New Roles for Clinicians in the Age of Artificial Intelligence
1Department of Ultrasound Medicine, Laboratory of Ultrasound Molecular Imaging, The Third Affiliated Hospital of Guangzhou Medical University of Guangzhou Medical University, The Liwan Hospital of the Third Affiliated Hospital of Guangzhou Medical University, Guangzhou, Guangdong 510000, China
*Correspondence to: Zhiyi Chen Tel: +86-020-81292115 E-mail: zhiyi_chen@gzhmu.edu.cn
Received: June 21 2020; Revised: July 23 2020; Accepted: August 24 2020; Published Online: September 17 2020
Cite this paper:
Fengyi Zeng, Xiaowen Liang and Zhiyi Chen. New Roles for Clinicians in the Age of Artificial Intelligence. BIO Integration 2020; 1(3): 113–117.
DOI: 10.15212/bioi-2020-0014. Available at: https://bio-integration.org/
Download citation
© 2020 The Authors. This is an open access article distributed under the terms of the Creative Commons Attribution License (https://creativecommons.org/licenses/by/4.0/). See https://bio-integration.org/copyright-and-permissions/
Abstract
With the rapid developments of digital picture processing, pattern recognition, and intelligent algorithms, artificial intelligence (AI) has been widely applied in the medical field. The applications of artificial intelligence in medicine (AIM) include diagnosis generation, therapy selection, healthcare management, disease stratification, etc. Among the applications, the focuses of AIM are assisting clinicians in implementing disease detection, quantitative measurement, and differential diagnosis to improve diagnostic accuracy and optimize treatment selection. Thus, researchers focus on creating and refining modeling processes, including the processes of data collection, data preprocessing, and data partitioning as well as how models are configured, evaluated, optimized, clinically applied, and used for training. However, there is little research on the consideration of clinicians in the age of AI. Meanwhile, AI is more accurate and spends less time in diagnosis between the competitions of AI and clinicians in some cases. Thus, AIM is gradually becoming a hot topic. Barely a day goes by without a claim that AI techniques are poised to replace most of today’s professionals. Despite huge promise surrounding this technology, AI alone cannot support all the requirements for precision medicine, rather AI should be used in cohesive collaboration with clinicians. However, the integration of AIM has created confusion among clinicians on their role in this era. Therefore, it is necessary to explore new roles for clinicians in the age of AI.
Statement of significance
With the advent of the era of AI, the integration of medical field and AI is on the rise. Medicine has undergone significant changes, and what was previously labor-intensive work is now being solved through intelligent means. This change has also raised concerns among scholars: Will doctors eventually be replaced by AI? From this perspective, this study elaborates on the reasons why AI cannot replace doctors, and points out how doctors should change their roles to accelerate the integration of these fields, so as to adapt to the developing times.
The current status of artificial intelligence in medicine
Artificial intelligence (AI) is bringing a paradigm shift to many fields, especially in healthcare [1, 2]. Since IBM first began attempting to develop healthcare applications for its “Watson” AI in 2015, AI has been gradually transformed from cutting-edge technology into accessible, practical technology integrating routine clinical applications with continuous developments in deep learning technologies [3]. Artificial intelligence in medicine (AIM) is similar to that used in regards to humans but in the medical domain, that aims at dealing with the maintenance of health and the prevention, alleviation, or cure of disease through knowledge- and/or data-intensive computer-based solutions. Current applications of AIM include diagnosis generation, therapy selection, healthcare management, disease stratification, etc. A number of encouraging results have been reported in AI-enabled computer-aided diagnosis surpassing human-level performance [4–7]. For example, an automated deep learning system was proposed based on digital X-ray to evaluate bone age and the results showed that the system has more accuracy in assessing bone age with a much faster interpretation (<2 s).
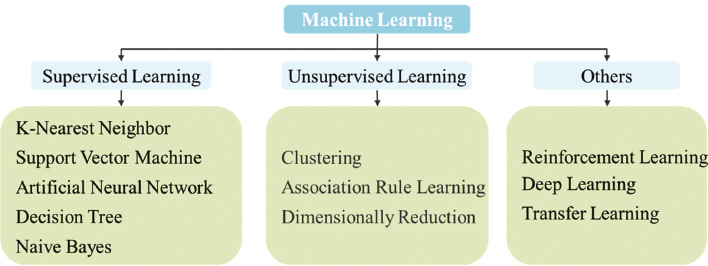
Machine learning is a branch of AI in which algorithms are most commonly used in clinical practice [8] (Figure 1). The potentials in clinical applications are in their abilities to analyze combinations of structured and unstructured data to generate clinical decision support. If these two kinds of data can be processed and fused, the clinician’s knowledge and experience are effectively fused with intelligent reasoning. Meanwhile, AI can achieve a diagnosis for patients through continuous collection, feedback, and modification. AI has great application value in generating a diagnosis. Besides, the advent of medical robots has given clinicians more options. Medical robots can be more precise, sophisticated, and flexible than clinicians. If a medical robot is combined with AI technology, some problems in the standardization, cost, time, and efficiency of surgery can be effectively solved.
