Ultrasound Neuromodulation: Integrating Medicine and Engineering for Neurological Disease Treatment
1Department of Ultrasound Medicine, Laboratory of Ultrasound Molecular Imaging, The Third Affiliated Hospital of Guangzhou Medical University, Guangzhou 510150, China
2Medical Imaging Centre, First Affiliated Hospital of University of South China, Hengyang, Hunan 421001, China
3Institute of Medical Imaging, University of South China, Hengyang, Hunan 421001, China
4Cancer Center, Faculty of Health Sciences, Centre for Cognitive and Brain Sciences, University of Macau, Macau SAR 999078, China
*Correspondence to: Zhiyi Chen, E-mail: zhiyi_chen@usc.edu.cn
Received: July 3 2020; Revised: August 3 2020; Accepted: September 21 2020; Published Online: June 12 2021
Cite this paper:
Yuhao Chen, Yue Li, Meng Du, Jinsui Yu, Fei Gao, Zhen Yuan and Zhiyi Chen. Ultrasound Neuromodulation: Integrating Medicine and Engineering for Neurological Disease Treatment. BIO Integration 2021; 2(4): 169–179.
DOI: 10.15212/bioi-2020-0026. Available at: https://bio-integration.org/
Download citation
© 2021 The Authors. This is an open access article distributed under the terms of the Creative Commons Attribution License (https://creativecommons.org/licenses/by/4.0/). See https://bio-integration.org/copyright-and-permissions/
Abstract
Neurological diseases associated with dysfunctions of neural circuits, including Alzheimer’s disease (AD), depression and epilepsy, have been increasingly prevalent. To tackle these issues, artificial stimulation or regulation of specific neural circuits and nuclei are employed to alleviate or cure certain neurological diseases. In particular, ultrasound neuromodulation has been an emerging interdisciplinary approach, which integrates medicine and engineering methodologies in the treatment. With the development of medicine and engineering, ultrasound neuromodulation has gradually been applied in the treatment of central nervous system diseases. In this review, we aimed to summarize the mechanism of ultrasound neuromodulation and the advances of focused ultrasound (FUS) in neuromodulation in recent years, with a special emphasis on its application in central nervous system disease treatment. FUS showed great feasibility in the treatment of epilepsy, tremor, AD, depression, and brain trauma. We also suggested future directions of ultrasound neuromodulation in clinical settings, with a focus on its fusion with genetic engineering or nanotechnology.
Keywords
Nanogenerator, neuromodulation, neurological disease, sonogenetics, ultrasound.
Introduction
Neurological diseases, such as Alzheimer’s disease (AD), depression, and epilepsy, are becoming increasingly common due to the rapidly increasing number of aging populations. Although millions of people are affected by neurological diseases, effective treatment measures are still far from adequate [1]. First, the currently preferred treatment for most central nervous system disease is drug therapy, but it is difficult for drugs to reach the therapeutic concentration in the brain due to the blood–brain barrier [2]. Second, even though surgical treatment could effectively alleviate the symptoms of neurological diseases such as tremor and Parkinson’s disease, thus somehow improving patients’ life quality [3], craniotomy may leave some sequelae, including intracranial hemorrhage, memory decline, and traumatic epilepsy. Moreover, gene therapy can alter gene mutation sites in neurological diseases through adeno-associated virus delivery, but the use of viral vectors still carries the risk of immune stimulation [4] (Table 1). Therefore, it is crucial to find a non-invasive, reversible, and controllable treatment method for neurological diseases.
Table 1 Current Treatment Methods for Neurological Diseases
| Treatment | Advantages | Disadvantages | Treatment of Neurological Diseases |
|---|---|---|---|
| Drug therapy | Simplicity, efficiency | Drug resistance | Epilepsy [5], tremor [6], Alzheimer’s disease [7], depression [8], Parkinson’s disease [9] |
| Surgery | Effectiveness | Invasiveness | Tremor [10], brain trauma [11], Parkinson’s disease [3] |
| Gene therapy | Durability | Bio-safety | Parkinson’s disease [12], Alzheimer’s disease [13] |
| Neuromodulation | Controllability, targeting | Unclear treatment mechanism for now | Epilepsy [14], tremor [15], Alzheimer’s disease [16], depression [17] |
Alternatively, the combination of medicine and engineering implicates a novel direction for the treatment of neurological diseases, namely neuromodulation [18, 19]. Neuromodulation refers to the artificial and controllable regulation of specific neuronal excitability and neural circuit conduction through physical methods, which is based on the combination of neuromedicine and physical engineering [20]. In some neurological diseases, the dysfunction of neural circuits results in impaired cognitive, sensory, or motor function [1]. Drawing on advanced and customized equipment, doctors applied electric, magnetic, optical, and acoustic modalities to accurately stimulate the specific neural circuits and brain nuclei to improve the function of the nervous system [21]. Currently available neuromodulation methods include deep brain stimulation, transcranial magnetic stimulation (TMS), optogenetics, and focused ultrasound (FUS) (Table 2). Deep brain stimulation, for example, by electrically stimulating neural circuits with electrodes implanted in brain tissue, has been used to alleviate tremor caused by Parkinson’s disease [22]. Neuromodulation has become one of the fastest developing disciplines in recent decade, and it has broad application prospects in the treatment of neurological diseases.
Table 2 Current Options of Neuromodulation Techniques
| Neuromodulation Technique | Principle | Limitations |
|---|---|---|
| Deep brain stimulation | Electrical stimulation through insertion of electrodes into brain tissue | It is invasive and requires surgical implantation of electrodes |
| Transcranial magnetic stimulation | A strong magnetic field is applied to the cerebral cortex, affecting neural electrical activity | Low focusing precision |
| Optogenetics | Light is used to activate photosensitive ion channels to excite nerve cells | Weak penetration depth Gene transfection is required |
| Focused ultrasound | The neurons’ excitability and neuro-microenvironment were changed by ultrasound irradiation | The biological consequences of ultrasound are complex, and the tissue around the ultrasound beam path might be damaged |
In particular, with the development of multi-element transducers and phased-array techniques, FUS energy can be non-invasively delivered to the targeted brain area through the human skull [23, 24]. Currently, FUS is applied as a new neuromodulation technique to reversibly stimulate or inhibit nervous system activity [25, 26]. Compared with other neuromodulation techniques, ultrasound neuromodulation has the advantages of penetration depth, non-invasiveness, imaging guidance, and precise spatial control [27]. Based on the interdisciplinary characteristics of ultrasound neuromodulation, the deep fusion of medicine and engineering is the core factor to promote the progress of ultrasound neuromodulation [28]. The continuous innovation of ultrasound transducers makes it possible to accurately stimulate the neural circuits in the human brain. The in-depth understanding of neurological diseases would encourage researchers to further explore the mechanisms of ultrasound neuromodulation.
The application of ultrasound neuromodulation in neurological disease treatment has manifested encouraging results and is still developing rapidly. Existing review work has surveyed the bio-physical mechanisms and safety issues of ultrasound neuromodulation [29, 30], but more empirical studies or systematic reviews are needed to provide a more comprehensive picture of applying ultrasound neuromodulation in neurological disease treatment. Therefore, the current review aimed to synthesize the research progress of ultrasound neuromodulation in the past 5 years, with special emphasis on its application in the treatment of various central nervous system diseases. We hope to present the latest advances in the field and also suggest potential areas for future research, focusing on the therapeutic effects of ultrasound neuromodulation for a variety of neurological disorders, including epilepsy, AD, and depression.
