesis. Dental implants have become an evidence-based treatment for the replacement of missing teeth. Selecting a biomaterial for a dental implant requires additional considerations for biological, mechanical, and aesthetic properties. Modern dental implants need to feature effective osseointegration and maintain long-term stability of their favorable properties to maintain both the implant’s structure and the integrity of surrounding hard and soft tissue [3, 4].
Figure 1 (A) Illustrates a cross-sectional view of a dental implant and the surrounding oral tissue. (B) Selecting the appropriate material to use for the implant requires considerations of implant durability, cell adhesion, and physiological implications for implant biocompatibility, and aesthetic concerns for patient satisfaction.
This review aims to assess the current state of biomaterials (Ti, zirconia, and novel materials) used in dental implants. Materials are assessed on their attributes, characteristics, comparison of strengths and weaknesses, biocompatibility, and new advancements in addressing any issues or concerns.
Titanium
Ti is widely used for medical applications and is currently the most commonly used material for dental implants. The popularity is in part due to the combination of its tensile strength, biocompatibility, ability to osseointegrate, density, corrosion resistance, and inert properties. Pure Ti, while being safe for most clinical use, has been observed to form an accumulation of Ti ions around the implant site. While no material is entirely bioinert, such ions released from an implant that fails to osseointegrate may induce proinflammatory responses from sensitization. Such failure occurs when there is a lack of biomechanical stability due to inadequate osseointegration. Stability can be promoted by modifying the implant’s physiochemical properties and surface topography. Observations from failed Ti implants show an increased lymph node Ti ion concentration by 7.4–9 times and lung Ti ion concentration by 2.2–3.8 times when compared to a successfully integrated implant [5, 6] (Table 1). Ti dental implants have been occasionally observed to result in an allergic reaction. However, the exact mechanism for Ti ion release and systemic effects remains unclear [7].
Table 1 Summary of in vivo and in vitro studies assessing clinically relevant factors of Ti and zirconia dental implants
| Authors | Study type | Description | Conclusion |
|---|---|---|---|
| Wang et al. (2019) [5] | In vitro | Investigating macrophage and fibroblasts behavior at the bone–implant interface of commercial implants | Surface composition (Ti vs ZLA vs Ti-Zi) had little effect on macrophage or fibroblast behavior, while hydrophilicity promoted lower inflammation and better soft tissue integration |
| El-Hadad et al. (2018) [24] | In vitro and in vivo | Evaluating in vitro and in vivo performance of functionally graded (FG) biomaterials of calcium phosphate/Ti alloys | FG Ti implants (Ti6Al4V) demonstrated the best in vitro cytocompatibility and in vivo systemic toxicity and osseointegration results |
| Roehling et al. (2017) [45] | In vitro | Comparing biofilm formation on zirconia and Ti implants | Zirconia presented a significant reduction in biofilm and plaque formation compared to Ti implant surfaces |
| Siddiqui et al. (2019) [46] | In vitro | Assessing the effect of bacterial and mechanical fatigue on zirconia implants | Mechanical loading and colonizing bacteria did not induce significant degradation or damage. The authors consider zirconia a suitable alternative to Ti implants |
| Langhoff et al. (2008) [47] | In vivo: sheep model | Comparing the osseointegration of modified Ti and zirconia implant surfaces | All implants achieved successful osseointegration, with zirconia reaching slightly higher initial bone-implant contact (BIC). Overall, there were no significant differences in BIC |
| Schwarz et al. (2019) [58] | In vitro | Assessing the effect of Ti and zirconia particles on osteoblast and fibroblast activity, and cytokine expression | Both Ti and zirconia particles reduced osteoblast and fibroblast cell viability, with no proinflammatory effect. The findings do require in vivo validation |
| Sánchez et al. (2014) [77] | In vitro | Assessing biofilm formation on hydroxyapatite, Ti and zirconia implant surfaces | Biofilm formed irrespective of implant material, while only the morphology and structure of the biofilms were different |
| Rosentritt et al. (2014) [78] | In vitro | Investigating fracture resistance and implant failure | Bonded/screwed zirconia implants displayed lower fracture resistance compared to two-piece Ti and one-piece zirconia implants |
| Rottmar et al. (2019) [79] | In vitro | Investigating the blood interaction, and resulting osseointegration, at the bone-implant interface of microstructure Ti and zirconia implants. | Thrombogenicity was the highest on zirconia surfaces compared to Ti. It was suggested that a higher thrombogenicity promotes osseointegration, however, similarly micro-structured Ti maintained good osseointegration potential |
| Zeller et al. (2020) [80] | In vivo | Investigation of biofilm formation on gold and silver metal alloys, PEEK, zirconia, and TiZr alloy implants. | PEEK, Zirconia and TiZr materials demonstrated similar biofilm formation on commercially available implants. Only gold and silver-based materials showed reduced biofilm growth |
| Herrmann et al. (2020) [81] | In vivo | Examining early and mature biofilms on Ti and zirconia implants at different roughness. | Zirconia showed significantly higher total bacterial cell counts, but could be due to surface roughness. Biofilm formation and total bacterial cell counts could be assumed to be caused by surface roughness |
| Kubasiewicz-Ross et al. (2018) [82] | In vivo: pig model | Studying the osseointegration of commercially available Ti and zirconia implants | Overall zirconia displayed similar levels of osseointegration, measured through BIC. Differences between implant material yielded no statistically important differences |
Surface modifications of Ti implants are performed to improve osseointegration and modulate cell adhesion. The largest post-operative issue with such implants is biofilm-induced mucositis, inflammation of mucous membranes, which can further develop into peri-implantitis, the inflammation of the gum and the surrounding bone structure. The first generation of surface modification was developed in the 1960s, where machined Ti (smooth surface) was used to promote osseointegration by leaving a small degree of roughness. Second generation surface modifications have been widely available since the 1990s and improve on the first generation by creating a microscopically rough surface topography. Finally, the current third generation (also known as bioactive surfaces) maintains similar roughness to the second generation and are modified chemically or topographically to promote osseointegration [8]. Most surface topographies minimize vertical deviation to 1 μm or less, effectively deterring biofilm formation. Current surface topographies include anodization, sandblasting, and polishing, however, conclusive evidence on which specific surface topographies are optimal and why remains undetermined [9].
Alternative alloys
It is known that Ti can form alloys to solve reactivity concerns [1]. Vanadium (V) and aluminum (Al) are common alloying elements for Ti (seen in Ti6Al4V alloy). Individually each element has shown potential adverse effects in high concentrations, causing carcinogenicity and neurotoxicity [10–12]. However, reports on V also demonstrate antidiabetic effects and resulted in reduced weight gain and gastrointestinal discomfort [1, 13]. Attempts are being made to replace these alloying elements with less toxic elements such as niobium (Nb), tantalum (Ta), and palladium (Pd), to improve biocompatibility; however, Ti6Al4V remains a common choice [14]. When comparing a Ti alloy to surgical stainless steel and cobalt alloys, the superior quality of Ti is its corrosion resistance. The ability for Ti alloys to withstand corrosive environments and develop an oxide layer with a shorter repassivation time compared to other metal alloys, aids in preventing a release of ions which can potentially be toxic (cobalt) or cause allergic reactions (nickel, found in stainless steel) [15].