Figure 1 The current methods of machine learning.
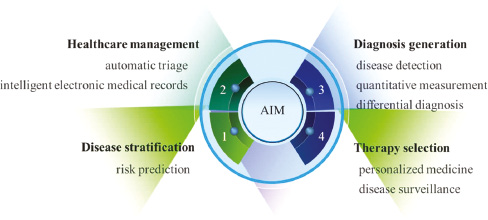
Being able to predict key outcomes could make the use of hospital palliative care resources more efficient and accurate. With the ability of big data processing, AI can mine the relationship between diseases and genes such that AI can predict the effectiveness of treatment programs for individuals. Additionally, AI can manage hospital health system to analyze the diagnosis and treatment programs for individuals more accurately. Therefore, AIM plays an important role in disease diagnosis and treatment, health management, and precision medicine which will greatly ease the tension of medical resources, adjust the medical service model, reduce the burden on doctors, and improve service efficiency (Figure 2).
Figure 2 The applications of AIM.
Although AI has taken a leap forward in medicine, there are still some dilemmas existing in clinical practice (Table 1). In fact, the key point for AIM applied to clinical practice is confidence. The first crisis of confidence comes from the diagnostic reliability, which needs a standard evaluation system to evaluate the performance of AIM in clinical applications. The second crisis of confidence comes from moral ambiguity, which needs to define the fault principle to eliminate the concerns of patients. In addition, data security is the third crisis of confidence. AIM usually generates personal health and medical information to make clinical decisions. Although the information is highly private, patients still worry about data breaches. The most noteworthy crisis of confidence is the lack of human–machine interaction which makes it hard to build an effective doctor–patient relationship. Thus, clinicians tend to be very careful when relying on AIM to make clinical decisions and patients tend to not trust the role of AIM.
Table 1 The Risks and Potential Solution of AIM
| The Risks of AI | Potential Solution | |
|---|---|---|
| Ethics related | Lack of moral subject status | Ethics Guidelines for Artificial Intelligence (2017) |
| Data breach | Interpreting machine learning models: Surrogate models | |
| Black box (diagnostic opacity) | Local interpretable model–agnostic explanations (LIME) | |
| Data correlation | Inconsistency of data quality | Develop specific data collection standards |
| Algorithmic discrimination | Clinician reviews input data | |
| Diagnostic related | Lack of doctor–patient communication | Choose more objective and interactive algorithms |
Will AI make clinicians obsolete?
With the rapid development of AI, the muddled relationship between clinicians and AI has become an issue. Some experts believe that AI may reduce the need for clinicians in medicine in the future as AI is proven to be more accurate than clinicians in diagnosis [9]. However, the overwhelming majority are convinced that clinicians will always be needed [10, 11]. Patients may be reluctant to trust AI recommendations or outcomes if sufficient evidence has not yet been gathered to demonstrate its efficacy for their particular medical condition. As mentioned already, mutual trust is a prerequisite for building effective doctor–patient relationship, which calls for empathy, creativity, and judgment, whereas AI cannot converse or interact with patients to create trust.
Building a harmonious doctor–patient relationship is not merely rhetoric, but it is related to the correctness and reasonableness of medical decisions, and even patients’ lives. Firstly, in the treatment of various complex and difficult diseases, human decision-making not only considers whether it is effective, but sometimes also considers non-disease factors such as economic conditions, a patient’s feelings, and the choice of family members. A deep understanding of the needs of patients and their families is essential. However, AI lacks human emotion, communication, and empathy, which results in indifference in relaying sensitive results to patients. Therefore, AI is not sophisticated enough to make diagnoses unaided by human intervention. Secondly, clinicians should, as information specialists, be able to steer the use of AI and guide the application of medical information to improve patient care [12]. In addition , because the clinical decisions made by AI are based on established knowledge and rules and the diseases are ongoing, clinicians need to evaluate the accuracy of such decisions to avoid the occurrence of misdiagnosis.