Mechanism of ultrasound neuromodulation
Effect of mechanical force
Acoustic radiation force is the mechanical force of ultrasound acting on the interface of substance. As shown in Figure 1B, given proper ultrasound intensities, acoustic radiation force stretches and distorts cytomembranes and then changes their geometric shape and mechanical properties [31]. Conformational recombination of phospholipid layers and proteins on the cell membrane leads to changes in membrane capacitance, affecting cell potential and hyperpolarization [32]. Chen et al. recently demonstrated that high-frequency oscillations could induce action potential through direct deflection effects at weak displacement amplitudes [33].
Figure 1 Mechanical effect of ultrasound neuromodulation in neuron. (A) Ion channels on the neuron membrane are closed in the resting state. (B) Focused ultrasound directly applies acoustic radiation to the ion channel protein and induces its opening. (C) Cavitation effect produced by ultrasound combined with microbubbles could also induce the opening of ion channels. (D) Ultrasound mechanical effect is capable of causing lipid membrane deformation and promotes the opening of ion channels through intramural cavitation, which in turn induces calcium influx and nerve impulses.
Ultrasound stimulation can lead to physical pores on the lipid bilayer membrane, resulting in an increase in the capacitance of the lipid membrane, in a process known as sonoporation [34]. The most prominent hypothetical mechanism for driving sonoporation is the cavitation effect. Stable cavitation generates microjets, shock waves, and acoustic streaming to stimulate mechanosensitive ion channels and receptors of surrounding nerve cells [35]. Cell potential and hyperpolarization states are also altered by changes in fluidity, permeability, and conductance of the cell membrane [36] (Figure 1C). In addition to the cavitation effect caused by extracellular microbubbles, intramembrane cavitation can also lead to neuronal depolarization [37]. Ultrasound mechanical energy is transformed into periodic expansions and contractions of the bilayer membrane space and induces intramembrane cavitation (bubble formation) (Figure 1D). Formation and collapse of nanobubbles in the membrane space could change the local curvature of bilayers and affect the capacitance, fluidity, and permeability of lipid bilayers. Intramembrane cavitation is considered to be another mechanism of the neuronal electrical discharge stimulated by cavitation in the absence of gas [38].
Thermal effect
When ultrasonic waves propagate through the medium, some of the acoustic energy is transformed into thermal energy which increases the temperature of the medium [39]. The thermal effects of high-intensity FUS can cause cell protein degeneration, DNA fragment rupture, and tissue coagulation necrosis [40]. At lower ultrasonic intensities, local heat generates moderate effects including decreased action potential amplitude, changes in ion channel dynamics, suppressed neural signaling, and reversible conduction block [41, 42]. Furthermore, the thermal effect of FUS has the ability to enhance the neurotrophic factor delivery through the increased blood perfusion and permeability of the blood–brain barrier [43].
Neurotrophic factor manipulation
Neurotrophic factors are polypeptides or protein factors that can promote the survival, growth, and differentiation of nerve cells [44]. Ultrasound can promote the secretion, release, and delivery of neurotrophic factors. Yang et al. found that neurotrophic factors, such as brain-derived neurotrophic factor (BDNF), glial cell-derived neurotrophic factor (GDNF), and vascular endothelial growth factor, were increased after stimulation of integrin receptors by low-intensity ultrasound [43]. The expressions of BDNF and GDNF in the ultrasound-irradiated cerebral hemispheres (Ispta=110 mW/cm2) were significantly higher than that in unirradiated hemispheres. Moreover, FUS (30–50 mW/cm2) could also improve the bio-activity of nerve growth factor and promote neurite outgrowth through the mechanotransduction-mediated ERK1/2 CREB Trx-1 pathway [45]. Ultrasound can increase the local concentration of neurotrophic factors by activating signaling pathways, which is beneficial for most neurological diseases.
Neurological disease treatment
Epilepsy
Epilepsy is a chronic disorder of the brain, which is characterized by an enduring predisposition to the generation of epileptic seizures [46]. Although more than 20 drugs have been developed to treat epilepsy, more than one-third of patients reported null response to any drug, known as drug-resistant epilepsy [47]. For these patients, neuromodulation might an alternative therapy to reduce the incidence of abnormal epileptic discharges [48]. Ultrasound neuromodulation techniques have gained widespread attention due to their therapeutic utility in nervous impulse suppression. In chemically induced animal models, ultrasound stimulation–induced cortical excitability diminution has been shown to attenuate epileptic activity [49]. Hakimova et al. found that pulsed ultrasound stimulation could effectively suppress seizures in mice with epilepsy in the temporal lobe. Ultrasound-treated mice exhibited fewer spontaneous recurrent seizures in the chronic period of epilepsy [50]. Chen et al. investigated the parametric selection of ultrasound exposure that provided epilepsy suppression. The EEG signals in ultrasound-treated groups showed a significant decrease in the number of spikes compared with the control groups [51]. FUS exposure for 600 seconds with a mechanical index of 0.75 provided an effective spike-suppressing effect. The downstream target of the mTOR pathway in the cortex and hippocampus of rats was suppressed by FUS treatment. Therefore, the aforementioned studies provided solid evidence that FUS pulsation could serve as an effective and non-invasive therapeutic tool to suppress epileptic activity, which implicates great potential for clinical use.
Tremor
Tremor is characterized by the involuntary, rhythmic, and sinusoidal alternation of body parts [52]. Particularly, essential tremor (ET) is a common nervous system disease characterized by tremor in clinical practice and affects approximately 1% of the population worldwide [53]. In a multi-institution clinical trial, 76 patients with moderate to severe medication-refractory ET were randomized to undergo FUS thalamotomy or a sham therapy, which did not provide ultrasonic energy. After 3 months of treatment, it was found that, compared with sham surgery, patients completing FUS thalamotomy significantly reduced hand tremor and improved their quality of life [52]. Sharabi et al. explored the feasibility of using non-thermal FUS to suppress ET in rats [54]. FUS was used to irradiate the olivary system, and the tremor frequency in ET rats was significantly reduced. The tremor was completely inhibited in half of the animals. Meanwhile, magnetic resonance imaging (MRI) after treatment detected no signs of nerve damage in the brain. FUS continues to advance and demonstrate its efficacy in the treatment of neurological diseases and may become a novel intervention against brain pathology. As a promising alternative to deep brain stimulation, ultrasound neuromodulation provides a broad spectrum of minimally invasive treatment with high specificity for diseases that are refractory to surgery.
Alzheimer’s disease
With the increase of aging population, neurodegenerative disease is reaching epidemic proportions. Dementia is a common neurodegenerative disease with approximately 44 million people worldwide suffering from it. Among the various causes of dementia, AD explains the biggest portion, accounting for approximately 50% to 75% [55]. Current drugs for AD target cholinergic and glutamine neurotransmitters, but their neuroprotective activity remains controversial [56]. Ultrasound neuromodulation is capable of stimulating neural circuits in the brain and increasing the secretion of endogenous neurotrophic factor [57, 58], which is expected to be used in novel treatments for neurodegenerative diseases. FUS has become a prospective treatment in mitigating brain injury, dysmnesia, and cognitive dysfunctions induced by cerebral disease [59]. Lin et al. examined the protective effect of FUS on brain injury induced by aluminum in AD rats [60]. FUS (Ispta=528 mW/cm2) reduced aluminum concentration, acetylcholine esterase activity, and amyloid protein β (Aβ) deposition, while promoting increased production of neurotrophic factor in brain tissues. BDNFs are effective mediators of neural plasticity in the hippocampus, which is significantly associated with the pathogenesis of AD [61]. Burgess et al. continuously stimulated the bilateral hippocampal bodies of AD mice using FUS (pressure=1.25 MPa). The number of new neurons in the hippocampus after treatment increased by more than 250%, and these neurons exhibited longer dendrites and branches [62]. At the same time, it was also demonstrated that the spatial learning in AD model mice was improved by Y-maze analysis.