A unique alloy, TiZr has shown clinical success in the past decade. Under the trade name Roxolid, Institut Straumann AG, Basel, Switzerland (a 15% Zr, 85% Ti composition), the TiZr alloy was designed for dental implants, becoming a viable alternative to zirconia and other Ti-based implants [16]. TiZr offers enhanced osseointegration compared to Ti6Al4V and pure Ti and avoids the use of toxic alloying elements. Additionally, corrosion resistance can potentially reduce problems associated with peripheral Ti ion concentrations [17–19]. A recent study observed that TiZr retains the ability for surface enhancement without compromising the mechanical strength of the implant [20]. While TiZr dental implants do not offer the aesthetic qualities of zirconia, they demonstrate highly preferable qualities among clinically available Ti alloy options.
TiNb is another alloy with favorable properties and provides a low elastic modulus similar to human cortical bone. It is clinically significant as it reduces the issue of stress concentration between the implant and bone, thus promoting osseointegration. This alloy improves on other functional aspects compared to pure Ti, possessing higher toughness, hardness, and corrosion resistance. TiNb has been proposed as a suitable alternative for replacing failed hard tissue [21, 22].
Recent trends
Recent trends in the field point toward the utility of novel ideas such as: (1) the development of implant coatings, and (2) the incorporation of alternative elements (e.g. iodine (I) and strontium (Sr)) to support Ti implants. The next generation of therapeutic implants may incorporate nano-engineered surface topographies. The use of anodized titania (titanium dioxide, TiO2) nanotubes (TNT) on the surface of Ti implants shows promising results. These NTs offer advantages in topography, mechano-transduction, drug release, and mediating toxicity. The TNTs mimic the topographical scale of surrounding native tissues to significantly upregulate protein absorption. The bone remodeling caused by mechanical strain stimulates cells at the bone–implant interface to promote initial attachment and continued adhesion. TNTs that are capable of local drug release potentially allow for direct targeting of the implant site and a reduction in toxicity compared to systemic administration. Together these factors contribute to influence cellular functions and immunomodulatory responses towards dental implants [23, 24]. Compared to conventional Ti implants, TNTs have been observed to orchestrate osteogenesis [25].
A recent development in surface modifications is plasma immersion ion implantation which provides a uniform application over complex surface geometries, while reducing overall cost and processing time. The in vitro testing of an oxygen plasma immersion ion implantation (OPIII) to a Ti implant identified improvements in protein expression and corrosion resistance [26]. The use of OPIII is capable of producing a bioactive oxide film which was determined to improve in vitro cell differentiation and in vivo osseointegration. It is undetermined to what degree the process optimizes the implant’s surface properties (topography, wettability, and roughness), however, the most current research has observed no significant alteration [27]. In its current state, OPIII has a good potential to become a viable surface modification through further research.
Additionally, an in vivo study demonstrated the ability to use macrophage polarization via NTs to augment osseointegration [28]. The property of local drug release is another significant advantage of this technology. While some attempts have been made to incorporate antibiotics into NTs, these traditional or organic antibiotics pose the risk of resistance and are limited by selective toxicity. This has resulted in attention towards inorganic antibacterial agents, such as silver. Using silver as a coating has shown strong antimicrobial effects, however, it poses biocompatibility issues. Studies are testing the effect of loading silver nanoparticles onto TNTs. These TNTs use a reducing agent to disperse silver nanoparticles from the coating and can aid in patient care during the initial postoperative risk of infection. Clinical safety and molecular mechanism still require further studies [29]. Long-term studies are required to translate this technology for clinical application, and cost will also need to be considered for commercial implementation.
Continued research in coatings has led to novel improvements on hydroxyapatite (HAp) for Ti6Al4V implants. In situ synthesis of HAp-based nanocomposites including chitosan and polycaprolactone/fluoride (PCL/F) substitution aim to utilize the advantages of HAp with promoting the formation of bone-like apatite at the bone–implant interface, while minimizing the brittleness of HAp. A sol–gel method and alkali-treated Ti is used to provide a homogenous, crack-free coating that does not suffer from any delamination. Both nanocomposites required a minimum 10 wt.% of HAp to provide the desired results with the respective composite [30, 31]. Research for chitosan/HAp identified improved cellular response at lower HAp content (10 wt.%), with higher content (50 and 60 wt.%) providing improved surface adhesion strength, roughness, and hydrophilicity [30]. It was noted with PCL/F that HAp content up to 30 wt.% improved similar surface properties, and higher corrosion resistance [31]. Both coatings meet the required performance of bioactive coatings and show potential for future clinical application.
An alternative material to Ti is Ta. Ta is a useful biomaterial due to being highly bioactive and holds similar properties to Ti regarding corrosion resistance and biocompatibility. The improvement over Ti is the optimization of the osseointegration process. However, it is a high-density material which is expensive to manufacture. Therefore, combining the properties of Ti and Ta, research has focused on developing Ta oxide films. Preliminary research observed promising results, improving wear resistance to microbial and chemical degradation. Improved osseointegration was also observed with increased osteoblastic activity and morphology. Finally, the study did not indicate any increased bacterial cell adhesion when compared to conventional Ti implants [32].
Adding alternative elements is not a new concept, and continuing with the idea of surface treatment, the addition of Sr is a possibility. Historically Sr is biologically known for promoting osteoblast activity and inhibiting osteoclast activity. Oral administration of Sr may cause adverse effects; therefore, surface incorporation (on Ti implants) has been preliminarily observed to increase early bone osseointegration [33]. Another potential element is I, an essential element with antiseptic properties and may be a useful biomaterial for dental implants. A previous study indicated that I-supported Ti implants in orthopedic applications substantially reduced the incidence of inflammation. The enhanced implants exhibited cytocompatibility and increased antimicrobial activity [34].
Another approach to modification is altering the implant design; the use of porous Ti has been researched to improve integration into hard tissue. The sponge-like framework also allows for antibacterial agents to be directly incorporated into the implant surface or via degradable drug carriers [35]. Currently challenges around optimization of the structure and high manufacturing cost are a barrier to implementation of this technology in the clinic [36].
A recent study has improved on the capability of porous Ti through using micropore channels in Ti implants to preserve alveolar height without additional growth factors. The canine in vivo model provides evidence in minimizing alveolar bone loss, while promoting cell viability, proliferation, and osteogenic differentiation [37]. Natural bone has periodontal ligament fibers which apply the required mechanical stimulation to maintain the correct height of alveolar bone. Traditional dental implants lack this function due to a direct osseointegration at the bone–implant interface [38]. The horizontal traction of the micropores simulates the periodontal ligament fibers which provide a potential clinical opportunity for higher quality dental implants. Overall, Ti offers many unique opportunities to be alloyed and altered. Thus, novel permutations are continually being invented and designed to improve the material for more effective clinical use.