To date, AIM works in supplementing or augmenting the decision-making process of clinicians. AI is equivalent to an efficient aid, helping clinicians focus, which can shorten screening time and alleviate certain burdens. Clinicians may then be free to tackle more holistic tasks, representing an improved use of human capital. Studies have demonstrated a synergistic effect when clinicians and AI work together, producing better results than either alone. AI-based technologies could also augment real-time clinical decision-making, resulting in improved efforts toward precision medicine.
In fact, clinicians arrive at the diagnosis and treatments by not only relying on their own expertise in the field, but by integrating the diagnosis of multiple departments to make an accurate diagnosis. For example, the clinical manifestations of a patient may be partially non-specific, and the diagnosis made at that time would not be completely correct. The accuracy of said diagnosis would be greatly improved when combined with other examination findings. AIM provides greater computing power to assist clinicians focusing on the integration of gene therapy, medical imaging, pathology, and other information, all in an effort to help clinicians perform their tasks more effectively.
Will clinicians become just a data provider?
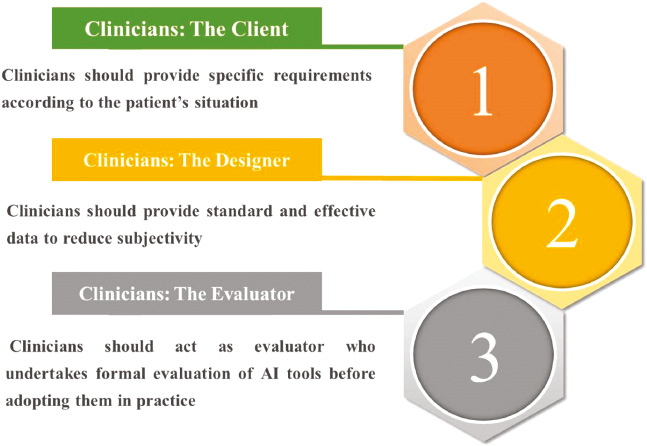
The primary goal of AIM is to allow clinicians to do less routine tasks and focus on more complex research to promote the development of medicine. In order to successfully integrate AI into medicine, the positionality of AIM and clinicians needs to be determined. Henceforth, clinicians need to be transformed from “operators” into “thinkers”. Clinicians have the greatest advantage in making accurate clinical diagnoses based on data [13]. Judgment is developed not only from knowledge gained from clinical practice, but also from years of medical training. Although clinicians can comprehend this idea, some may not know how to embrace the inclusion of AI, similar to society embracing the digital world in the 21st century. With that in mind, we will explore three major roles for clinicians in the age of AI (Figure 3).
Figure 3 Three major roles of clinicians in the age of AI.
Clinicians: The client
By using computer algorithms to extract useful information from massive clinical data, AIM could be applied to clinical diagnosis, which can assist clinical decision-making and promote diagnostic accuracy. However, medicine is a complex field where different diseases might exhibit similar patterns of lesions. This poses a great challenge for even the most advanced engineering expert to decipher normal physiological structures, disease pathogenesis, and clinical diagnosis processes. It is worth noting that the development of AIM should be based on clinical needs. For example, if a liver ultrasound demonstrates lesions, but other clinical features did not describe cancerous features, AI’s comprehensive information processing to predict the likelihood of an individual’s cancer is useful for clinicians to arrive at a diagnosis and treatment plan. For patients, the fundamental question facing the diagnostic interface may not be “Can this machine understand me”, but rather “Do I want this machine to understand me?” Will patients be willing to share information with a machine? Are they willing to let a machine break the news that they have cancer, no matter how appropriate the machine’s emotional simulation is at the time? Effective communication requires doctors to carefully assess the patient’s hopes, fears, and expectations, most of which are unspoken. Some patients may withhold information, which will affect the doctor’s diagnosis and treatment. Only an experienced doctor can root out the real underlying problems of the patient. Such complicated interactions could not be copied by mere algorithms. More importantly, the same treatments will change due to differences in physical fitness. The so-called personalized cancer therapy is utilized to decide which treatment method can be used to improve the cure rate according to the patient’s autoimmune function, the location of the tumor, and the pathological type. Therefore, clinicians should provide specific requirements according to the patient’s condition, while AIM needs to make corresponding changes according to the individualized requirements to achieve personalized treatments. This pattern provides opportunities to build bridges between clinicians and engineering experts. In this way can we centralize all the information to improve diagnostic accuracy and maximize the effect of integration.