Importantly, FUS not only improves the effectiveness of AD treatment by increasing neurotrophic factors but can also be used directly as physiotherapy for AD [63]. The main pathological features of AD are amyloid plaques and neurofibrillary tangles (NFTs). Leinenga and Goetz treated AD with repeated scanning ultrasound (pressure=0.7 MPa) independently and found that Aβ plaques were cleared in 75% of the ultrasound-treated mice [64]. The mobility and cognitive ability of the mice whose Aβ plaques were nearly removed showed improved performance. Changes in mouse behavior were correlated to the decline in Aβ plaques as well as the increase in plasticity in the dentate gyrus. Pandit et al. investigated the effects of ultrasound treatments in K3 mouse models that harbor the K369I mutation of tau, presenting with prevalent NFTs in the cortex and hippocampus [65]. The results showed that repeated ultrasound treatment resulted in a two-fold reduction in tau phosphorylation and NFTs, especially in the hippocampus. After sonication, the MTOR activity (p-mTOR/mTOR) was significantly decreased, and the number of p62-positive spots were increased, suggesting that ultrasonic processing could inhibit AD by increasing the autophagy activity of neurons.
To sum up, accumulating therapies that targeted various aspects of AD have achieved significant clinical developments. Ultrasound could produce therapeutic effects in AD through different mechanisms, including activation of microglial cells to clear Aβ, and enhancement of tau clearance through autophagy.
Depression
Depression is a common and recurrent mood disorder in the modern society. Despite the significant increase in anti-depressant medications, many patients are still suffering from inadequate drug therapy [66]. Promoting BDNF could alleviate symptoms of depression, as BDNF plays an important role in its pathogenesis [67]. It has been proposed that FUS could be effective in the treatment of depression because it regulates the concentration of BDNF in the brain [57].
Zhang et al. used FUS to stimulate the prelimbic cortex of restrained rats for 2 weeks [68]. They found that it provided relief of depressive symptoms such as reversed anhedonia and reduced exploratory behavior. BDNF in the ipsilateral brain was significantly promoted in the FUS group, protecting neurons against restraint stress and facilitating neurogenesis in the hippocampus. Previously, BDNF has been shown to be involved in neurogenic regulation of the hippocampus and decreased hippocampal neurogenesis is also associated with depression. Studies have shown that transcranial ultrasound could promote hippocampal neurogenesis [69], but its bio-physical mechanism is still poorly understood. Therefore, the effect of transcranial ultrasound on neurogenesis merits further investigations to elucidate its mechanism in the treatment of depression.
In addition to being associated with increased BDNF expression, the therapeutic effect of ultrasound also inhibits the oxidative stress injury response that is toxic to neurons. Zhao et al. found that FUS (50 mW/cm2) could induce the activation of K2P channels, stretch-activate ion channels, and ultimately modulate the PI3K-Akt and ERK1/2 signaling pathways to prevent cytotoxicity of 1-methyl-4-phenylpyridinium (MPP+)-induced oxidative stress. Their results showed that activation of mechanosensitive ion channels might be a mechanism of the neuroprotective effect of FUS [70]. Thus, FUS has the potential to be a non-invasive antidepressant treatment tool. FUS therapy is expected to address the drawbacks of current physical therapy, such as inadequate response, serious side effects, and major surgical hazards.
Brain trauma
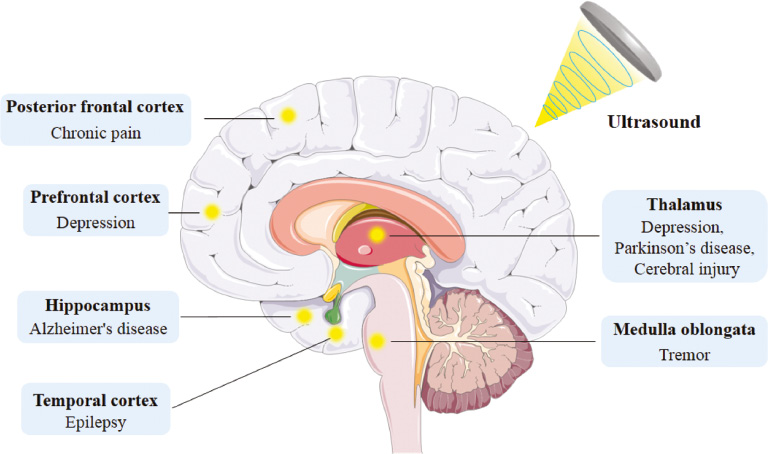
Brain trauma causes different degrees of neurological dysfunction. The symptoms of neurological dysfunction are determined by the damaged brain area. Local brain trauma can lead to motor, verbal, visual, and auditory abnormalities, whereas diffuse brain trauma could result in consciousness confusion and coma. In the clinic, brain stimulation has demonstrated the eligibility to enhance the behavioral responsiveness of disorder of consciousness (DOC) patients, which could increase the excitability of thalamic efferent neurons. Monti et al. applied FUS (720 mW/cm2) to stimulate the intact thalamus of a comatose brain trauma patient. After sonication, the patient exhibited improved behaviors in motor function, understanding, and communication abilities without evident harmful reactions. Five days after the sonication, the patient demonstrated walking ability [71]. Currently, a clinical trial explored the role of low-intensity FUS in patients with acute brain injury [72, 73]. Treatment of neurological diseases by FUS is in its infancy, but this study substantiated the therapeutic effect of ultrasound neuromodulation in patients, which was informative for future examinations on the application of ultrasound in the treatment of clinical diseases. The currently identified therapeutic targets for central nervous system disease are summarized in Figure 2.
Figure 2 Schematic diagram of ultrasound neuromodulation targets in neurological disease treatment. Ultrasound could be used to stimulate different areas of the human brain, including the thalamus, medulla oblongata, and temporal lobe. According to the types of neurological diseases, the appropriate targets of ultrasound neuromodulation can be selected to achieve the treatment of several different neurological diseases, including Alzheimer’s disease, depression, epilepsy, and tremor.
New directions of ultrasound neuromodulation
Sonogenetics
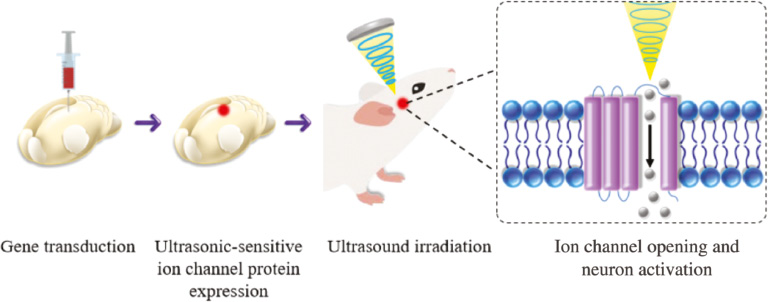
Ultrasound has the ability to transfer energy to the targeted area with millimeter precision and exert mechanical forces on the tissue to control mechanical signaling. However, with the development of molecular biology and precision medicine, millimeter-level nerve stimulation relying on focusing probes cannot meet the practical requirements. To improve the specificity of ultrasonic neuromodulation, the term “sonogenetics” was first proposed in 2015 [74]. Sonogenetics is a promising research field that sensitizes the neuron’s response to ultrasound by superficial expression of mechanical-sensitive ion channels. Similar to optogenetics and magnetogenetics, sonogenetics uses gene-engineering technology to transduce the gene’s encoding ultrasonic-sensitive ion channel proteins into targeted neurons [74]. Then, ultrasonic stimulation is applied to mechanically deform channel proteins, thus activating the ion channel and inducing action potentials of neurons that underwent gene editing (Figure 3).