Zirconia
Dental implants made from the bioceramic zirconia (zirconium dioxide; ZrO2) are a non-metal alternative to Ti implants that address aesthetic concerns. Widely available as partially stabilized zirconia (PSZ), it provides a transformative toughening of the biomaterial [39]. Additionally, zirconia advantageously displays a significant reduction in plaque affinity and proinflammatory responses in surrounding soft tissue [40].
Compared to Ti implants, similar or better results from zirconia have been observed in in vitro cell culture experiments. These results however are not directly comparable, probably due to inconsistencies in influential variables of cell type, incubation conditions, and surface properties. Surface modifications for both implant materials are well characterized and contribute a significant effect on the bone–implant interface. Nanoporous zirconia surfaces have indicated promise for improved cell growth as observed by larger cell size and higher cell count compared to polished zirconia and surface modified Ti implants (acid etched and sandblasted) [41, 42]. Assessing the biocompatibility of zirconia, the cytotoxicity is comparable to Ti nanoparticles. High concentrations of zirconia nanoparticles inhibit osteogenic differentiation and may induce necrotic or apoptotic effects on tissue. Proinflammatory effects for ziconia have not been reported. Research is thus limited and requires further study to rule out potential biocompatibility issues [43, 44].
The most significant flaw of zirconia is an aging phenomenon known as low-temperature degradation (LTD) which transforms the tetragonal surface back to the initial monoclinic structure in the presence of water or a humid environment [45, 46]. Zirconia surfaces have shown lower bacterial adhesion compared to Ti; however, these bacteria are still able to cause deterioration of zirconia surfaces [47]. Currently, no research has been able to adequately study the effect of oral bacteria on LTD. One study attempted to identify a correlative link between oral bacteria and mechanical fatigue; however, it was unable to arrive at any conclusive evidence [48]. The majority of LTD comes from manufacturing flaws. Further studies are required to observe the role of oral temperature and pH fluctuation on zirconia implants.
The success of an implant is reliant on the degree of biomaterial osseointegration. Much research in surface modifications has been conducted to enhance implant stability and bone apposition, however few optimal alterations have been identified. The use of surface topography for Ti plays a similar role in zirconia implants; however, producing modified surfaces is more complicated than in Ti due to a potential compromise of biomechanical stability. Furthermore, the current developments in surface modifications for zirconia do not have clinical applications as seen in novel surface topographies of Ti dental implants. Many clinicians remain skeptical of the osseointegrative properties of zirconia. Improvement of surface properties has taken two main approaches; (1) via optimization of surface roughness, and (2) through the application of a coating. Traditional surface modifications follow the first approach, which include air particle abrasion, acid etching, and polishing. However, these methods introduce risk of surface and internal damage, possibly leading to fracturing. An effective roughening process would make zirconia implants more viable, as optimal roughness demonstrates a similar capacity for osseointegration compared to roughened Ti implants [3, 49].
Recent trends in surface modifications
Following the second approach to surface modifications, HAp resembles the chemical composition of bone and teeth, and has been suggested as a bioactive coating for zirconia implants. The advantage is stimulating osseointegration through the supply of calcium and phosphate ions [50]. Research has indicated that HAp-coated metallic implants heal faster and attach more readily and completely to the surrounding tissue [51]. While design of the coating’s properties would need to be optimized, transitioning this coating to zirconia may also prove difficult, because of potential bioactivity of calcium phosphate coatings [52–55]. A novel implementation of etching (selective infiltration via hydrofluoric acid and a molten glass coating) has been found to maintain surface chemistry and alter the roughness for effective osseointegration [56, 57]. Other novel surface modifications include biofunctionalization via an adhesive peptide (arginine–glycine–aspartate, fibronectin, or collagen), and laser treatment. Laser-treated zirconia exerted no surface contamination and promoted fibroblast attachment, an effect attributed to improved surface wettability [58, 59]. The immobilized peptide in biofunctionalization enhances the biocompatibility of the implant through extracellular matrix regulation, as peptides such as fibronectin encourage cell adhesion and bone formation [60, 61]. While being effective for in vitro treatments, these modifications are clinically limited by a lack of supporting research and the question of longevity remains open [58].
A promising approach to improving bioactivity of zirconia without a substantial compromise of mechanical properties is through a gradated design and composite outer layer. While the calcium phosphate composite has contraindications in the literature, the gradated design aids to ensure no coating detachment after implantation which otherwise may result in implant failure [62].
Bioactive surface coatings, such as HAp, can result in delamination of the coating from the implant after a long loading time. Control of the coating thickness is a strategy to mitigate this issue. Simple and repeatable methods of arc induction or plasma spraying are used to provide accurate thickness control and maintain the required chemical effect. Plasma anodization and fluoridation are alternative methods to control surface energy on zirconia implants. Diode laser application can be used to clean implant surfaces in the cases of peri-implantitis. Erbium: YAG and carbon dioxide lasers cannot be recommended due to their penetrative, and surface altering properties, respectively. Modification from long-term exposure to fluoride has shown enhanced contact of the bone-implant interface [63].
Another interesting surface modification includes selective infiltration etching (SIE), which creates a nanoporous surface to facilitate cell growth and attachment. The technique involves molten glass infiltration to alter the surface grain of the zirconia implant and promote grain reorganization. It is followed by acid etching to dissolve the glass, which results in a few microns of porous surface material. This is advantageous by maintaining structural integrity and creating an ideal surface for osseointegration [64].
The use of plasma immersion ion implantation has also been researched for zirconia implants. Similarly to Ti, the method implanted surface level functional groups without compromising the structural integrity of the material. The nitrogen-containing functional groups promoted early stage osseointegration in vitro. The proliferation and osteogenic properties provide evidence for a foundational method that will require future in vivo investigations [65].
Zirconia remains a viable alternative to Ti implants. While not as mechanically robust, zirconia implants satisfy a need in the consumer market for aesthetic and non-metal alternatives. Current research is developing improvements for the bone–implant interface to improve successful osseointegration and adapt to structural limitations.
Other alternatives
Graphene
The highly published carbon allotrope, graphene, has the potential for many bioapplications, including dental implants. Graphene offers reliable functionality through mechanical strength and stability. Early research of graphene identified issues related to long-term biocompatibility in an oral environment and the possibility of oxidative debris which can induce cytotoxicity. Current attempts at applications are limited by manufacturing difficulties and cost effectiveness [66]. However, future applications may deploy graphene as a nanotube coating alternative to the TNTs mentioned in Titanium – Recent Trends.