Clinicians: The designer
Here, the role of clinicians is to maintain their clinical expertise and guard against the pitfalls of over-reliance on technology. The ultimate goal of an AI algorithm is to solve clinical problems in clinical practice, as evaluated by clinicians. It is impossible for engineering experts to take into account every single clinical problem. Thus, it is necessary for clinicians to help engineering experts to overcome clinical problems to enhance the accuracy of AI algorithms. Besides, high quality data is conducive to the construction of an AI system with high diagnostic accuracy. For example, if a patient was shown to have an opaque density on X-ray imaging, it is likely to cause the system to have a wrong perception, assuming that the object is a lesion, which will result in a large number of misdiagnoses in clinical applications. In another example, ultrasound scans could have a mirror effect, where a parenchymal tumor or the presence of fluid could be displayed on both sides of the diaphragm. In this case, the AI might misdiagnose this patient as having two tumors. In addition, natural language processing technology has been used for clinical intelligent diagnosis based on Chinese text-based electronic medical records (EMR), in which medical experts need to make a unified annotation of medical record information before the medical record information can be converted into a language that is recognizable by the AI. In this process, it is equivalent to strict re-screening of information by medical experts, and finally the input of qualified data can realize the intelligent diagnostic assistance of the AI. Thus, clinicians should provide standard and effective data to reduce subjectivity so as to build models with high diagnostic accuracy. Meanwhile, due to the scientific and vigorous nature of guidelines based on evidence-based medicine, guideline-based AIM can be truly effective. If AIM is developed without guidelines, the results obtained would not be consistent with the reality of clinical medicine, which would undoubtedly be a waste of resources. After establishing these models, clinicians need to design validation schemes, analyze experimental results, and draw conclusions. Therefore, clinicians should cooperate with engineering experts and play their role as designers to participate in the formulation of artificial intelligence research programs and make constructive suggestions. In addition, patients may also report inaccurate or irrelevant information, including exaggeration or even lies, where doctors are more likely to recognize the authenticity of information. In the human–AI diagnostic interface, doctors play an important role as “humans” to understand a patient’s illness and input accurate data into the computerized system.
Clinicians: The evaluator
At present, while the updating speed of medical AI products is very fast, the application of AI products still needs to be strictly checked. It should be emphasized that establishing intelligent algorithms in clinical practice requires rigorous validation. For example, it is reported that Watson’s suggestions are consistent with the Cancer Committee in 93% of breast cancer cases, at least in laboratory conditions [14]. However, the suitability of an AI model for training data is often highly optimistic and does not reflect its late performance on unseen data. Thus, clinicians must act as evaluators who perform formal evaluation of AI tools before adopting them in practice. For example, before AIM is adopted in clinical practice, the validation of the AIM must be evaluated, such as training cohorts (data quality, sample size, etc.) and algorithms. AI algorithms are developed using high quality data. If the training data is not comprehensive, the algorithms may provide unexpected results. Bias in the training data is a common phenomenon. Some examples of areas of possible bias include differences in patient populations, types of equipment, imaging parameters used, and the lack of representation of rare diseases [15]. Biased data will result in the failed generation of AI algorithms. Consequently, it is imperative for clinicians to evaluate the performance of AI algorithms based on the origins of the data. After AI has been put into clinical use, clinicians should also give feedback on the performance of the AI products to help with their improvement. Therefore, clinicians should utilize medical evaluation metrics to assess the performance of AIM, such as sensitivity, specificity, reproducibility, and consistency. It is noteworthy that the metric of accuracy is subjective and that clinicians believe the reproducibility and consistency are more reliable. If the results of such evaluations were provided to regulatory agencies, it could provide the basis for the post-marketing surveillance of AI, and ultimately, improved technologies, and performance.
In terms of the current developmental situation, AIM can enhance basic medical institutions through Internet-based services to improve diagnostic accuracy, ensuring that patients receive high-quality, locally-based medical services and thus reducing the economic burden of medical care. It is important to understand that both AIM and clinicians have limitations, and overcoming these limitations requires a joint effort. Medical AI needs to be further evaluated by clinicians before practical application, and should be optimized according to the feedback of clinicians in order to create new diagnosis and treatment models.