Figure 3 Schematic diagram of in vivo application of sonogenetics. First, the gene encoding ultrasonic-sensitive ion channel proteins was transduced to the target brain tissue, and the nerve cells in the target brain region are encouraged to express ion channel proteins in response to ultrasound. Then, ultrasound irradiation could activate ion channels, increase calcium ion influx, and then achieve neuronal excitation. Nerve cells that did not receive gene transfer were not excited by ultrasound irradiation.
The TRP-4 channel is responsive to mechanical signals, including ultrasound [72]. Ibsen et al. reported that the stimulation of Caenorhabditis elegans expressing TRP-4 using low-frequency (2.25 MHz) and low-pressure FUS (0.9 MPa) modulated neuronal activities and led to a subsequent escape response in C. elegans. The addition of microbubbles in this study amplified the mechanical effect of ultrasound on C. elegans. The results demonstrated that the combination of the genome-editing technique and ultrasound is available for the modulation of target neurons with high efficiency in organisms [74]. To further lay the foundation of sonogenetics, Ye et al. engineered the hippocampal CA1/CA3 neurons with a variant (I92L) of the mechanosensitive channel of large conductance that increased mechanosensitivity and evaluated its response to ultrasonic stimulation [75]. This study demonstrated that the introduction of I92L indeed conferred ultrasound sensitivity to neurons. The mutant expressing I92L could generate a depolarizing current of 4 pA/pF without microbubbles under ultrasound stimulation with a pressure of 0.25 MPa. Neurons expressing I92L could elicit spike trains induced by ultrasound with a time precision of milliseconds. However, the high frequency of ultrasound used in these studies resulted in low penetration, which is not suitable for applications in vivo. Huang et al. developed a method to remotely control transgenic neurons using low-frequency and low-acoustic pressure FUS based on the auditory sensing protein prestin from mammalian outer hair cells [76]. They found that low-frequency ultrasound (0.5 MHz) could effectively induce calcium flow in cells transfected with mutant prestin. Further, the researchers injected an adeno-associated virus encoding mutant prestin into the unilateral ventral tegmental area of mouse. The nerve excitation in unilateral hemispheres of the transfected mice expressing prestin were triggered by ultrasound, whereas the contralateral brain regions that did not express prestin were not activated. These results confirmed that low-frequency ultrasound could specifically activate neurons expressing the mutant prestin to achieve noninvasive and precise neural cell activity manipulation.
In addition to specific neuromodulation, sonogenetics could also be harnessed to regulate the signal pathways mediated by mechanical signals to achieve temporospatial control of cellular processes in disease therapy. In recent studies, to increase the spatiotemporal precision of CAR-T activation, Pan et al. transduced the T-cell-expressed Piezo 1 ion channel into CAR-T, mediated by ultrasound, to improve the targeting ability of CAR-T immunotherapy against malignant tumor tissues [77]. This method allowed remote, non-invasive, and accurate control of gene expression as well as guidance of polytype cancer treatment.
Sonogenetics enables the specific stimulation of individual neurons at the cellular level and can be used as a highly targeted and noninvasive neuromodulation method in fundamental neuroscience research. However, the clinical translation of sonogenetics relies on the identification of more acoustically responsive ion channels, which are not expressed in the mammalian brain. Moreover, only when genetic engineering of human neurons are performed reliably and safely could sonogenetics be pervasively applied in clinical trials.
Nanogenerator support
Safety is still the crucial concern to the application of ultrasound neuromodulation in the human brain. The biological outcome of ultrasound-mediated neuromodulation is excessively affected by different combinations of ultrasound parameters, including intensity, frequency, and pulse length [78]. A higher intensity or longer exposure time may cause nerves to suffer from hyperthermia and cavitation from sonication [79, 80]. To reduce the output power of ultrasound and prevent damage to healthy tissue during neuromodulation, a secondary reinforcement can be applied to improve the neural stimulation ability of FUS.
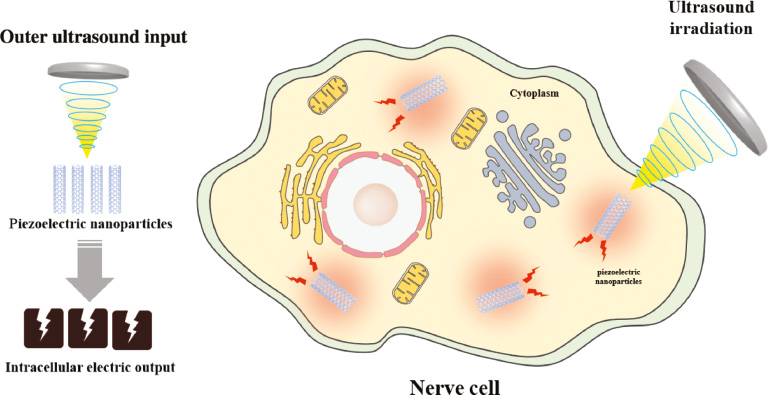
Nanogenerators are a prospective method to strengthen the local effect of FUS [81, 82]. They can effectively generate electricity in biofluids driven by ultrasonic stimulation via the piezoelectric properties of nanomaterials [83] (Figure 4). Drawing on characteristic of acoustoelectric conversion, piezoelectric nanomaterials can be used as nanogenerators to efficiently transform received ultrasonic energy into electricity and induce stable stimulation of neurons.
Figure 4 Schematic diagram of ultrasound combined with piezoelectric nanoparticles for targeting neural modulation. The mechanical effect of ultrasound can induce piezoelectric effect of piezoelectric nanoparticles and generate local electric field. Piezoelectric nanoparticles could be endocytized by nerve cells. Ultrasound irradiation stimulates the piezoelectric nanoparticles in nerve cells to generate electricity and induces the excitation of nerve cells.
To date, multiple preclinical studies detailing the application of piezoelectric nanomaterials on neural tissues in vitro have been published. As a piezoelectric material with good biocompatibility, boron nitride nanotubes (BNNT) can be polarized under ultrasonic mechanical stress and transduce electric stimuli to cells. Ciofani et al. found that after treatment with BNNT and ultrasound, neuronal-like PC12 cells produced 30% more axons than controls with increased Ca2+ influx. The results demonstrated that acoustoelectric transduction could facilitate neural stimulation by the indirect effects from low-intensity ultrasound [84].
To explore the underlying mechanism of ultrasound-mediated piezoelectric nanomaterial treatment in promoting neuronal cell growth and differentiation, Marino et al. successfully induced calcium and sodium influx in neuron-like cells using cubic barium titanate nanoparticles (BTNP) under ultrasound [85]. It was hypothesized that the activation of the voltage-gated ion channels was induced by a localized electric field produced from the process of acoustoelectric transduction from ultrasound stimulation. Ca2+ transients and axon elongation of SH-SY5Y cells cultured on the P(VDF-TrFE)/BTNP films were induced by ultrasound irradiation, suggesting that the piezoelectric effect directly mediated by polymer/ceramic composite films and ultrasound could be used for neuron stimulation [86]. In parallel, Rojas et al. confirmed that the combination of pulsed ultrasound and BTNP enhanced the mixed spiking and bursting electrophysiological activities in neurons by using microelectrode arrays [87]. The modified F-ratio of the neurons was linearly correlated with the strength of the pressure field, suggesting that neural activity could be altered by fine-tuning the amplitude of ultrasound waves.