Bioactive glass
The use of bioactive glass has long been considered for its capability to bond to soft and hard tissue. It is commonly used as a reinforcement material in HAp-coatings on metallic implants to improve mechanical properties and osseointegration [67]. A recent study has proposed the use of bioactive glass as a coating to reduce the incidence of bacterial infections which result in implant failure. The bioglass was synthesized with up to 2% silver (in weight), to aid in antibacterial properties. The addition of ≥0.5% silver prevented the growth of common Gram-negative and positive bacteria (Staphylococcus aureus and Escherichia coli) [68]. Long-term structural stability and additional bacteria types specific to the oral environment, such as Streptococcus salivarius, need to be further examined.
Polymer materials
The use of fiber reinforced composites (FRC) have been used extensively within the broader fields of science and engineering. FRC implants exhibit durable mechanical performance and elasticity, with in vivo studies indicating equal biocompatibility and osseointegration compared to pure Ti. A large benefit over conventional materials is the ability to be used as a fixed implant that is mouldable in situ. The implant creates a strong adhesion to underlaying tooth substrate, transferring stress based on fiber direction. Further novel approaches have been made by embedding the FRC surface with previously mentioned bioactive glass to improve the osseointegration process [69, 70].
Another polymer of interest is a thermo plastic, polyetheretherketone (PEEK). PEEK composites can be reinforced with glass fiber or carbon fiber to replicate the biomechanics of human cortical bone, potentially decreasing bone loss and improving osseointegration. Compared to pure Ti implants, PEEK implants have a lower fracture resistance, however, they suffer from decreased stress shielding. Clinical evidence is currently lacking to determine if polymer composites will replace common Ti and zirconia implants [71, 72].
A potential biopolymer that can be considered for future directions are collagen hydrogels, which as a coating could promote osseointegration. The use of a naturally occurring polymer may provide favorable properties in terms of biocompatibility and lower cytotoxicity, due to having a low immune response. Collagen hydrogels benefit from being capable of simulating the oral microenvironment and are easy to form through self-assembly [73]. This polymer requires further research in the potential introduction of collagen hydrogels into the bone-implant interface to promote implant osseointegration.
Magnesium composite
Magnesium-based materials are not new to medical applications and often degrade during the healing process [74]. The use of alloyed magnesium raises concerns with ion release from degradation, which may cause systemic toxicity [75, 76]. Studies recognize the use of powder metallurgy as a promising approach to the development of magnesium-based biocomposites [83, 84]. Metallic or ceramic additions, such as Ti, zirconia, or zinc oxide in the metallurgy process allows for the composite matrix to be reinforced for high mechanical performance [85–88]. Using fluorapatite, calcium, or rare-earth elements such as dysprosium or gadolinium enhances corrosion resistance [86–92]. Through utilizing a bioactive, bioinert, and mechanically stable composition, a modern magnesium composite has the potential to become a viable alternative. Studies are still required to investigate if the composite can outperform alternative zirconia forms or Ti alloys.
Ceramic composites
Combinations of alumina (Al2O3) and zirconia (ZrO2 have been explored due to their high stiffness and toughness, however, they are limited by high cost and complex manufacturing methods. The addition of TiO2 has been researched to improve production through a less complex sintering process and enhanced bioactivity at the bone–implant interface. The resulting alumina-zirconia-titania ceramic has been optimized into a low-cost manufacturing process with high mechanical strength. Compared to zirconia, aging resistance has been improved, showing no signs of LTD in 40 years of simulated clinical use [93].
The inclusion of titania has promoted studies into the ceramic’s biocompatibility. An increased wettability of the ceramic surface produced a positive correlation with cell viability, with no significant cytotoxic effect. While a higher content of titania improved wettability, DNA damage was associated with the composite containing >10wt. % TiO2 [94]. The proposed implant contains less titania than the genotoxic concentration, providing enhanced surface properties and suitability for future in vivo trialing.
Conclusion and outlook
This review aims to provide an accessible overview of the use of biomaterials in implant dentistry. Focusing primarily on the use of Ti and zirconia, our discussion expands on the properties of these biomaterials and novel modifications that can be implemented to improve their utility. Alternative biomaterials are also introduced; however, analysis is limited due to lack of extensive clinical and laboratory data. This review seeks to provide guidance for continued research into modifying Ti and zirconia-based dental implants. While it takes account of current clinical implications of novel modifications, this is not the focus of the review. Future reviews can address the clinical management of a wider range of dental implants as a complement to the current review.
In modern dentistry there is a growing demand for improvements in mechanical, bioactive, and aesthetic properties of tooth replacement implants. Furthermore, the success of dental implants depends on their capability for osseointegration, corrosion resistance, infection prevention, and durability against degradation. Current commercially available biomaterials exhibit a unanimous capability for osseointegration, however, they suffer from limitations in their clinical application. Ti-based materials offer superior mechanical properties (such as tensile strength and stability) that achieve reduced implant failure and longer lifespan, while zirconia focuses on satisfying aesthetic purposes by mimicking natural tooth-like color. Surface topographies will remain an essential aspect of implants in optimizing cell adhesion for improving osseointegration and reducing biofilm formation [9]. The importance of maintaining mechanical and aesthetic concerns is supported by López-Píriz et al., who also agree that the impact of peri-implantitis from biofilm formation is another significant cause of implant failure in modern dental implants [4]. Bacterial colonization is reduced by novel biomaterials such as a bioactive glass coating, which prevents growth on the implant surface. Additionally, the use of certain coatings induces a similar effect to surface topographies for cell and tissue adhesion, while providing additional mechanical support and corrosion resistance. Corrosion will remain an issue as no material is entirely bioinert. Novel materials and compositions such as graphene and polymers require additional long-term studies to observe potential effects on stability and biocompatibility [66, 71]. The utilization of bioactive glass as a coating for polymer and metallic implants presents an effective improvement for osseointegration [70].
Future directions for implants are likely to retain the use of Ti and zirconia, based on patient preference for mechanical vs aesthetic and metal vs non-metal (Table 2). Zirconia used in a PSZ form should undergo further development in surface modifications via coatings or innovations in altered topography to maintain its position as a competitive alternative to Ti. Improved surface properties will enhance adhesion to soft and hard tissues and inhibit bacterial colonization [53]. Ti currently offers the most versatility in design for alloying, surface modification, and coating adhesion. A TiZr implant may be the most promising alloy due to the lack of potentially toxic ions (such as V and Al) from the composition, adequate mechanical strength, and surface modification capability [16]. For example, a productive future direction may be an acid-etched TiZr dental implant with a bioactive glass coating. In summary, dental implants are well-established but require continued measurement and optimisation of biocompatibility and material properties to improve the technology.