Conclusion
The vast majority of medical AI is in the research stage, but only a few AI products are currently used in clinical practice. One of the main reasons is that AI has an inexplicable nature in the process of decision-making. People are unclear as to what information AI uses to make decisions, thus reducing the trust of clinicians in decision-making. Although AI has advantages in data processing and analysis, its development is based on clinical problems, which are usually found by clinicians. In addition, the relationship between clinicians and patients is currently irreplaceable by AI. Clinicians need not fear AI but should gradually adapt to it while retaining their own services for cognitively challenging tasks. Thus, AI does promise a revolution that is likely to come about more effectively only when humans and AI work hand-in-hand in a synergistic manner.
Acknowledgments
This work was supported by the Scientific and Technological Livelihood Projects of Liwan District (201904003), Youth Foundation of Scientific Research of The Third Affiliated Hospital of Guangzhou Medical University (No. 2018Q18).
References
- Yu KH, Zhang C, Berry GJ, Altman RB, Ré C, et al. Predicting non-small cell lung cancer prognosis by fully automated microscopic pathology image features. Nat Commun 2016;7:12474. [PMID: 27527408 DOI: 10.1038/ncomms12474]
- Anthimopoulos M, Christodoulidis S, Ebner L, Christe A, Mougiakakou S. Lung pattern classification for interstitial lung diseases using a deep convolutional neural network. IEEE Trans Med Imaging 2016;35:1207-16. [PMID: 26955021 DOI: 10.1109/TMI.2016.2535865]
- Strickland E. IBM Watson, heal thyself: how IBM overpromised and underdelivered on AI health care. IEEE Spectrum 2019;56:24-31. [DOI: 10.1109/MSPEC.2019.8678513]
- Shen D, Wu G, Suk H-I. Deep learning in medical image analysis. Annu Rev Biomed Eng 2017;19:221-48. [PMID: 28301734 DOI: 10.1146/annurev-bioeng-071516-044442]
- Esteva A, Kuprel B, Novoa RA, Ko J, Swetter SM, et al. Dermatologist-level classification of skin cancer with deep neural networks. Nature 2017;542:115-8. [PMID: 28117445 DOI: 10.1038/nature21056]
- Setio AAA, Ciompi F, Litjens G, Gerke P, Jacobs C, et al. Pulmonary nodule detection in CT images: false positive reduction using multi-view convolutional networks. IEEE Trans Med Imaging 2016;35:1160-9. [PMID: 26955024 DOI: 10.1109/TMI.2016.2536809]
- Lee H, Tajmir S, Lee J, Zissen M, Yeshiwas BA, et al. Fully automated deep learning system for bone age assessment. J Digit Imaging 2017;30:427-41. [PMID: 28275919 DOI: 10.1007/s10278-017-9955-8]
- Manyika J, Chui M, Brown B, Bughin J, Dobbs R, et al. Big Data: The Next Frontier for Innovation, Competition, and Productivity. Available from: https://www.mckinsey.com/business-functions/mckinsey-digital/our-insights/big-data-the-next-frontier-for-innovation [Last accessed on June 2020].
- Tang X, Wang B, Rong Y. Artificial intelligence will reduce the need for clinical medical physicists. J Appl Clin Med Phys 2018;19:6-9. [PMID: 29333732 DOI: 10.1002/acm2.12244]
- Goldhahn J, Rampton V, Spinas GA. Could artificial intelligence make doctors obsolete? BMJ 2018;363:k4563. [PMID: 30404897 DOI: 10.1136/bmj.k4563]
- Mittelman M, Markham S, Taylor M. Patient commentary: stop hyping artificial intelligence-patients will always need human doctors. BMJ 2018;363:k4669. [PMID: 30404859 DOI: 10.1136/bmj.k4669]
- Jha S, Topol EJ. Adapting to artificial intelligence: radiologists and pathologists as information specialists. JAMA 2016;316:2353-4. [PMID: 27898975 DOI: 10.1001/jama.2016.17438]
- Liew C. The future of radiology augmented with artificial intelligence: a strategy for success. Eur J Radiol 2018;102:152-6. [PMID: 29685530 DOI: 10.1016/j.ejrad.2018.03.019]
- Somashekhar SP, Sepúlveda MJ, Puglielli S, Norden AD, Shortliffe EH, et al. Watson for oncology and breast cancer treatment recommendations: agreement with an expert multidisciplinary tumor board. Ann Oncol 2018;29:418-23. [PMID: 29324970 DOI: 10.1093/annonc/mdx781]
- Rubin DL. Artificial intelligence in imaging: the radiologist’s role. J Am Coll Radiol 2019;16:1309-17. [PMID: 31492409 DOI: 10.1016/j.jacr.2019.05.036]