Piezoelectric nanoparticles are expected to be highly specific, effective, and remote electrical stimulation tools in vivo through mechanical deformation by ultrasound stimulation [88]. However, extensive studies of the biocompatibility, biodistribution, and durability of these novel nanomaterials are needed to mitigate the security issue in vivo. Future research could focus on the targeted properties of piezoelectric nanomaterials to enable selective binding of neurons to achieve specific neuromodulation. Ultrasound targeted microbubble destruction (UTMD) technology is a non-invasive approach that can achieve targeted delivery by modifying microbubbles with antibodies or ligands [89]. Piezoelectric nanomaterials can be loaded into the microbubbles attached to specific ligands and delivered to targeted neurons. Furthermore, the effect of UTMD on enhancing membrane permeability can further promote the entry of nanoparticles into cells [90, 91]; thus, UTMD technology combined with piezoelectric nanomaterials is expected to be a new prospect in ultrasound neuromodulation research.
Outlook
Recent studies have demonstrated that ultrasound not only exerts neuromodulation on cortical brain regions [41, 92], but also non-invasively stimulates deep brain regions, such as the hippocampus and thalamus [93]. The functional regulation of deep brain tissue has significant implications for the treatment of nervous system diseases. There are few studies on ultrasound neuromodulation in the treatment of neurological diseases that have registered clinical trials. Hameroff et al. reported the therapeutic efficacy of ultrasound in patients with chronic pain [94], which could provoke more applications in related fields. After ultrasound stimulation of the posterior frontal cortex, the subjective mood of patient was improved. Ultrasound neuromodulation is therefore expected to provide a novel treatment approach for the neurofunctional diseases. In light of the recent developments and limitations of ultrasound neuromodulation in clinical trials, we suggested the following outstanding questions for future investigations of neuromedicine and engineering:
- For medicine, the exact biophysical mechanisms underlying the therapeutic effect of ultrasound neuromodulation remain to be elucidated. At present, most ultrasound neuromodulation research are limited to the observation of surface phenomena, but there is no in-depth study on the signal pathway mechanism, ultrasonic-electric interaction, or its influence on neuronal activity.
- With respect to the treatment mechanism, it is necessary to further optimize ultrasonic parameters according to the characteristics of different neurological diseases. In the future, more studies should be carried out to explore the neural network mechanism of ultrasound neuromodulation to identify the therapeutic targets for various neurological diseases.
- In terms of instrument engineering, it would be important to promote the development and industrialization of ultrasound neuromodulation instruments through close communication between doctors and engineers. The combination of ultrasound neuromodulation and neuroimaging technology such as fiber bundle tracking and electrophysiological signal analysis should be promoted to achieve precise image-guided neuromodulation.
- From a lens of interdisciplinary integration, the application scope of ultrasound neuromodulation for diseases still needs to be expanded. A combination of various therapeutic means, such as fusing ultrasound neuromodulation and nanotechnology, should be adopted to promote the clinical application of ultrasound neuromodulation. Ultimately, the goal is to apply the technology to clinical treatment.
Conclusion
As a combination of medicine and engineering, ultrasound neuromodulation has been proposed for the treatment of different central nervous diseases. Accumulating evidence manifested that ultrasound neuromodulation has great potentials as an innovative treatment against neurological diseases. Based on the development of ultrasonic transducers, ultrasound neuromodulation become a non-invasive therapy with high spatial precision and fewer side effects. We believe that, with the development of interdisciplinary investigation of neuromedicine, biological engineering, ultrasound, nanotechnology, and molecular biology, ultrasound neuromodulation will play a greater role in the treatment of neurological diseases in the near future.
Conflict of interest
The authors declare that they have no conflicts of interest.
Acknowledgments
This work was supported by the National Key R&D Program of China (2019YFE0110400), National Natural Science Foundation of China (no. 81971621), and Natural Science Foundation of Guangdong Province (no. 2019A1515012212).
References
- Goldberg EM, Coulter DA. Mechanisms of epileptogenesis: a convergence on neural circuit dysfunction. Nat Rev Neurosci 2013;14:337-49. [PMID: 23595016 DOI: 10.1038/nrn3482]
- Hashimoto Y, Tachibana K, Kondoh M. Tight junction modulators for drug delivery to the central nervous system. Drug Discov Today 2020;25:1477-86. [PMID: 32439607 DOI: 10.1016/j.drudis.2020.05.007]
- Armstrong MJ, Okun MS. Diagnosis and treatment of Parkinson disease: a review. J Am Med Assoc 2020;323:548-60. [PMID: 32044947 DOI: 10.1001/jama.2019.22360]
- Richardson RM, Bankiewicz KS, Christine CW, Van Laar AD, Gross RE, et al. Data-driven evolution of neurosurgical gene therapy delivery in Parkinson’s disease. J Neurol Neurosurg Psychiatry 2020;91:1210-8. [PMID: 32732384 DOI: 10.1136/jnnp-2020-322904]
- Koneval Z, Knox KM, Memon A, Zierath DK, White HS, et al. Antiseizure drug efficacy and tolerability in established and novel drug discovery seizure models in outbred vs inbred mice. Epilepsia 2020;61:2022-34. [PMID: 32757210 DOI: 10.1111/epi.16624]
- Bruno E, Nicoletti A, Filippini G, Quattrocchi G, Colosimo C, et al. Zonisamide for essential tremor. Cochrane Database Syst Rev 2017;8:CD009684. [PMID: 28836659 DOI: 10.1002/14651858.CD009684.pub2]
- Smaga I, Fierro D, Mesa J, Filip M, Knackstedt LA. Molecular changes evoked by the beta-lactam antibiotic ceftriaxone across rodent models of substance use disorder and neurological disease. Neurosci Biobehav Rev 2020;115:116-30. [PMID: 32485268 DOI: 10.1016/j.neubiorev.2020.05.016]
- Bresnahan R, Gianatsi M, Maguire MJ, Tudur Smith C, Marson AG. Vigabatrin add-on therapy for drug-resistant focal epilepsy. Cochrane Database Syst Rev 2020;7:CD007302. [PMID: 32730657 DOI: 10.1002/14651858.CD007302.pub3]
- de Bie RMA, Clarke CE, Espay AJ, Fox SH, Lang AE. Initiation of pharmacological therapy in Parkinson’s disease: when, why, and how. Lancet Neurol 2020;19:452-61. [PMID: 32171387 DOI: 10.1016/S1474-4422(20)30036-3]