Table 2 Main characteristics and future direction of biomaterials for dental implants. Materials are ordered by appearance
| Benefits | Concerns | Anticipated future directions | |
|---|---|---|---|
| Ti | Biocompatible, fatigue and corrosion resistant, and high mechanical strength [1, 5, 6] | Low wear resistance, potential Ti ion cytotoxicity [7–10] | Alloys (e.g. TiZr), surface modification (topography and coatings) [23, 25, 27, 35, 36] |
| zirconia | Natural tooth-like color, wear-resistant, biocompatible [39, 40] | Brittle, biofilm formation, cytotoxicity [45, 57, 58] | Novel methods for surface topography modification [54–56] |
| Ta | High bioactivity, similar mechanical properties to Ti | High density, difficult to manufacture | Ta oxide film coating [34] |
| Graphene | High mechanical strength and stability | Biocompatibility, production efficacy and cost | Nanotube coating [66] |
| PEEK | Simulate cortical bone, reduced effects of stress shielding | Low fracture resistance | Further research for clinical evidence [71, 72] |
| Magnesium composite | Biocompatible [74] | Low corrosion resistance, hydrogen evolution from degradation [75, 76] | Refining composition of alloy/composite to enhance mechanical strength and bioactivity [83–92] |
Conflicts of interest
The authors declare no conflict of interest.
References
- Kaur M, Singh K. Review on titanium and titanium based alloys as biomaterials for orthopaedic applications. Mater Sci Eng C 2019;102:844-62. [PMID: 31147056 DOI: 10.1016/j.msec.2019.04.064]
- Williams DF. On the mechanisms of biocompatibility. Biomaterials 2008;29:2941-53. [PMID: 18440630 DOI: 10.1016/j.biomaterials.2008.04.023]
- Roehling S, Schlegel KA, Woelfler H, Gahlert M. Zirconia compared to titanium dental implants in preclinical studies – A systematic review and meta-analysis. Clin Oral Implants Res 2019;30:365-95. [PMID: 30916812 DOI: 10.1111/clr.13425]
- López-Píriz R, Cabal B, Goyos-Ball L, Fernández A, Bartolomé JF, et al. Current state-of-the-art and future perspectives of the three main modern implant-dentistry concerns: aesthetic requirements, mechanical properties, and peri-implantitis prevention. J Biomed Mater Res A 2019;107:1466-75. [PMID: 30786152 DOI: 10.1002/jbm.a.36661]
- Wang Y, Zhang Y, Sculean A, Bosshardt DD, Miron RJ. Macrophage behavior and interplay with gingival fibroblasts cultured on six commercially available titanium, zirconium, and titanium-zirconium dental implants. Clin Oral Investig 2019;23:3219-27. [PMID: 30415441 DOI: 10.1007/s00784-018-2736-z]
- Frisken KW, Dandie GW, Lugowski S, Jordan G. A study of titanium release into body organs following the insertion of single threaded screw implants into the mandibles of sheep. Aust Dent J 2002;47:214-7. [PMID: 12405460 DOI: 10.1111/j.1834-7819.2002.tb00331.x]
- Delgado-Ruiz R, Romanos G. Potential causes of titanium particle and ion release in implant dentistry: a systematic review. Internat J Mol Sci 2018;19:3585. [PMID: 30428596 DOI: 10.3390/ijms19113585]
- Ivanovski S. Osseointegration – the influence of implant surface. Ann R Australas Coll Dent Surg 2010;20:82. [PMID: 22046744]
- Dhaliwal JS, Rahman NA, Knights J, Ghani H, de Albuquerque Junior RF. The effect of different surface topographies of titanium implants on bacterial biofilm: a systematic review. SN Appl Sci 2019;1:615. [DOI: 10.1007/s42452-019-0638-6]
- Flaten TP. Aluminium as a risk factor in Alzheimer’s disease, with emphasis on drinking water. Brain ResBull 2001;55:187-96. [PMID: 11470314 DOI: 10.1016/s0361-9230(01)00459-2]
- Ress NB, Chou BJ, Renne RA, Dill JA, Miller RA, et al. Carcinogenicity of inhaled vanadium pentoxide in F344/N rats and B6C3F1 mice. Toxicol Sci 2003;74:287-96. [PMID: 12773761 DOI: 10.1093/toxsci/kfg136]
- Shaw CA, Petrik MS. Aluminum hydroxide injections lead to motor deficits and motor neuron degeneration. J Inorg Biochem 2009;103:1555-62. [PMID: 19740540 DOI: 10.1016/j.jinorgbio.2009.05.019]
- Srivastava AK. Anti-diabetic and toxic effects of vanadium compounds. Mol Cell Biochem 2000;206:177-82. [PMID: 10839208 DOI: 10.1023/a:1007075204494]
- Matsuno H, Yokoyama A, Watari F, Uo M, Kawasaki T. Biocompatibility and osteogenesis of refractory metal implants, titanium, hafnium, niobium, tantalum and rhenium. Biomaterials 2001;22:1253-62. [PMID: 11336297 DOI: 10.1016/s0142-9612(00)00275-1]
- Solar RJ, Pollack SR, Korostoff E. In vitro corrosion testing of titanium surgical implant alloys: An approach to understanding titanium release from implants. J Biomed Mater Res 1979;13:217-50. [PMID: 429392 DOI: 10.1002/jbm.820130206]
- Grandin HM, Berner S, Dard M. A review of titanium zirconium (TiZr) alloys for use in endosseous dental implants. Materials 2012;5:1348-60. [DOI: 10.3390/ma5081348]
- Ikarashi Y, Toyoda K, Kobayashi E, Doi H, Yoneyama T, et al. Improved biocompatibility of titanium–zirconium (Ti–Zr) alloy: tissue reaction and sensitization to Ti–Zr alloy compared with pure Ti and Zr in rat implantation study. Materi Trans 2005;46:2260-7. [DOI: 10.2320/matertrans.46.2260]
- Khan MA, Williams RL, Williams DF. Conjoint corrosion and wear in titanium alloys. Biomaterials 1999;20:765-72. [PMID: 10353659 DOI: 10.1016/s0142-9612(98)00229-4]
- Naganawa T, Ishihara Y, Iwata T, Koide M, Ohguchi M, et al. In vitro biocompatibility of a new titanium-29niobium-13tantalum-4.6zirconium alloy with osteoblast-like MG63 cells. J Periodontol 2004;75:1701-7. [PMID: 15732874 DOI: 10.1902/jop.2004.75.12.1701]
- Cordeiro JM, Faverani LP, Grandini CR, Rangel EC, da Cruz NC, et al. Characterization of chemically treated Ti-Zr system alloys for dental implant application. Mater Sci Eng C 2018;92:849-61. [PMID: 30184814 DOI: 10.1016/j.msec.2018.07.046]
- Bai Y, Deng Y, Zheng Y, Li Y, Zhang R, et al. Characterization, corrosion behavior, cellular response and in vivo bone tissue compatibility of titanium–niobium alloy with low Young’s modulus. Mater Sci Eng C 2016;59:565-76. [PMID: 26652409 DOI: 10.1016/j.msec.2015.10.062]
- El-Hadad S, Safwat EM, Sharaf NF. In-vitro and in-vivo, cytotoxicity evaluation of cast functionally graded biomaterials for dental implantology. Mater Sci Eng C 2018;93:987-95. [PMID: 30274137 DOI: 10.1016/j.msec.2018.09.003]
- Gulati K, Hamlet MS, Ivanovski S. Tailoring the immuno-responsiveness of anodized nano-engineered titanium implants. J Mater Chem B 2018;6:2677-89. [PMID: 32254221 DOI: 10.1039/c8tb00450a]
- Yeo I-SL. Modifications of dental implant surfaces at the micro- and nano-level for enhanced osseointegration. Materials 2020;13:89. [PMID: 31878016 DOI: 10.3390/ma13010089]
- Bjursten LM, Rasmusson L, Oh S, Smith GC, Brammer KS, Jin S. Titanium dioxide nanotubes enhance bone bonding in vivo. J Biomed Mater Res A 2010;92A:1218-24. [PMID: 19343780 DOI: 10.1002/jbm.a.32463]
- Yang CH. Oxygen plasma immersion ion implantation treatment enhances the human bone marrow mesenchymal stem cells responses to titanium surface for dental implant application. Clin Oral Implants Res 2015;26:166. [PMID: 24313899 DOI: 10.1111/clr.12293]
- Chen C-S, Chang J-H, Srimaneepong V, Wen J-Y, Tung O-H, et al. Improving the in vitro cell differentiation and in vivo osseointegration of titanium dental implant through oxygen plasma immersion ion implantation treatment. Surf Coat Technol 2020;399:126125. [DOI: 10.1016/j.surfcoat.2020.126125]
- Ma Q-L, Zhao L-Z, Liu R-R, Jin B-Q, Song W, et al. Improved implant osseointegration of a nanostructured titanium surface via mediation of macrophage polarization. Biomaterials 2014;35:9853-67. [PMID: 25201737 DOI: 10.1016/j.biomaterials.2014.08.025]
- Gunputh UF, Le H, Handy RD, Tredwin C. Anodised TiO2 nanotubes as a scaffold for antibacterial silver nanoparticles on titanium implants. Mater Sci Eng C 2018;91:638-44. [PMID: 30033297 DOI: 10.1016/j.msec.2018.05.074]
- Ansari Z, Kalantar M, Soriente A, Fasolino I, Kharaziha M, et al. In-situ synthesis and characterization of chitosan/hydroxyapatite nanocomposite coatings to improve the bioactive properties of Ti6Al4V substrates. Materials 2020;13:3772. [PMID: 32859071 DOI: 10.3390/ma13173772]
- Ansari Z, Kalantar M, Kharaziha M, Ambrosio L, Raucci MG. Polycaprolactone/fluoride substituted-hydroxyapatite (PCL/FHA) nanocomposite coatings prepared by in-situ sol–gel process for dental implant applications. Prog Org Coat 2020;147:105873. [DOI: 10.1016/j.porgcoat.2020.105873]
- Beline T, da Silva JHD, Matos AO, Azevedo Neto NF, de Almeida AB, et al. Tailoring the synthesis of tantalum-based thin films for biomedical application: characterization and biological response. Mater Sci Eng C 2019;101:111-9. [PMID: 31029304 DOI: 10.1016/j.msec.2019.03.072]
- Lin G, Zhou C, Lin M, Xu A, He F. Strontium-incorporated titanium implant surface treated by hydrothermal reactions promotes early bone osseointegration in osteoporotic rabbits. Clin Oral Implants Res 2019;30:777-90. [PMID: 31104360 DOI: 10.1111/clr.13460]
- Shirai T, Shimizu T, Ohtani K, Zen Y, Takaya M, et al. Antibacterial iodine-supported titanium implants. Acta Biomater 2011;7:1928-33. [PMID: 21115142 DOI: 10.1016/j.actbio.2010.11.036]
- Sternberg K, Petersen S, Grabow N, Senz V, Meyer zu Schwabedissen H, et al. Implant-associated local drug delivery systems based on biodegradable polymers: customized designs for different medical applications. Biomedi Tech 2013;58:417-27. [PMID: 23979120 DOI: 10.1515/bmt-2012-0049]
- Pałka K, Pokrowiecki R. Porous titanium implants: a review. Adv Eng Mater 2018;20:1700648. [DOI: 10.1002/adem.201700648]
- Yin S, Zhang W, Tang Y, Yang G, Wu X, et al. Preservation of alveolar ridge height through mechanical memory: a novel dental implant design. Bioact Mater 2021;6:75-83. [PMID: 32817915 DOI: 10.1016/j.bioactmat.2020.07.015]
- Ikar M, Grobecker-Karl T, Karl M, Steiner C. Mechanical stress during implant surgery and its effects on marginal bone: a literature review. Quintessence Int 2020;51:142-50. [PMID: 31781692 DOI: 10.3290/j.qi.a43664]
- Al-Amleh B, Lyons K, Swain M. Clinical trials in zirconia: a systematic review. J Oral Rehabil 2010;37:641-52. [PMID: 20406352 DOI: 10.1111/j.1365-2842.2010.02094.x]
- Akagawa Y, Hosokawa R, Sato Y, Kamayama K. Comparison between freestanding and tooth-connected partially stabilized zirconia implants after two years’ function in monkeys: a clinical and histologic study. J Prosthet Dent 1998;80:551-8. [PMID: 9813805 DOI: 10.1016/s0022-3913(98)70031-9]
- Hempel U, Hefti T, Kalbacova M, Wolf-Brandstetter C, Dieter P, et al. Response of osteoblast-like SAOS-2 cells to zirconia ceramics with different surface topographies. Clin Oral Implants Res 2010;21:174-81. [PMID: 19709059 DOI: 10.1111/j.1600-0501.2009.01797.x]
- Hempel U, Hefti T, Dieter P, Schlottig F. Response of human bone marrow stromal cells, MG-63, and SaOS-2 to titanium-based dental implant surfaces with different topography and surface energy. Clin Oral Implants Res 2013;24:174-82. [PMID: 22092368 DOI: 10.1111/j.1600-0501.2011.02328.x]
- Ben-Nissan B, Choi AH. Sol–gel production of bioactive nanocoatings for medical applications. Part I: an introduction. Nanomedicine 2006;1:311-9. [PMID: 17716161 DOI: 10.2217/17435889.1.3.311]
- Choi AH, Ben-Nissan B. Sol-gel production of bioactive nanocoatings for medical applications. Part II: current research and development. Nanomedicine 2007;2:51-61. [PMID: 17716190 DOI: 10.2217/17435889.2.1.51]