- Elble RJ, Shih L, Cozzens JW. Surgical treatments for essential tremor. Expert Rev Neurother 2018;18:303-21. [PMID: 29475371 DOI: 10.1080/14737175.2018.1445526]
- Hirschi R, Hawryluk G. Treatment thresholds in neurotrauma. World Neurosurg 2020;134:654-5. [PMID: 32059269 DOI: 10.1016/j.wneu.2019.12.040]
- Titze-de-Almeida SS, Soto-Sanchez C, Fernandez E, Koprich JB, Brotchie JM, et al. The thresholds in neurotrauma miRNA-based therapeutics for Parkinson’s disease. Cells 2020;9:841. [PMID: 32244357 DOI: 10.3390/cells9040841]
- Yamazaki Y, Zhao N, Caulfield TR, Liu C-C, Bu G. Apolipoprotein E and Alzheimer disease: pathobiology and targeting strategies. Nat Rev Neurol 2019;15:501-18. [PMID: 31367008 DOI: 10.1038/s41582-019-0228-7]
- Davis P, Gaitanis J. Neuromodulation for the treatment of epilepsy: a review of current approaches and future directions. Clin Ther 2020;42:1140-54. [PMID: 32620340 DOI: 10.1016/j.clinthera.2020.05.017]
- Neumann W-J, Turner RS, Blankertz B, Mitchell T, Kuehn AA, et al. Toward electrophysiology-based intelligent adaptive deep brain stimulation for movement disorders. Neurotherapeutics 2019;16:105-18. [PMID: 30607748 DOI: 10.1007/s13311-018-00705-0]
- Jafari Z, Kolb BE, Mohajerani MH. Neural oscillations and brain stimulation in Alzheimer’s disease. Prog Neurobiol 2020:101878. [PMID: 32615147 DOI: 10.1016/j.pneurobio.2020.101878]
- Hung Y-Y, Yang L-H, Stubbs B, Li D-J, Tseng P-T, et al. Efficacy and tolerability of deep transcranial magnetic stimulation for treatment-resistant depression: a systematic review and meta-analysis. Prog Neuropsychopharmacol Biol Psychiatry 2020;99:109850. [PMID: 31863873 DOI: 10.1016/j.pnpbp.2019.109850]
- Troccaz J, Dagnino G, Yang G-Z. Frontiers of medical robotics: from concept to systems to clinical translation. Annu Rev Biomed Eng 2019;21:193-218. [PMID: 30822100 DOI: 10.1146/annurev-bioeng-060418-052502]
- Brenan CJH. The center for integration of medicine and innovative technologies. IEEE Pulse 2011;2:59-62. [PMID: 21791403 DOI: 10.1109/MPUL.2011.941458]
- Tao X, Lee MS, Donnelly CR, Ji R-R. Neuromodulation, specialized proresolving mediators, and resolution of pain. Neurotherapeutics 2020;17:886-99. [PMID: 32696274 DOI: 10.1007/s13311-020-00892-9]
- Hao S, Tang B, Wu Z, Ure K, Sun Y, et al. Forniceal deep brain stimulation rescues hippocampal memory in Rett syndrome mice. Nature 2015;526:430-4. [PMID: 26469053 DOI: 10.1038/nature15694]
- Cagnan H, Denison T, McIntyre C, Brown P. Emerging technologies for improved deep brain stimulation. Nat Biotechnol 2019;37:1024-33. [PMID: 31477926 DOI: 10.1038/s41587-019-0244-6]
- Fry FJ, Ades HW, Fry WJ. Production of reversible changes in the central nervous system by ultrasound. Science 1958;127:83-4. [PMID: 13495483 DOI: 10.1126/science.127.3289.83]
- Li G, Qiu W, Hong J, Jiang Q, Su M, et al. Imaging- guided dual-target neuromodulation of the mouse brain using array ultrasound. IEEE Trans Ultrason Ferroelectr Freq Control 2018;65:1583-9. [PMID: 29994254 DOI: 10.1109/TUFFC.2018.2847252]
- Jiang Q, Li G, Zhao H, Sheng W, Yue L, et al. Temporal neuromodulation of retinal ganglion cells by low-frequency focused ultrasound stimulation. IEEE Trans Neural Syst Rehabil Eng 2018;26:969-76. [PMID: 29752231 DOI: 10.1109/TNSRE.2018.2821194]
- Kubanek J. Neuromodulation with transcranial focused ultrasound. Neurosurg Focus 2018;44:E14. [PMID: 29385924 DOI: 10.3171/2017.11.FOCUS17621]
- Landhuis E. Ultrasound for the brain. Nature 2017;551:257-9. [PMID: 32080485 DOI: 10.1038/d41586-017-05479-7]
- Fomenko A, Neudorfer C, Dallapiazza RF, Kalia SK, Lozano AM. Low-intensity ultrasound neuromodulation: an overview of mechanisms and emerging human applications. Brain Stimul 2018;11:1209-17. [PMID: 30166265 DOI: 10.1016/j.brs.2018.08.013]
- Blackmore J, Shrivastava S, Sallet J, Butler CR, Cleveland RO. Ultrasound neuromodulation: a review of results, mechanisms and safety. Ultrasound Med Biol 2019;45:1509-36. [PMID: 31109842 DOI: 10.1016/j.ultrasmedbio.2018.12.015]
- Pasquinelli C, Hanson LG, Siebner HR, Lee HJ, Thielscher A. Safety of transcranial focused ultrasound stimulation: a systematic review of the state of knowledge from both human and animal studies. Brain Stimul 2019;12:1367-80. [PMID: 31401074 DOI: 10.1016/j.brs.2019.07.024]
- Zhou W, Wang J, Wang K, Huang B, Niu L, et al. Ultrasound neuro-modulation chip: activation of sensory neurons in Caenorhabditis elegans by surface acoustic waves. Lab Chip 2017;17:1725-31. [PMID: 28447086 DOI: 10.1039/c7lc00163k]
- Heureaux J, Chen D, Murray VL, Deng CX, Liu AP. Activation of a bacterial mechanosensitive channel in mammalian cells by cytoskeletal stress. Cell Mol Bioeng 2014;7:307-19. [PMID: 25606062 DOI: 10.1007/s12195-014-0337-8]
- Chen H, Garcia-Gonzalez D, Jerusalem A. Computational model of the mechanoelectrophysiological coupling in axons with application to neuromodulation. Phys Rev E 2019;99:032406. [PMID: 30999419 DOI: 10.1103/PhysRevE.99.032406]
- Helfield B, Chen X, Watkins SC, Villanueva FS. Biophysical insight into mechanisms of sonoporation. Proc Natl Acad Scie U S A 2016;113:9983-8. [PMID: 27551081 DOI: 10.1073/pnas.1606915113]
- Wright CJ, Haqshenas SR, Rothwell J, Saffari N. Unmyelinated peripheral nerves can be stimulated in vitro using pulsed ultrasound. Ultrasound Med Biol 2017;43:2269-83. [PMID: 28716433 DOI: 10.1016/j.ultrasmedbio.2017.05.008]
- di Biase L, Falato E, Di Lazzaro V. Transcranial focused ultrasound (tFUS) and transcranial unfocused ultrasound (tUS) neuromodulation: from theoretical principles to stimulation practices. Front Neurol 2019;10:549. [PMID: 31244747 DOI: 10.3389/fneur.2019.00549]
- Krasovitski B, Frenkel V, Shoham S, Kimmel E. Intramembrane cavitation as a unifying mechanism for ultrasound-induced bioeffects. Proc Natl Acad Sci U S A 2011;108:3258-63. [PMID: 21300891 DOI: 10.1073/pnas.1015771108]
- Plaksin M, Shoham S, Kimmel E. Intramembrane cavitation as a predictive bio-piezoelectric mechanism for ultrasonic brain stimulation. Phys Rev X 2014;4:011004. [DOI: 10.1103/PhysRevX.4.011004]
- Li J, Suo Y, Liao X, Ahn J, Liu D, et al. Analysis of Staphylococcus aureus cell viability, sublethal injury and death induced by synergistic combination of ultrasound and mild heat. Ultrason Sonochem 2017;39:101-10. [PMID: 28732925 DOI: 10.1016/j.ultsonch.2017.04.019]
- Devarakonda SB, Myers MR, Lanier M, Dumoulin C, Banerjee RK. Assessment of gold nanoparticle-mediated-enhanced hyperthermia using MR-guided high-intensity focused ultrasound ablation procedure. Nano Lett 2017;17:2532-8. [PMID: 28287747 DOI: 10.1021/acs.nanolett.7b00272]
- King RL, Brown JR, Pauly KB. Localization of ultrasound-induced in vivo neurostimulation in the mouse model. Ultrasound Med Biol 2014;40:1512-22. [PMID: 24642220 DOI: 10.1016/j.ultrasmedbio.2014.01.020]