- Chevalier J. What future for zirconia as a biomaterial? Biomaterials 2006;27:535-43. [PMID: 16143387 DOI: 10.1016/j.biomaterials.2005.07.034]
- Lawson S. Environmental degradation of zirconia ceramics. J Eur Ceram Soc 1995;15:485-502. [DOI: 10.1016/0955-2219(95)00035-S]
- Roehling S, Astasov-Frauenhoffer M, Hauser-Gerspach I, Braissant O, Woelfler H, et al. In vitro biofilm formation on titanium and zirconia implant surfaces. J Periodontol 2017;88:298-307. [PMID: 27712464 DOI: 10.1902/jop.2016.160245]
- Siddiqui DA, Sridhar S, Wang F, Jacob JJ, Rodrigues DC. Can oral bacteria and mechanical fatigue degrade zirconia dental implants in vitro? ACS Biomater Sci Eng 2019;5:2821-33. [DOI: 10.1021/acsbiomaterials.9b00223]
- Langhoff JD, Voelter K, Scharnweber D, Schnabelrauch M, Schlottig F, et al. Comparison of chemically and pharmaceutically modified titanium and zirconia implant surfaces in dentistry: a study in sheep. Int J Oral Maxillofac Surg 2008;37:1125-32. [PMID: 18977118 DOI: 10.1016/j.ijom.2008.09.008]
- Pae A, Lee H, Noh K, Woo Y-H. Cell attachment and proliferation of bone marrow-derived osteoblast on zirconia of various surface treatment. J Adv Prosthodont 2014;6:96-102. [PMID: 24843393 DOI: 10.4047/jap.2014.6.2.96]
- Pardun K, Treccani L, Volkmann E, Streckbein P, Heiss C, et al. Mixed zirconia calcium phosphate coatings for dental implants: tailoring coating stability and bioactivity potential. Mater Sci Eng C 2015;48:337-46. [PMID: 25579931 DOI: 10.1016/j.msec.2014.12.031]
- Song Y-G, Cho I-H. Characteristics and osteogenic effect of zirconia porous scaffold coated with β-TCP/HA. J Adv Prosthodont 2014;6:285-94. [PMID: 25177472 DOI: 10.4047/jap.2014.6.4.285]
- Soon G, Pingguan-Murphy B, Lai KW, Akbar SA. Review of zirconia-based bioceramic: surface modification and cellular response. Ceram Int 2016;42:12543-55. [DOI: 10.1016/j.ceramint.2016.05.077]
- Aboushelib MN, Kleverlaan CJ, Feilzer AJ. Selective infiltration-etching technique for a strong and durable bond of resin cements to zirconia-based materials. J Prosthet Dent 2007;98:379-88. [PMID: 1802182 DOI: 10.1016/S0022-3913(07)60123-1]
- Aboushelib MN, Osman E, Jansen I, Everts V, Feilzer AJ. Influence of a nanoporous zirconia implant surface of on cell viability of human osteoblasts. J Prosthodont 2013;22:190-5. [PMID: 23432766 DOI: 10.1111/j.1532-849X.2012.00920.x]
- Hao L, Lawrence J. Effects of CO2 laser irradiation on the wettability and human skin fibroblast cell response of magnesia partially stabilised zirconia. Mater Sci Eng C 2003;23:627-39. [DOI: 10.1177/0885328204043546]
- Ye M, Shi B. Zirconia nanoparticles-induced toxic effects in osteoblast-like 3T3-E1 cells. Nanoscale Res Lett 2018;13:353. [PMID: 30402719 DOI: 10.1186/s11671-018-2747-3]
- Schwarz F, Langer M, Hagena T, Hartig B, Sader R. Cytotoxicity and proinflammatory effects of titanium and zirconia particles. Int J Implant Dent 2019;5:25. [PMID: 31286286 DOI: 10.1186/s40729-019-0178-2]
- Hao L, Lawrence J. Laser surface treatment of magnesia partially stabilized zirconia for enhanced human skin fibroblast cell response. J Laser Appl 2004;16:55-64. [DOI: 10.2351/1.1642634]
- Rubinstein AI, Sabirianov RF, Namavar F. Enhanced cell growth by nanoengineering zirconia to stimulate electrostatic fibronectin activation. Nanotechnology 2014;25:065101.
- Wilson CJ, Clegg RE, Leavesley DI, Pearcy MJ. Mediation of biomaterial–cell interactions by adsorbed proteins: a review. Tissue Eng 2005;11:1-18. [PMID: 15738657 DOI: 10.1089/ten.2005.11.1]
- Faria D, Pires JM, Boccaccini AR, Carvalho O, Silva FS, et al. Development of novel zirconia implant’s materials gradated design with improved bioactive surface. J Mech Behav Biomed Mater 2019;94:110-25. [PMID: 30884280 DOI: 10.1016/j.jmbbm.2019.02.022]
- Stübinger S, Homann F, Etter C, Miskiewicz M, Wieland M, et al. Effect of Er:YAG, CO2 and diode laser irradiation on surface properties of zirconia endosseous dental implants. Lasers Surg Med 2008;40:223-8. [PMID: 18366074 DOI: 10.1002/lsm.20614]
- Aboushelib MN, Salem NA, Taleb ALA, El Moniem NMA. Influence of surface nano-roughness on osseointegration of zirconia implants in rabbit femur heads using selective infiltration etching technique. J Oral Implant 2013;39:583-90. [PMID: 21905894 DOI: 10.1563/AAID-JOI-D-11-00075]
- Guo S, Liu N, Liu K, Li Y, Zhang W, et al. Effects of carbon and nitrogen plasma immersion ion implantation on bioactivity of zirconia. RSC Adv 2020;10:35917-29. [DOI: 10.1039/D0RA05853J]
- Tahriri M, Del Monico M, Moghanian A, Tavakkoli Yaraki M, Torres R, et al. Graphene and its derivatives: opportunities and challenges in dentistry. Mater Sci Eng C 2019;102:171-85. [PMID: 31146988 DOI: 10.1016/j.msec.2019.04.051]
- Choi AH, Ben-Nissan B, Matinlinna JP, Conway RC. Current perspectives: calcium phosphate nanocoatings and nanocomposite coatings in dentistry. J Dent Res 2013;92:853-9. [PMID: 23857642 DOI: 10.1177/0022034513497754]
- Gavinho SR, Prezas PR, Ramos DJ, Sá-Nogueira I, Borges JP, et al. Nontoxic glasses: Preparation, structural, electrical and biological properties. Int J Appl Ceram Technol 2019;16:1885-94. [DOI: 10.1111/ijac.13243]
- Ballo AM, Cekic-Nagas I, Ergun G, Lassila L, Palmquist A, et al. Osseointegration of fiber-reinforced composite implants: Histological and ultrastructural observations. Dent Mater 2014;30:e384-95. [PMID: 25182369 DOI: 10.1016/j.dental.2014.08.361]
- Vallittu PK. An overview of development and status of fiber-reinforced composites as dental and medical biomaterials. Acta Biomater Odontol Scand 2018;4:44-55. [PMID: 29707613 DOI: 10.1080/23337931.2018.1457445]
- Mishra S, Chowdhary R. PEEK materials as an alternative to titanium in dental implants: a systematic review. Clin Implant Dent Relat Res 2019;21:208-22. [PMID: 30589497 DOI: 10.1111/cid.12706]
- Panayotov IV, Orti V, Cuisinier F, Yachouh J. Polyetheretherketone (PEEK) for medical applications. J Mater Sci Mater Med 2016;27:118. [PMID: 27259708 DOI: 10.1007/s10856-016-5731-4]
- Xue P-P, Yuan J-d, Yao Q, Zhao Y-Z, Xu H-L. Bioactive factors-imprinted scaffold vehicles for promoting bone healing: the potential strategies and the confronted challenges for clinical production. BIO Integration 2020;1:37-54. [DOI: 10.15212/bioi-2020-0010]
- Ali M, Hussein MA, Al-Aqeeli N. Magnesium-based composites and alloys for medical applications: a review of mechanical and corrosion properties. J Alloys Compd 2019;792:1162-90. [DOI: 10.1016/j.jallcom.2019.04.080]
- Hassan SF, Gupta M. Effect of type of primary processing on the microstructure, CTE and mechanical properties of magnesium/alumina nanocomposites. Compos Struct 2006;72:19-26. [DOI: 10.1016/j.compstruct.2004.10.008]
- Kirkland NT, Staiger MP, Nisbet D, Davies CHJ, Birbilis N. Performance-driven design of Biocompatible Mg alloys. JOM 2011;63:28-34. [DOI: 10.1007/s11837-011-0089-z]
- Sánchez MC, Llama-Palacios A, Fernández E, Figuero E, Marín MJ, et al. An in vitro biofilm model associated to dental implants: structural and quantitative analysis of in vitro biofilm formation on different dental implant surfaces. Dent Mater 2014;30:1161-71. [PMID: 25110288 DOI: 10.1016/j.dental.2014.07.008]
- Rosentritt M, Hagemann A, Hahnel S, Behr M, Preis V. In vitro performance of zirconia and titanium implant/abutment systems for anterior application. J Dent 2014;42:1019-26. [PMID: 24699071 DOI: 10.1016/j.jdent.2014.03.010]
- Herrmann H, Kern J-S, Kern T, Lautensack J, Conrads G, et al. Early and mature biofilm on four different dental implant materials: an in vivo human study. Clin Oral Implants Res 2020;31:1094-104. [PMID: 32871610 DOI: 10.1111/clr.13656]
- Zeller B, Stöckli S, Zaugg LK, Astasov-Frauenhoffer M, Hauser-Gerspach I, et al. Biofilm formation on metal alloys, zirconia and polyetherketoneketone as implant materials in vivo. Clin Oral Implants Res 2020;31:1078-86. [DOI: 10.1111/clr.13654]
- Rottmar M, Müller E, Guimond-Lischer S, Stephan M, Berner S, et al. Assessing the osteogenic potential of zirconia and titanium surfaces with an advanced in vitro model. Dent Mater 2019;35:74-86. [PMID: 30424918 DOI: 10.1016/j.dental.2018.10.008]
- Kubasiewicz-Ross P, Hadzik J, Dominiak M. Osseointegration of zirconia implants with 3 varying surface textures and a titanium implant: a histological and micro-CT study. Adv Clin Exp Med 2018;27:1173-9. [PMID: 29912481 DOI: 10.17219/acem/69246]
- Witte F, Ulrich H, Rudert M, Willbold E. Biodegradable magnesium scaffolds: part 1: appropriate inflammatory response. J Biomed Mater Res A 2007;81A:748-56. [PMID: 17390368 DOI: 10.1002/jbm.a.31170]
- Zheng YF, Gu XN, Xi YL, Chai DL. In vitro degradation and cytotoxicity of Mg/Ca composites produced by powder metallurgy. Acta Biomater 2010;6:1783-91. [PMID: 19815098 DOI: 10.1016/j.actbio.2009.10.009]
- Hassan SF, Gupta M. Effect of nano-ZrO2 particulates reinforcement on microstructure and mechanical behavior of solidification processed elemental Mg. J Compos Mater 2007;41:2533-43. [DOI: 10.1177/0021998307074187].
- Lei T, Tang W, Cai S-H, Feng F-F, Li N-F. On the corrosion behaviour of newly developed biodegradable Mg-based metal matrix composites produced by in situ reaction. Corros Sci 2012;54:270-7. [DOI: 10.1016/j.corsci.2011.09.027]
- Rashad M, Pan F, Tang A, Lu Y, Asif M, Hussain S, et al. Effect of graphene nanoplatelets (GNPs) addition on strength and ductility of magnesium-titanium alloys. J Magnes Alloys 2013;1:242-8. [DOI: 10.1016/j.jma.2013.09.004]
- Umeda J, Kawakami M, Kondoh K, Ayman E-S, Imai H. Microstructural and mechanical properties of titanium particulate reinforced magnesium composite materials. Mater Chem Phys 2010;123:649-57. [DOI: 10.3390/app8112012]
- Grillo CA, Alvarez F, de Mele MAFL. Cellular response to rare earth mixtures (La and Gd) as components of degradable Mg alloys for medical applications. Colloids Surf B Biointerfaces 2014;117:312-21. [PMID: 24667077 DOI: 10.1016/j.colsurfb.2014.02.030]
- Razavi M, Fathi MH, Meratian M. Microstructure, mechanical properties and bio-corrosion evaluation of biodegradable AZ91-FA nanocomposites for biomedical applications. Mater Sci Eng A 2010;527:6938-44. [DOI: 10.1016/j.msea.2010.07.063]
- Yang L, Huang Y, Feyerabend F, Willumeit R, Kainer KU, et al. Influence of ageing treatment on microstructure, mechanical and bio-corrosion properties of Mg–Dy alloys. J Mech Behav Biomed Mater 2012;13:36-44. [PMID: 22842274 DOI: 10.1016/j.jmbbm.2012.04.007]
- Zhang S, Zhang X, Zhao C, Li J, Song Y, et al. Research on an Mg–Zn alloy as a degradable biomaterial. Acta Biomater 2010;6:626-40. [PMID: 19545650 DOI: 10.1016/j.actbio.2009.06.028]
- Camposilvan E, Leone R, Gremillard L, Sorrentino R, Zarone F, et al. Aging resistance, mechanical properties and translucency of different yttria-stabilized zirconia ceramics for monolithic dental crown applications. Dent Mater 2018;34:879-90. [PMID: 29598882 DOI: 10.1016/j.dental.2018.03.006]
- Khaskhoussi A, Calabrese L, Currò M, Ientile R, Bouaziz J, et al. Effect of the compositions on the biocompatibility of new alumina–zirconia–titania dental ceramic composites. Materials 2020;13:1374. [PMID: 32197510 DOI: 10.3390/ma13061374]