- Lee YF, Lin CC, Cheng JS, Chen GS. Nerve conduction block in diabetic rats using high-intensity focused ultrasound for analgesic applications. Br J Anaesth 2015;114:840-6. [PMID: 25904608 DOI: 10.1093/bja/aeu443]
- Yang F-Y, Lu W-W, Lin W-T, Chang C-W, Huang S-L. Enhancement of neurotrophic factors in astrocyte for neuroprotective effects in brain disorders using low-intensity pulsed ultrasound stimulation. Brain Stimul 2015;8:465-73. [PMID: 25558041 DOI: 10.1016/j.brs.2014.11.017]
- Ayanlaja AA, Zhang B, Ji G, Gao Y, Wang J, et al. The reversible effects of glial cell line-derived neurotrophic factor (GDNF) in the human brain. Semin Cancer Biol 2018;53:212-22. [PMID: 30059726 DOI: 10.1016/j.semcancer.2018.07.005]
- Zhao L, Feng Y, Hu H, Shi A, Zhang L, et al. Low-intensity pulsed ultrasound enhances nerve growth factor-induced neurite outgrowth through mechanotransduction-mediated ERK1/2-CREB-Trx-1 signaling. Ultrasound Med Biol 2016;42:2914-25. [PMID: 27592560 DOI: 10.1016/j.ultrasmedbio.2016.07.017]
- Thijs RD, Surges R, O’Brien TJ, Sander JW. Epilepsy in adults. Lancet 2019;393:689-701. [PMID: 30686584 DOI: 10.1016/S0140-6736(18)32596-0]
- Manford M. Recent advances in epilepsy. J Neurol 2017;264:1811-24. [PMID: 28120042 DOI: 10.1007/s00415-017-8394-2]
- Rolston JD, Deng H, Wang DD, Englot DJ, Chang EF. Multiple subpial transections for medically refractory epilepsy: a disaggregated review of patient-level data. Neurosurgery 2018;82:613-20. [PMID: 28637175 DOI: 10.1093/neuros/nyx311]
- Zhang Y, Zhou H, Qu H, Liao C, Jiang H, et al. Effects of non-invasive, targeted, neuronal lesions on seizures in a mouse model of temporal lobe epilepsy. Ultrasound Med Biol 2020;46:1224-34. [PMID: 32081583 DOI: 10.1016/j.ultrasmedbio.2020.01.008]
- Hakimova H, Kim S, Chu K, Lee SK, Jeong B, et al. Ultrasound stimulation inhibits recurrent seizures and improves behavioral outcome in an experimental model of mesial temporal lobe epilepsy. Epilepsy Behav 2015;49:26-32. [PMID: 25940106 DOI: 10.1016/j.yebeh.2015.04.008]
- Chen S-G, Tsai C-H, Lin C-J, Cheng-Chia L, Yu H-Y, et al. Transcranial focused ultrasound pulsation suppresses pentylenetetrazol induced epilepsy in vivo. Brain Stimul 2020;13:35-46. [PMID: 31575487 DOI: 10.1016/j.brs.2019.09.011]
- Elias WJ, Lipsman N, Ondo WG, Ghanouni P, Kim YG, et al. A randomized trial of focused ultrasound thalamotomy for essential tremor. N Engl J Med 2016;375:730-9. [PMID: 27557301 DOI: 10.1056/NEJMoa1600159]
- Haubenberger D, Hallett M. Essential tremor. N Engl J Med 2018;378:1802-10. [PMID: 29742376 DOI: 10.1056/NEJMcp1707928]
- Sharabi S, Daniels D, Last D, Guez D, Zivli Z, et al. Non-thermal focused ultrasound induced reversible reduction of essential tremor in a rat model. Brain Stimul 2019;12:1-8. [PMID: 30181107 DOI: 10.1016/j.brs.2018.08.014]
- Lane CA, Hardy J, Schott JM. Alzheimer’s disease. Eur J Neurol 2018;25:59-70. [PMID: 28872215 DOI: 10.1111/ene.13439]
- Mangialasche F, Solomon A, Winblad B, Mecocci P, Kivipelto M. Alzheimer’s disease: clinical trials and drug development. Lancet Neurol 2010;9:702-16. [PMID: 20610346 DOI: 10.1016/S1474-4422(10)70119-8]
- Tsai S-J. Transcranial focused ultrasound as a possible treatment for major depression. Med Hypotheses 2015;84:381-3. [PMID: 25665863 DOI: 10.1016/j.mehy.2015.01.030]
- Tufail Y, Matyushov A, Baldwin N, Tauchmann ML, Georges J, et al. Transcranial pulsed ultrasound stimulates intact brain circuits. Neuron 2010;66:681-94. [PMID: 20547127 DOI: 10.1016/j.neuron.2010.05.008]
- Ren C, Li J-M, Lin X. LIPUS enhance elongation of neurites in rat cortical neurons through inhibition of GSK-3 beta. Biomed Environ Sci 2010;23:244-9. [PMID: 20708505 DOI: 10.1016/S0895-3988(10)60059-1]
- Lin W-T, Chen R-C, Lu W-W, Liu S-H, Yang F-Y. Protective effects of low-intensity pulsed ultrasound on aluminum-induced cerebral damage in Alzheimer’s disease rat model. Sci Rep 2015;5 :9671. [PMID: 25873429 DOI: 10.1038/srep09671]
- Huang S, Tong H, Lei M, Zhou M, Guo W, et al. Astrocytic glutamatergic transporters are involved in A beta-induced synaptic dysfunction. Brain Res 2018;1678:129-37. [PMID: 29066369 DOI: 10.1016/j.brainres.2017.10.011]
- Burgess A, Dubey S, Yeung S, Hough O, Eterman N, et al. Alzheimer disease in a mouse model: MR imaging-guided focused ultrasound targeted to the hippocampus opens the blood-brain barrier and improves pathologic abnormalities and behavior. Radiology 2014;273:736-45. [PMID: 25222068 DOI: 10.1148/radiol.14140245]
- Meng Y, Volpini M, Black S, Lozano AM, Hynynen K, et al. Focused ultrasound as a novel strategy for Alzheimer disease therapeutics. Ann Neurol 2017;81:611-7. [PMID: 28395123 DOI: 10.1002/ana.24933]
- Leinenga G, Goetz J. Scanning ultrasound removes amyloid-beta and restores memory in an Alzheimer’s disease mouse model. Sci Transl Med 2015;7:278ra33. [PMID: 25761889 DOI: 10.1126/scitranslmed.aaa2512]
- Pandit R, Leinenga G, Gotz J. Repeated ultrasound treatment of tau transgenic mice clears neuronal tau by autophagy and improves behavioral functions. Theranostics 2019;9:3754-67. [PMID: 31281511 DOI: 10.7150/thno.34388]
- Coryell WH. Maintenance treatment for psychotic depressive disorders progress and remaining challenges. J Am Med Assoc 2019;322:615-7. [PMID: 31429877 DOI: 10.1001/jama.2019.9682]
- Koo JW, Chaudhury D, Han M-H, Nestler EJ. Role of mesolimbic brain-derived neurotrophic factor in depression. Biol Psychiatry 2019;86:738-48. [PMID: 31327473 DOI: 10.1016/j.biopsych.2019.05.020]
- Zhang D, Li H, Sun J, Hu W, Jin W, et al. Antidepressant-like effect of low-intensity transcranial ultrasound stimulation. IEEE Trans Biomed Eng 2019;66:411-20. [PMID: 29993461 DOI: 10.1109/TBME.2018.2845689]
- Scarcelli T, Jordao JF, O’Reilly MA, Ellens N, Hynynen K, et al. Stimulation of hippocampal neurogenesis by transcranial focused ultrasound and microbubbles in adult mice. Brain Stimul 2014;7:304-7. [PMID: 24629831 DOI: 10.1016/j.brs.2013.12.012]
- Zhao L, Feng Y, Shi A, Zhang L, Guo S, et al. Neuroprotective effect of low-intensity pulsed ultrasound against MPP+-induced neurotoxicity in PC12 channels and stretch-activated ion channels K2P channels and stretch-activated ion channels. Ultrasound Med Biol 2017;43:1986-99. [PMID: 28583325 DOI: 10.1016/j.ultrasmedbio.2017.04.020]
- Monti MM, Schnakers C, Korb AS, Bystritsky A, Vespa PM. Non- invasive ultrasonic thalamic stimulation in disorders of consciousness after severe brain injury: a first-in-man report. Brain Stimul 2016;9:940-1. [PMID: 27567470 DOI: 10.1016/j.brs.2016.07.008]
- Nagarajan A, Ning Y, Reisner K, Buraei Z, Larsen JP, et al. Progressive degeneration of dopaminergic neurons through TRP channel-induced cell death. J Neurosci 2014;34:5738-46. [PMID: 24760834 DOI: 10.1523/JNEUROSCI.4540-13.2014]
- Nct02522429. Thalamic low intensity focused ultrasound in acute brain injury (LIFUP). 2015. Available from: https://clinicaltrials.gov/ct2/show/NCT02522429?.
- Ibsen S, Tong A, Schutt C, Esener S, Chalasani SH. Sonogenetics is a non-invasive approach to activating neurons in Caenorhabditis elegans. Nat Commun 2015;6:8264. [PMID: 26372413 DOI: 10.1038/ncomms9264]
- Ye J, Tang S, Meng L, Li X, Wen X, et al. Ultrasonic control of neural activity through activation of the mechanosensitive channel MscL. Nano Lett 2018;18:4148-55. [PMID: 29916253 DOI: 10.1021/acs.nanolett.8b00935]
- Huang Y-S, Fan C-H, Hsu N, Chiu N-H, Wu C-Y, et al. Sonogenetic modulation of cellular activities using an engineered auditory-sensing protein. Nano Lett 2020;20:1089-100. [PMID: 31884787 DOI: 10.1021/acs.nanolett.9b04373]
- Pan Y, Yoon S, Sun J, Huang Z, Lee C, et al. Mechanogenetics for the remote and noninvasive control of cancer immunotherapy. Proc Nat Acad Sci U S A 2018;115:992-7. [PMID: 29343642 DOI: 10.1073/pnas.1714900115]
- Baek H, Pahk KJ, Kim H. A review of low-intensity focused ultrasound for neuromodulation. Biomed Eng Lett 2017;7:135-42. [PMID: 30603160 DOI: 10.1007/s13534-016-0007-y]
- Dalecki D. Mechanical bioeffects of ultrasound. Ann Rev Biomed Eng 2004;6:229-48. [PMID: 15255769 DOI: 10.1146/annurev.bioeng.6.040803.140126]
- Naor O, Krupa S, Shoham S. Ultrasonic neuromodulation. J Neural Eng 2016;13:031003. [PMID: 27153566 DOI: 10.1088/1741-2560/13/3/031003]
- Garcia-Lopez V, Chen F, Nilewski LG, Duret G, Aliyan A, et al. Molecular machines open cell membranes. Nature 2017;548:567-72. [PMID: 28858304 DOI: 10.1038/nature23657]
- Srivastava SK, Clergeaud G, Andresen TL, Boisen A. Micromotors for drug delivery in vivo: the road ahead. Adv Drug Deliv Rev. 2019;138:41-55. [PMID: 30236447 DOI: 10.1016/j.addr.2018.09.005]
- Lee B-S, Yoon J, Jung C, Kim DY, Jeon S-Y, et al. Silicon/carbon nanotube/BaTiO3 nanocomposite anode: evidence for enhanced lithium-ion mobility induced by the local piezoelectric potential. ACS Nano 2016;10:2617-27. [PMID: 26815662 DOI: 10.1021/acsnano.5b07674]
- Ciofani G, Danti S, D’Alessandro D, Ricotti L, Moscato S, et al. Enhancement of neurite outgrowth in neuronal-like cells following boron nitride nanotube-mediated stimulation. ACS Nano. 2010;4:6267-77. [PMID: 20925390 DOI: 10.1021/nn101985a]
- Marino A, Arai S, Hou Y, Sinibaldi E, Pellegrino M, et al. Piezoelectric nanoparticle-assisted wireless neuronal stimulation. ACS Nano. 2015;9:7678-89. [PMID: 26168074 DOI: 10.1021/acsnano.5b03162]
- Genchi GG, Ceseracciu L, Marino A, Labardi M, Marras S, et al. P(VDF-TrFE)/BaTiO3 nanoparticle composite films mediate piezoelectric stimulation and promote differentiation of SH-SY5Y neuroblastoma cells. Adv Healthc Mater. 2016;5:1808-20. [PMID: 27283784 DOI: 10.1002/adhm.201600245]
- Rojas C, Tedesco M, Massobrio P, Marino A, Ciofani G, et al. Acoustic stimulation can induce a selective neural network response mediated by piezoelectric nanoparticles. J Neural Eng 2018;15:036016. [PMID: 29235438 DOI: 10.1088/1741-2552/aaa140]
- Marino A, Battaglini M, De Pasquale D, Degl’Innocenti A, Ciofani G. Ultrasound-activated piezoelectric nanoparticles inhibit proliferation of breast cancer cells. Sci Rep. 2018;8:6257. [PMID: 29674690 DOI: 10.1038/s41598-018-24697-1]
- Yang C, Li Y, Du M, Chen Z. Recent advances in ultrasound-triggered therapy. J Drug Target. 2019;27:33-50. [PMID: 29659307 DOI: 10.1080/1061186X.2018.1464012]
- Airan RD, Meyer RA, Ellens NPK, Rhodes KR, Farahani K, et al. Noninvasive targeted transcranial neuromodulation via focused ultrasound gated drug release from nanoemulsions. Nano Lett. 2017;17:652-9. [PMID: 28094959 DOI: 10.1021/acs.nanolett.6b03517]
- Huang P, You X, Pan M, Li S, Zhang Y, et al. A novel therapeutic strategy using ultrasound mediated microbubbles destruction to treat colon cancer in a mouse model. Cancer Lett. 2013;335:183-90. [PMID: 23415737 DOI: 10.1016/j.canlet.2013.02.011]
- Kim H, Chiu A, Lee SD, Fischer K, Yon S-S. Focused ultrasound-mediated non-invasive brain stimulation: examination of sonication parameters. Brain Stimul. 2014;7:748-56. [PMID: 25088462 DOI: 10.1016/j.brs.2014.06.011]
- Baek H, Pahk KJ, Kim M-J, Youn I, Kim H. Modulation of cerebellar cortical plasticity using low-intensity focused ultrasound for poststroke sensorimotor function recovery. Neurorehabil Neural Repair 2018;32:777-87. [PMID: 30157709 DOI: 10.1177/1545968318790022]
- Hameroff S, Trakas M, Duffield C, Annabi E, Gerace MB, et al. Transcranial ultrasound (TUS) effects on mental states: a pilot study. Brain Stimul 2013;6:409-15. [PMID: 2266427 DOI: 10.1016/j.brs.2012.05.002]